Last updated on Apr 4, 2026

Get the free Drug Reimbursement Claim Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is drug reimbursement claim form
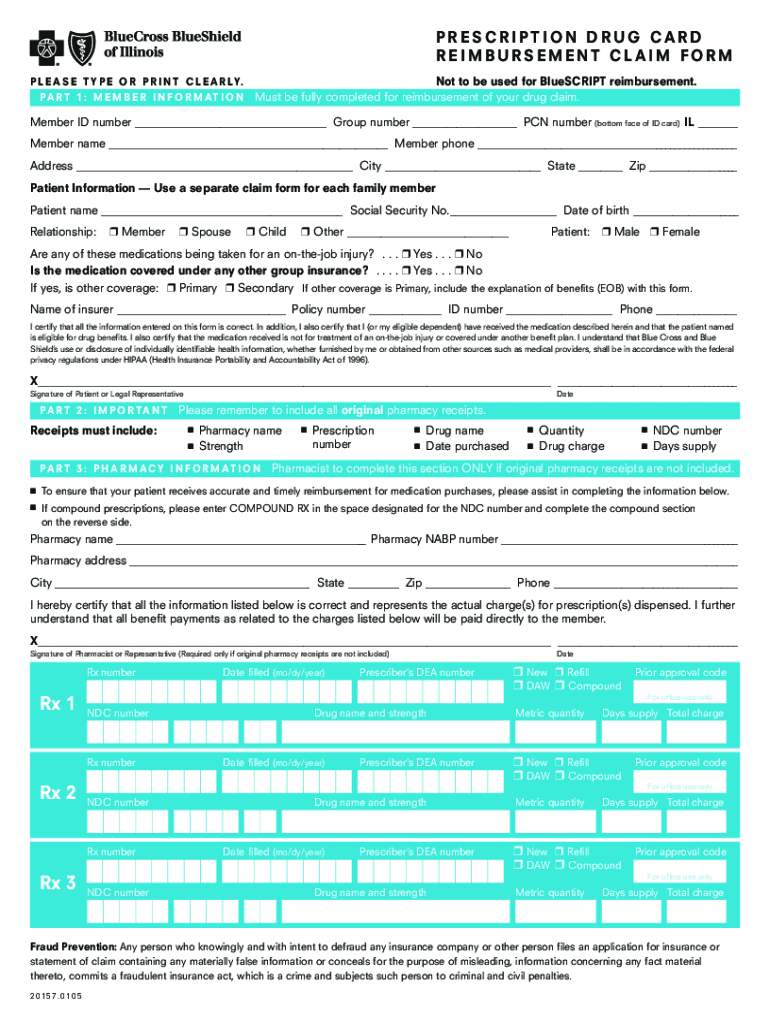
The Drug Reimbursement Claim Form is a Health Insurance Claim Form used by Blue Cross and Blue Shield of Illinois members to request reimbursement for prescription drug purchases.
pdfFiller scores top ratings on review platforms




