Last updated on Apr 3, 2026

Get the free Opana Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

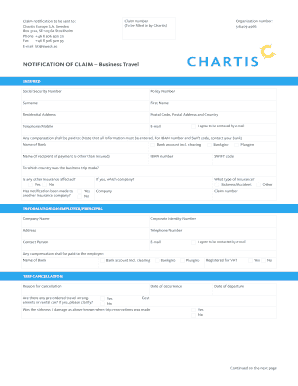
What is opana prior authorization form
The Opana Prior Authorization Form is a healthcare document used by physicians to request coverage for the medication Opana (oxymorphone) for patients experiencing moderate to severe pain.
pdfFiller scores top ratings on review platforms




Who needs opana prior authorization form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to opana prior authorization form
What is the Opana Prior Authorization Form?
The Opana Prior Authorization Form serves a critical function in the healthcare system, allowing physicians to request coverage for oxymorphone, a key medication used in pain management. This form is paramount for patients suffering from moderate to severe pain, as it facilitates necessary treatment and medication access. With this form, healthcare providers can ensure that patients receive the appropriate therapeutic options tailored to their needs.
Purpose and Benefits of the Opana Prior Authorization Form
The primary purpose of the Opana Prior Authorization Form is to provide healthcare providers with a structured means to gain approval for oxymorphone prescriptions. Physicians rely on this form to document medical necessity and to streamline the approval process for necessary medications. For patients, the benefits extend beyond mere access; it also increases the likelihood of receiving effective pain management through insurance coverage.
Key Features of the Opana Prior Authorization Form
This form is organized into several sections that capture essential information. Typical sections include:
-
Patient information
-
Physician details
-
Documentation of prior therapies
Optional fields and checkboxes address specific medical conditions or circumstances, ensuring that each submission is tailored to the patient's unique situation. The form accommodates diverse healthcare needs, enhancing the overall efficiency of care delivery.
Who Needs the Opana Prior Authorization Form?
The Opana Prior Authorization Form is particularly relevant for healthcare providers who prescribe oxymorphone. This includes a range of medical professionals such as primary care physicians, pain specialists, and oncologists. Prior authorization is necessary in situations where insurers need to verify that the medicine aligns with their coverage criteria, ensuring both compliance and patient safety.
How to Fill Out the Opana Prior Authorization Form Online (Step-by-Step)
Filling out the Opana Prior Authorization Form online is straightforward when following these steps:
-
Access the form through the designated platform.
-
Input patient information in the specified fields.
-
Complete the physician information section.
-
Document any previous treatments and the results.
-
Review all fields for completeness and accuracy.
-
Submit the form electronically or prepare it for mailing.
Pay particular attention to any blank fields and optional checkboxes to ensure all relevant information is captured.
Common Errors when Filling Out the Opana Prior Authorization Form
Physicians may encounter various pitfalls while completing the Opana Prior Authorization Form. Common errors include:
-
Leaving mandatory fields blank
-
Submitting incomplete information regarding prior treatments
To avoid these mistakes, doctors should double-check that all sections are filled out completely and that any claims made are thoroughly documented. This diligence prevents unnecessary delays in the approval process.
Submission Methods for the Opana Prior Authorization Form
Once the Opana Prior Authorization Form is completed, several submission methods are available:
-
Electronic submission through an insurance portal
-
Mailing a hard copy to the designated insurance provider
Each method may come with specific deadlines for review and approval, and it’s critical to be aware of these timelines to ensure timely processing.
What Happens After You Submit the Opana Prior Authorization Form?
Following submission, the form undergoes a review process by Coventry Health Care. Possible outcomes include:
-
Approval of medication
-
Denial with reasons provided
-
Request for further information from the prescriber
Understanding these outcomes can help physicians prepare for next steps and facilitate patient care accordingly.
Security and Compliance when Using the Opana Prior Authorization Form
Handling sensitive patient information is of utmost importance when using the Opana Prior Authorization Form. It is essential to apply secure practices throughout the process. pdfFiller offers robust security features, including 256-bit encryption, to ensure compliance with HIPAA and GDPR standards, protecting user data effectively.
Maximize Your Experience with pdfFiller for the Opana Prior Authorization Form
pdfFiller enhances the process of completing and submitting the Opana Prior Authorization Form with its user-friendly platform. Key features include eSigning and editing capabilities, making the form-filling experience more efficient and effective. Users are encouraged to leverage these tools to streamline the completion process, ensuring a smooth operational experience.
How to fill out the opana prior authorization form
-
1.Access the Opana Prior Authorization Form by visiting pdfFiller and searching for the form by its name.
-
2.Open the form once located; review the fields that need completion to ensure you have the necessary information.
-
3.Before you begin filling out the form, gather required patient information including details about their pain management history and trials of previous medications.
-
4.Begin completing the form by addressing the blank fields, ensuring accurate patient and physician information is entered, including signatures where required.
-
5.Utilize pdfFiller’s interface to check off options, fill in text boxes, and provide necessary details as indicated in the form's instructions.
-
6.After completing the form, review it thoroughly for any omissions or errors—double-check all patient details and submission requirements.
-
7.Finalize the form by saving your work through the save option, and if ready to submit, use pdfFiller's options to download or send it directly to Coventry Health Care.

Who is eligible to use the Opana Prior Authorization Form?
Physicians prescribing Opana for patients suffering from moderate to severe pain are eligible to utilize this form to request authorization from Coventry Health Care.
What supporting documents are required when submitting the form?
Supporting documents typically include patient medical records and documentation of previously attempted treatments or medications in accordance with the World Health Organization analgesic ladder.
How should the completed Opana form be submitted?
The completed Opana Prior Authorization Form should be submitted directly to Coventry Health Care, either through electronic submission via pdfFiller or by printing and mailing it.
What are common mistakes to avoid when filling out the form?
Common mistakes include forgetting to sign the document, leaving required fields blank, and failing to provide adequate documentation of prior therapies.
Are there any deadlines for submitting the Opana Prior Authorization Form?
While specific deadlines may vary based on individual insurance policies, it is best to submit the form as soon as possible following the decision to prescribe Opana to avoid delays in treatment.
What is the processing time for the Opana Prior Authorization request?
Processing times can vary but typically take several business days. It's advisable to follow up with Coventry Health Care to confirm receipt and get updates on status.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.