Last updated on Apr 3, 2026

Get the free Medicare Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

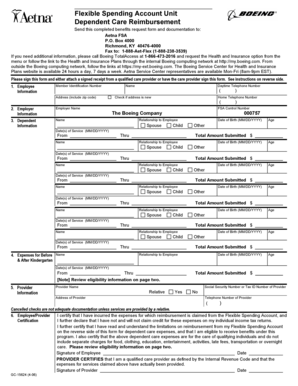
What is medicare prior authorization form
The Medicare Prior Authorization Form is a healthcare document used by patients and providers to request prior authorization for specific medications and treatments under Medicare Part B and D.
pdfFiller scores top ratings on review platforms




Who needs medicare prior authorization form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to medicare prior authorization form
What is the Medicare Prior Authorization Form?
The Medicare Prior Authorization Form is a vital document used to request approval for specific medications and treatments under Medicare Part B and D. This form plays a significant role in the healthcare process by ensuring that patients receive necessary services that conform to Medicare guidelines. Certain medications, such as immunosuppressants and oral chemotherapy agents, require prior authorization, which emphasizes the importance of this form in both patient care and provider compliance.
Purpose and Benefits of the Medicare Prior Authorization Form
This form is essential in streamlining access to needed treatments and medications. By facilitating a clear communication channel between healthcare providers and Medicare, it helps ensure that prescribed services adhere to guidelines, which can prevent unnecessary denials. The benefits include enhanced patient access to care, reduced medical costs, and improved treatment outcomes, which are crucial for both patients and providers.
Who Needs the Medicare Prior Authorization Form?
Typically, patients prescribed specific medications or treatments and their healthcare providers need to complete the Medicare Prior Authorization Form. This form is relevant in various contexts, including scenarios where certain treatments are clinically necessary but are subject to Medicare's review process. Individuals managing chronic conditions or requiring ongoing care often find this authorization process essential.
How to Fill Out the Medicare Prior Authorization Form Online
Filling out the form online can be a straightforward process. Here are the steps to complete it digitally:
-
Access the digital form through a reputable platform.
-
Enter patient and physician information accurately.
-
Select the appropriate medications and treatments needing authorization.
-
Review the filled sections for accuracy.
-
Submit the form electronically.
Be sure to leverage tools that provide guidance on navigating specific fillable fields and checkboxes.
Required Documents and Supporting Materials
When submitting the Medicare Prior Authorization Form, additional documents may be necessary to support the request. These may include:
-
Patient's medical history and current treatment details.
-
Prescriptions from the healthcare provider.
-
Any relevant test results or clinical notes.
Accuracy and completeness in the submitted documentation are critical to ensure prompt processing and approval.
Submission Methods and Delivery
There are various options available to submit the completed Medicare Prior Authorization Form. These methods include:
-
Online submission through secure platforms.
-
Faxing the completed form to the appropriate Medicare office.
-
Mailing the form directly to the specified Medicare address.
Tracking confirmations of receipt and processing times is pivotal, especially when using online submission methods, which tend to be faster and more reliable.
Common Errors and How to Avoid Them
Common mistakes while completing the Medicare Prior Authorization Form can lead to delays. Here are frequent pitfalls to watch for:
-
Incomplete or incorrect patient information.
-
Failure to select the necessary medications or treatments.
-
Omitting required supporting documents.
To avoid these issues, double-check all entries and utilize a review and validation checklist before submission.
What Happens After You Submit the Medicare Prior Authorization Form?
Once submitted, the Medicare review process begins. Patients will be notified about their authorization status via:
-
Mail correspondence from Medicare.
-
Direct communication from the healthcare provider.
If a request is rejected or additional information is needed, it's essential to understand how to address these issues promptly to avoid further delays in necessary treatments.
Security and Compliance for the Medicare Prior Authorization Form
Security measures are critical for the protection of personal health information when handling the Medicare Prior Authorization Form. Ensuring compliance with HIPAA and GDPR is vital in safeguarding sensitive documents. Utilizing secure platforms for submission and storage helps maintain the integrity and confidentiality of patient data.
Leverage pdfFiller for Your Medicare Prior Authorization Form Needs
Utilizing pdfFiller makes it easier to manage and fill out the Medicare Prior Authorization Form. Features such as eSigning, document sharing, and template creation enhance the user experience, providing a trusted means for processing sensitive documents efficiently.
How to fill out the medicare prior authorization form
-
1.To access the Medicare Prior Authorization Form on pdfFiller, visit the pdfFiller website and search for the form by name in the search bar. Once located, click on it to open.
-
2.Navigate the form interface by using the toolbar on the right side to add text in the required fields. You can click on any fillable field to start entering your information.
-
3.Before filling out the form, gather necessary details like patient information, physician details, relevant medical history, and the specific medication or treatment needing authorization.
-
4.Proceed through the form by filling in each section. Make sure to check all checkboxes and provide any additional required information to avoid delays.
-
5.Once you have filled in all sections, carefully review the form for any errors or omissions. Utilize the built-in spelling checker provided by pdfFiller.
-
6.To finalize your completed form, save it by clicking the 'Save' button at the top of the screen. You can also download a copy to your device for your records.
-
7.If you are ready to submit, select the submission method that suits your needs, whether it’s email, fax, or print. Follow the prompts to complete the submission via pdfFiller.

Who is eligible to use the Medicare Prior Authorization Form?
Any patient covered under Medicare who requires authorization for specific medications and treatments is eligible to use the Medicare Prior Authorization Form.
What is the typical processing time for authorization requests?
Processing times for Medicare prior authorization requests can vary, but it typically takes about 7-14 business days to receive a response after submission.
What information do I need before completing the form?
Before completing the form, ensure you have the patient’s personal details, prescribing physician’s information, any required medical documentation, and specifics about the medication or treatment being requested.
How do I submit the completed Medicare Prior Authorization Form?
After filling out the form on pdfFiller, you can submit it electronically via email or fax, or print it out to mail it directly to the appropriate Medicare administrative contractor.
Are there common mistakes to avoid when filling out the form?
Yes, common mistakes include leaving required fields blank, submitting incomplete information, or failing to include necessary supporting documents. Double-check all entries before submission.
Is notarization required for the Medicare Prior Authorization Form?
No, notarization is not required for the Medicare Prior Authorization Form, but ensure all requested signatures are present before submitting.
What should I do if my authorization request is denied?
If your authorization request is denied, you can appeal the decision by following the guidelines provided in the denial notice, which typically includes submitting additional documentation or rationale.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.