Who needs drug reimbursement claim form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to drug reimbursement claim form
What is the Drug Reimbursement Claim Form?
The Drug Reimbursement Claim Form is a critical document for members of Blue Cross and Blue Shield of Illinois. This form is primarily used to request reimbursement for prescription drug purchases. It is essential to include original pharmacy receipts when submitting the claim. The process begins with filling out the form accurately, ensuring all necessary details are provided to facilitate a smooth reimbursement process.
Purpose and Benefits of the Drug Reimbursement Claim Form
The Drug Reimbursement Claim Form serves multiple purposes, primarily providing financial relief to members by ensuring they are reimbursed for out-of-pocket expenses. This streamlined process benefits both members and pharmacies, making it easier to manage claims and improve healthcare affordability. By utilizing this form, members can enhance their access to necessary prescription medications without significant financial burden.
Who Needs the Drug Reimbursement Claim Form?
The primary users of the Drug Reimbursement Claim Form include patients, legal representatives, and pharmacists. Patients or their representatives must be eligible to file the form, and in some situations, signatures from both parties are required. Understanding the eligibility criteria and the roles of each party is essential to ensure a successful claim submission.
How to Fill Out the Drug Reimbursement Claim Form: Step-by-Step Guide
Filling out the Drug Reimbursement Claim Form correctly is crucial for successful reimbursement. Follow these steps to complete the form:
-
Enter your Member ID prominently in the designated field.
-
Provide the pharmacy name where the medication was purchased.
-
Ensure the patient’s signature is included at the end of the form.
-
Double-check all information for accuracy to avoid common errors.
Pay particular attention to important fields as mistakes can delay your reimbursement process.
Required Documents and Supporting Materials
When submitting the Drug Reimbursement Claim Form, it’s important to include the necessary supporting documents. Required materials typically include:
-
Original pharmacy receipts detailing the prescription purchase.
-
Any additional documentation that may support your claim.
Organizing these materials before submission can significantly enhance the processing speed of your claim.
Submission Methods for the Drug Reimbursement Claim Form
Submitting the completed Drug Reimbursement Claim Form can be done through various methods. Options include:
-
Mailing the completed form to the specified address.
-
Utilizing electronic submission methods if available.
Be sure to pay attention to submission timelines to ensure your claim is processed promptly and effectively.
What Happens After Submitting the Drug Reimbursement Claim Form?
After submission, the claims undergo a review process. The approval process can yield different outcomes, affecting how and when funds are disbursed. You can check the application status through the provided methods, which may include follow-up correspondence or online status checks.
Maintaining Security and Compliance with Your Drug Reimbursement Claim Form
Security is paramount when handling your Drug Reimbursement Claim Form. It's crucial to utilize platforms that ensure compliance with regulations like HIPAA. Features such as encryption protect sensitive information, allowing you to submit claims with confidence.
Utilizing pdfFiller for an Efficient Claim Process
pdfFiller offers excellent capabilities for completing the Drug Reimbursement Claim Form. Users can fill, eSign, and submit forms directly through the platform, which can significantly save time and minimize errors. Additionally, support resources are available for those who need assistance during the process.
How to fill out the drug reimbursement claim form
-
1.Access the Drug Reimbursement Claim Form on pdfFiller by searching for the form name in the pdfFiller search bar or accessing the relevant healthcare forms category.
-
2.Open the form and navigate through the document using the scrolling feature. Take note of each field that requires input.
-
3.Before filling out the form, gather necessary information including your Member ID number, prescription details, and original pharmacy receipts to ensure accurate completion.
-
4.Start by entering your personal information in the designated fields. This usually includes your name, address, and any other applicable details.
-
5.Next, provide the relevant pharmacy information such as the pharmacy name and contact details, ensuring you spell correctly to avoid processing delays.
-
6.Fill in the section that requests details about the prescription drugs purchased. Include dates of purchase and medication names clearly.
-
7.Look for signature lines for both the patient and pharmacist. Ensure both signatures are included, as the form requires them for processing.
-
8.Carefully review the completed form for any inaccuracies or missing information, making necessary corrections before proceeding.
-
9.Once satisfied with the entries, save your work by using the 'Save' or 'Download' options on pdfFiller. You can also print a copy if needed.
-
10.Submit the form by mailing it to the address specified in the instructions accompanying the form. Ensure you include all required documentation like pharmacy receipts.

Who is eligible to use the Drug Reimbursement Claim Form?
The Drug Reimbursement Claim Form is designed for members of Blue Cross and Blue Shield of Illinois who have purchased prescription drugs and are seeking reimbursement.
What documents are required to submit this claim?
To submit the claim, you'll need to include original pharmacy receipts along with the completed claim form for processing.
What should I do if I miss a submission deadline?
If you miss a deadline for submitting your drug claim, contact Blue Cross and Blue Shield's customer service for guidance on possible remedies or extensions.
How can I track the status of my claims?
Typically, you can track the status of your claims by contacting customer support or checking through the Blue Cross Blue Shield of Illinois member portal online.
How long does it take to process the claim?
Claims processing time can vary but typically takes 4 to 6 weeks. Ensure all information is accurate to avoid delays.
What are common mistakes to avoid when completing the form?
Common mistakes include missing signatures, incorrect pharmacy details, or failing to include the original receipts. Double-check all information before submission.
Can a representative submit the form on my behalf?
Yes, a legal representative can submit the form, but it must include the necessary signatures from both the patient and the representative for validity.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.