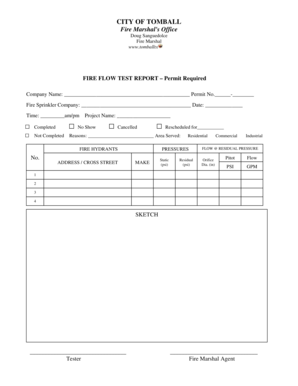
Humana Claim Reconsideration Form
Video Tutorial How to Fill Out humana claim reconsideration form
Thousands of positive reviews can’t be wrong
Read more or give pdfFiller a try to experience the benefits for yourself
Questions & answers
How do I get reimbursed from Humana?
Claim payment If you paid for services from your provider, ask us to reimburse you. You may request reimbursement by mailing a copy of your Humana member ID card and the provider's bill to the claims address written on the back of your card. Make sure the bill shows the patient's name and Humana member ID number.
How do I correct MyHumana claim?
Call Humana's provider call center at 800-457-4708. Record the reference number issued to you by the call center. If your issue is not resolved by the call center representative, you can ask for a supervisor. In some situations, the call center representative will route your issue to an internal team at Humana.
Does Humana follow Medicare billing guidelines?
We also align our system with other sources, such as, Centers for Medicare & Medicaid Services (CMS) guidelines, correct-coding initiatives, Humana policy, national benchmarks and industry standards.
How do I file an appeal with Humana Medicare?
How can I submit a grievance request? Fax number: 1-855-251-7594. Mailing address: Humana Grievances and Appeals. P.O. Box 14165. Puerto Rico members: Use the following form and fax and/or mailing address: Appeal, Complaint or Grievance Form – English. Fax number: 1-800-595-0462. Mailing address: Humana Puerto Rico.
How do you get Humana era?
You can access your ERA through your clearinghouse or through the secure provider tools available at Availity Essentials . Fees may be associated with ERA transactions. Check with your clearinghouse for specific rates.
Which processes claims for providers?
Healthcare providers transmit their medical claims to a clearinghouse. Clearinghouses then scrub, standardize and screen medical claims before sending them to the payor. This process helps mitigate errors in medical coding and reduces the time to receive provider reimbursement.
Related templates