Last updated on Apr 8, 2026

Get the free Routine Vision Member Claim Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is routine vision member claim
The Routine Vision Member Claim Form is a healthcare document used by members to submit claims for vision services received from out-of-network providers.
pdfFiller scores top ratings on review platforms




Who needs routine vision member claim?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to routine vision member claim
What is the Routine Vision Member Claim Form?
The Routine Vision Member Claim Form serves as a critical tool for members of the OptiCare Managed Vision network. Its primary purpose is to enable members to seek reimbursement for out-of-network vision services. This is particularly significant in North Carolina, where members may engage with providers not affiliated with their network. By utilizing the routine vision claim form, members can navigate the reimbursement process efficiently and effectively.
Benefits of Using the Routine Vision Member Claim Form
Submitting the Routine Vision Member Claim Form offers numerous advantages for members. It simplifies the process for claiming reimbursements for services rendered by non-network providers. Moreover, this form plays a vital role in ensuring that members can recover costs associated with vision care expenses, helping to manage their overall healthcare spending.
Key Features of the Routine Vision Member Claim Form
This claim form consists of several essential fields that must be completed for processing. Key elements include:
-
Member information: Name, date of birth, and member ID.
-
Provider details: Necessary information regarding the service provider.
-
Signature requirements: Members must sign and date the claim.
Additionally, members are required to attach itemized receipts or 'super bills' to substantiate their claims. This comprehensive structure ensures clarity and compliance during submission.
Eligibility Criteria for the Routine Vision Member Claim Form
To use the Routine Vision Member Claim Form, specific eligibility requirements must be met. Only members of the OptiCare Managed Vision network can submit this form. It is important to note that there may be restrictions on specific services covered, so members should review their plan details to avoid misunderstandings.
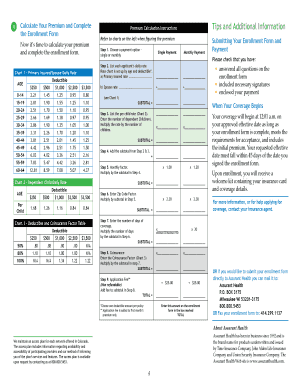
How to Fill Out the Routine Vision Member Claim Form (Step-by-Step Guide)
Filling out the Routine Vision Member Claim Form accurately is essential for successful processing. Follow these steps:
-
Enter member information: Include your full name, date of birth, and the UPMC for Life ID number.
-
Fill in provider details: Provide the name and contact information of the vision provider.
-
Sign and date: Ensure that you sign and date the claim form in the designated areas.
Completing these steps with attention to detail will facilitate a smoother claim submission process.
Submission Methods and Deadlines for the Routine Vision Member Claim Form
Members must adhere to specific submission guidelines for the Routine Vision Member Claim Form. Claims should be mailed directly to OptiCare Managed Vision located in Rocky Mount, NC. It is crucial to observe any deadlines for submission to ensure reimbursement claims are processed in a timely manner, thereby avoiding any potential delays.
Common Errors and How to Avoid Them
Understanding common mistakes can significantly improve your claim submission experience. Frequent errors include:
-
Omitting essential member or provider information.
-
Failing to sign or date the claim form appropriately.
To mitigate these issues, it is advisable to review the completed claim thoroughly before submission, confirming that all required details are included.
What Happens After You Submit the Routine Vision Member Claim Form?
Once you submit the Routine Vision Member Claim Form, a process is in place for monitoring the status of your claim. Members can expect to receive confirmation of receipt, and the outcome of the claim will be communicated promptly. Potential outcomes include either acceptance or rejection of the claim, depending on the information provided and adherence to guidelines.
Security and Compliance When Using the Routine Vision Member Claim Form
Data security is paramount when handling the Routine Vision Member Claim Form. pdfFiller employs robust measures to ensure sensitive information is managed securely. The platform complies with necessary privacy standards such as HIPAA and GDPR, providing members with peace of mind as they submit sensitive documentation.
Ready to Fill Out Your Claim Form?
Utilizing pdfFiller's services can enhance your experience in filling out the Routine Vision Member Claim Form. The platform offers an intuitive interface for filling, signing, and submitting your claim form efficiently. By leveraging a cloud-based service, members can benefit from organized document management and ease of use throughout the claims process.
How to fill out the routine vision member claim
-
1.To access the Routine Vision Member Claim Form, visit pdfFiller's website and search for the form by its name.
-
2.Open the form in pdfFiller and familiarize yourself with its layout, keeping an eye on the fillable fields available.
-
3.Before starting, gather essential information, including your NAME (LAST, FIRST, MI), DATE OF BIRTH, UPMC for Life ID #, and related provider details.
-
4.Click into each fillable field to input your information clearly, ensuring accuracy in each entry to avoid processing delays.
-
5.Refer to the instructions provided within the form to understand the sections that need to be completed and the specific details required.
-
6.Once all fields are filled, review the entire form for completeness and correctness, checking for any missing information or typos.
-
7.To finalize your claim, sign and date the form as required, ensuring that the signature matches your details.
-
8.Once satisfied, use pdfFiller's options to save and download a copy of the completed form for your records.
-
9.Lastly, submit the completed form along with any necessary supporting documents to OptiCare Managed Vision at their provided address.

Who is eligible to use the Routine Vision Member Claim Form?
The Routine Vision Member Claim Form is specifically for members of the OptiCare Managed Vision network who have received vision services outside of their network and wish to file a claim for reimbursement.
What documents do I need to submit along with this claim form?
In addition to the completed Routine Vision Member Claim Form, you must provide an itemized receipt or 'super bill' from the service provider, detailing the services rendered.
How do I submit the Routine Vision Member Claim Form?
After completing the form and attaching the necessary documents, you should mail it to OptiCare Managed Vision in Rocky Mount, NC. It's advisable to send it via a traceable mailing method for confirmation.
Is there a deadline for submitting the claims?
While the specific deadline isn't outlined in the form metadata, it's generally best to submit claims as soon as possible after receiving services to avoid potential delays in reimbursement.
What are common mistakes to avoid when filling out the claim form?
Common mistakes include missing signatures, incorrect personal information, and failing to provide an itemized receipt. Ensure all fields are filled accurately to facilitate smooth processing.
How long does it take to process my vision claim?
Processing times can vary, but typically, it may take several weeks for the insurance company to review and process your claim, depending on their workload and the completeness of your submission.
Can I track the status of my claim after submission?
Most insurance providers, including OptiCare Managed Vision, may offer a way to track the status of your claim. It's best to contact them directly for the most accurate information.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.