Last updated on Apr 3, 2026

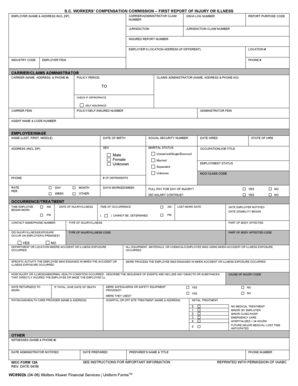
Get the free Member Submitted Claim Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is member submitted claim form
The Member Submitted Claim Form is a healthcare document used by patients to submit claims for medical, vision, and dental services when providers have not billed their insurance directly.
pdfFiller scores top ratings on review platforms




Who needs member submitted claim form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to member submitted claim form
What is the Member Submitted Claim Form?
The Member Submitted Claim Form is an essential document in the healthcare reimbursement process, specifically utilized for filing medical, vision, and dental claims. This form serves as a means for patients to submit expenses incurred when providers do not bill their health plan directly. It is particularly important for patients needing reimbursement for out-of-pocket expenses, ensuring that they can recover costs related to their healthcare.
Patients should understand when to use this form as opposed to relying on provider-billed claims, which are handled directly by the healthcare provider. The Member Submitted Claim Form plays a vital role in facilitating communication between the patient and the insurance provider regarding the eligibility and reimbursement of medical costs.
Purpose and Benefits of the Member Submitted Claim Form
The primary purpose of the Member Submitted Claim Form is to enable patients to seek reimbursement for their healthcare expenses incurred out-of-pocket. Utilizing this form streamlines the claims process, allowing patients to efficiently receive funds owed to them. This form is particularly beneficial for services that may not be billed directly to the insurer.
Using the Member Submitted Claim Form enhances convenience; patients can easily compile their expenses and submit them for review without navigating long processes typically associated with non-direct billing scenarios. The added efficiency offered by this form empowers patients towards maximizing their healthcare reimbursements.
Who Needs the Member Submitted Claim Form?
The Member Submitted Claim Form is primarily needed by patients who have incurred medical expenses that require reimbursement. This includes individuals who may have received care from out-of-network providers or those who opted for services not directly billed by clinics or hospitals. This form is particularly relevant for residents of Washington state, who must comply with specific submission requirements to ensure compliance with local healthcare regulations.
Patients who have out-of-pocket expenses from services like emergency care or specialty services usually require this form to file a claim and obtain their rightful reimbursements.
How to Fill Out the Member Submitted Claim Form Online
Filling out the Member Submitted Claim Form online can be seamlessly accomplished using pdfFiller. Here are the steps:
-
Access the form via pdfFiller’s platform.
-
Complete the required fields such as patient details and itemized bills.
-
Ensure all parts of the form are accurately filled to avoid delays.
-
Utilize the fillable PDF features to streamline your completion process.
-
Add your electronic signature if required, ensuring compliance.
It’s crucial to double-check each section of the form for accuracy before submission to prevent common mistakes that could lead to potential reimbursement delays.
Required Documents and Supporting Materials for Your Claim
To successfully submit the Member Submitted Claim Form, you will need to provide several key documents:
-
Itemized bills detailing the services rendered.
-
Receipts from providers showing proof of payment.
-
Any additional supporting documentation that may expedite processing.
Each document plays a critical role in verifying the details of your claim, facilitating a smoother review process. Ensure you prepare these materials thoroughly to enhance the chances of a successful claim submission.
Where and How to Submit the Member Submitted Claim Form
The submission of the Member Submitted Claim Form can typically be done via postal mail, with clear instructions provided within the form itself. Some insurance providers may also allow for online submission, so checking available options is advisable.
When submitting your claim, be aware of any associated fees and the deadlines for submission. Tracking your claim submission and receiving confirmation can further ensure that your claim is processed promptly and accurately.
Common Errors to Avoid When Submitting the Member Submitted Claim Form
To minimize issues when submitting the Member Submitted Claim Form, be mindful of these common errors:
-
Missing signatures or necessary approvals.
-
Incomplete fields or missing documentation.
-
Failing to double-check information for accuracy.
Reviewing the claims form thoroughly before submission helps ensure that all necessary details are filled out correctly, preventing delays and facilitating a smooth claims process.
Security and Compliance When Filing Your Claim
When submitting your Member Submitted Claim Form, it is essential to be aware of the security measures that protect your sensitive health-related documents. pdfFiller employs 256-bit encryption and follows compliance standards to ensure data protection and confidentiality during the claims process.
Protecting your personal health information is paramount, and utilizing secure platforms guarantees the safety of your documents while navigating the claims process.
Maximize Your Claims Efficiency with pdfFiller
pdfFiller serves as an invaluable tool for users aiming to streamline their claims process. You can easily create, edit, and fill out the Member Submitted Claim Form through the platform. Additionally, features such as eSigning and document sharing enhance the overall user experience and workflow.
By leveraging pdfFiller for your healthcare reimbursement needs, you can benefit from efficiency and convenience in managing your claim submissions.
How to fill out the member submitted claim form
-
1.Access the Member Submitted Claim Form on pdfFiller by searching for its title in the platform’s search bar.
-
2.Open the form by clicking on it once it appears in search results.
-
3.Review the instruction sections of the form to familiarize yourself with the required information and steps.
-
4.Gather necessary documents including the itemized bill, patient information, and details of the claim you are submitting.
-
5.Start filling in the patient information fields including your name, contact details, and member identification.
-
6.Use the fillable fields to enter specifics about the medical services received such as dates of service and the nature of the treatment.
-
7.Attach the itemized bill by uploading it in the designated section and ensure all costs are clearly listed.
-
8.Carefully check each field to confirm that all information is accurate and complete, ensuring that mandatory fields are filled appropriately.
-
9.Once all fields are completed, review the form thoroughly for errors or missing information.
-
10.Finally, add your signature in the provided space using pdfFiller’s signature feature.
-
11.Save your filled form and consider downloading a copy for your records.
-
12.Submit the form by mailing it directly to Premera Blue Cross as per their submission guidelines.

Who is eligible to use the Member Submitted Claim Form?
This form is intended for patients who have incurred expenses from healthcare providers that did not bill directly to their insurance plan.
What documents do I need to submit with this form?
You need an itemized bill from the service provider, patient identification details, and any additional information about the treatment received.
How do I submit the completed form?
The completed form must be mailed to Premera Blue Cross for processing. Make sure to check the mailing address specified on the form.
Are there any deadlines for submitting this claim form?
While specific deadlines may vary, it’s advisable to submit the form as soon as possible after incurring expenses to avoid delays in reimbursement.
What are common mistakes to avoid when filling out the form?
Be careful to fill in all required fields accurately, ensure your signature is included, and double-check that the itemized bill is attached properly.
How long does it take to process the claim once submitted?
Claim processing times can vary, but typically, you should allow a few weeks for your claim to be reviewed and processed by Premera Blue Cross.
Is this form applicable for claims in states other than Washington?
No, this particular form is intended for use in Washington state. Different forms may be required for other locations.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.