Last updated on Apr 18, 2026

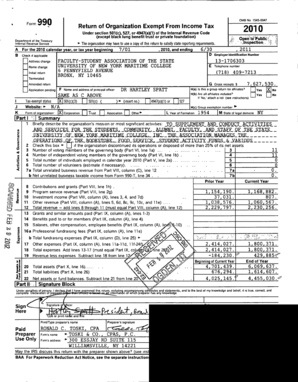
Get the free COBRA Continued Group Coverage Application
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is cobra continued group coverage
The COBRA Continued Group Coverage Application is a health insurance document used by employees in Alaska to extend their group health coverage after a qualifying life event.
pdfFiller scores top ratings on review platforms




Who needs cobra continued group coverage?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to cobra continued group coverage
What is the COBRA Continued Group Coverage Application?
The COBRA Continued Group Coverage Application is a crucial document for employees in Alaska who need to maintain their health coverage following qualifying events. These events include termination of employment, a reduction in hours, or retirement. Completing this application ensures that health coverage remains uninterrupted, which is pivotal for both the employees and their dependents during transitions.
After a qualifying event, applicants have a limited timeframe of 60 days to submit the COBRA application to their employers. This timely filing requirement is essential to activate the continuation of health benefits. Both employees and employers must complete this form to facilitate the smooth transition of coverage.
Purpose and Benefits of the COBRA Continued Group Coverage Application
Completing the COBRA application is vital for securing continued health insurance coverage. This process safeguards employees and their dependents from potential health risks associated with gaps in coverage. The financial security that stems from uninterrupted health insurance cannot be overstated, as it protects against unexpected medical expenses.
Additionally, employers have a legal obligation to inform their employees of COBRA rights, which includes providing a COBRA election form. Understanding these rights can significantly benefit employees in navigating their health coverage options while making informed choices about their future.
Eligibility Criteria for the COBRA Continued Group Coverage Application
To qualify for the COBRA Continued Group Coverage Application, employees must experience specific qualifying events. These events may include job loss due to layoffs, reduction in hours that affect eligibility, or retirement. Dependents of the employee can also be eligible for coverage, which extends various protections to families.
-
Qualifying events include termination of employment, reduction in work hours, or retirement.
-
Dependents may qualify for continued health coverage as well.
-
Typically, COBRA coverage can last up to 18 months after the application is submitted.
How to Fill Out the COBRA Continued Group Coverage Application Online (Step-by-Step)
Filling out the COBRA application is made easier with a clear understanding of its various fields. Key sections of the application include GROUP NAME, GROUP ID, and SUBGROUP ID, all of which require accurate information for processing.
-
Access the COBRA continued group coverage application form online.
-
Input the GROUP NAME, GROUP ID, and SUBGROUP ID accurately.
-
Ensure all required signatures are obtained from both the Applicant and the Employer.
-
Verify that you have gathered all necessary information before submission.
Common Errors and How to Avoid Them
When completing the COBRA application, it's crucial to be aware of common mistakes that could lead to application rejection or processing delays. Errors such as missing information or illegible handwriting can result in significant setbacks.
-
Double-check all filled fields for accuracy and completeness.
-
Ensure clarity in handwriting and avoid ambiguous answers.
Submission Methods for the COBRA Continued Group Coverage Application
Users have several options available for submitting their completed COBRA application. It is important to choose a method that is both secure and reliable. Common submission methods include sending the form via email or physical mail to the employer.
-
Acceptable submission methods include email and physical mail.
-
Keep records of the submission for tracking purposes.
-
Check if there are any associated fees or additional documentation required with the application.
What Happens After You Submit the COBRA Continued Group Coverage Application?
After submitting the COBRA application, the processing time can vary based on employer protocols. Applicants should expect to receive confirmation once their application is received.
-
Employers will process applications and confirm their receipt.
-
Status checks can be conducted to ensure application progress.
-
Be prepared to address potential rejection scenarios and understand the reasons for rejections.
How pdfFiller Can Help You Complete the COBRA Continued Group Coverage Application
pdfFiller is an excellent tool for those looking to streamline the process of completing the COBRA application. With features such as cloud-based editing and eSigning capability, users can manage their applications efficiently.
Security is a priority, especially when dealing with sensitive health documents. pdfFiller ensures that all user data is protected, making it a trustworthy platform for managing your COBRA continued group coverage application.
How to fill out the cobra continued group coverage
-
1.Access pdfFiller and search for 'COBRA Continued Group Coverage Application'. Open the form in your browser.
-
2.Navigate through the form using your cursor. Click on each fillable field available for data entry.
-
3.Before starting, gather essential information like group name, group ID, and any details about the qualifying event.
-
4.Carefully fill in all required information, ensuring accuracy for each applicant and dependent listed.
-
5.Use checkboxes to select applicable COBRA coverage options. Make sure all necessary selections are made.
-
6.Review the completed form for any errors or missing information to ensure it is fully completed.
-
7.Once satisfied with the filled form, save your changes within pdfFiller.
-
8.Download the completed form for your records and submission purposes, or submit it directly to the employer using the provided submission options.

Who is eligible to use the COBRA Continued Group Coverage Application?
Any employee in Alaska who has experienced a qualifying event, such as termination, reduction in hours, or retirement, may use the COBRA Continued Group Coverage Application to extend their health coverage.
What is the deadline for submitting this application?
You must complete and return the COBRA Continued Group Coverage Application to your employer within 60 days of the qualifying event or notification of COBRA rights.
How should I submit the completed application form?
Once completed, you can submit the COBRA application to your employer. Depending on their process, it may be submitted electronically via pdfFiller or printed and delivered physically.
What supporting documents are required with the COBRA application?
Generally, no specific supporting documents are required alongside the COBRA application itself, but it may help to include any relevant documentation regarding the qualifying event.
What common mistakes should I avoid when filling out this form?
Ensure all required fields are filled accurately, including names, group information, and event details. Double-check for any misspellings or omitted sections before submission.
How long does it take to process the COBRA application?
Processing times can vary based on the employer's policies. Typically, expect a response within a few business days after they receive your completed application.
Is there a fee associated with extending COBRA coverage?
Yes, continuing COBRA coverage usually requires payment of the full premium plus a small administrative fee. Be sure to check with your employer for specific costs involved.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.