Last updated on Apr 10, 2026

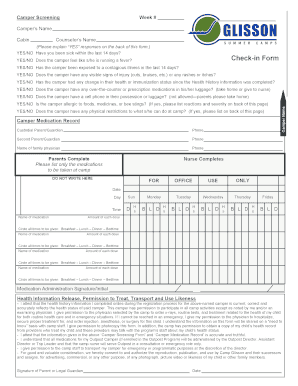
Get the free Member Claim Form for Routine Vision
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is member claim form for
The Member Claim Form for Routine Vision is a healthcare document used by members to submit claims for vision services received outside the OptiCare network.
pdfFiller scores top ratings on review platforms




Who needs member claim form for?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to member claim form for
What is the Member Claim Form for Routine Vision?
The Member Claim Form for Routine Vision serves as a critical tool for OptiCare members who need to submit claims for vision services received outside the network. This form plays an essential role in the claims process, as it allows members to retrieve essential reimbursements. Utilizing the Member Claim Form is vital for effective submissions, ensuring that members can successfully claim benefits for their out-of-network vision services.
Purpose and Benefits of the Member Claim Form for Routine Vision
This specific member vision claim form is necessary for OptiCare members to file claims efficiently. By using this form, members can benefit from reimbursement on vision care that is provided outside of their usual network. Additionally, the form streamlines the claims process, making it easier for members to retrieve their benefits without unnecessary delays.
Who Needs to Use the Member Claim Form for Routine Vision?
The Member Claim Form is specifically designed for members who have received vision services from out-of-network providers. Members eligible to use the form generally include those who see non-network providers for their vision care. Situations necessitating the use of this form often arise when members are unable to access in-network services, making it crucial for these individuals to file claims for reimbursement.
How to Fill Out the Member Claim Form for Routine Vision
Filling out the Member Claim Form requires attention to detail. To complete the form, follow these steps:
-
Begin by entering your personal member details.
-
Provide information about the vision provider, including their contact information.
-
Attach an itemized receipt detailing the services received.
Common mistakes include omitting required fields or not including adequate supporting information. Ensure that both member and provider details are accurate to avoid delays in processing.
Required Documents and Supporting Materials
Submitting the Member Claim Form requires certain supporting documents. Members need to provide:
-
A clear itemized receipt from the vision provider.
-
Details of the service rendered, including dates and types of services.
Each document plays a vital role in ensuring that the claim is processed successfully. Before submission, members should verify that all required documentation is complete to avoid processing delays.
Submission Methods for the Member Claim Form for Routine Vision
Completed Member Claim Forms can be submitted via various methods. Members may choose to:
-
Mail the form to the designated OptiCare address.
-
Utilize electronic submission options, where applicable.
It’s important to note where to send the form accurately, as this will ensure timely processing. Members should also be aware of potential processing times, which may vary depending on the submission method chosen.
Tracking Your Submission and What Happens Next
After submitting your claim, it's essential to know how to track its status. Members can check their claim status through the OptiCare member portal. Common timelines for claim processing may fluctuate, but members can generally expect notifications regarding the status of their submission within a few weeks.
Security and Compliance for the Member Claim Form for Routine Vision
Security is paramount when handling sensitive information contained within the Member Claim Form. The submission process adheres to rigorous security measures to protect personal data. Compliance with regulations such as HIPAA and GDPR ensures that members’ information remains safe and confidential throughout the claims process.
How pdfFiller Simplifies the Claim Process
pdfFiller enhances the Member Claim Form process by offering user-friendly features. Members can easily edit and eSign the form online, facilitating quick and secure submission. With numerous satisfied users, pdfFiller assures an effective way to manage and file vision claims, providing a seamless experience.
Final Steps to Take Before Submission
Before submitting the Member Claim Form, members should take the following final steps:
-
Review all filled fields and ensure accuracy of the information.
-
Double-check that all required documentation is included.
Taking these steps helps ensure that the submission process runs smoothly and efficiently, preventing unnecessary delays or complications.
How to fill out the member claim form for
-
1.Access the Member Claim Form for Routine Vision on pdfFiller by searching for the form title in the platform's search bar.
-
2.Once opened, familiarize yourself with the layout to locate fields designated for member and provider information.
-
3.Before starting, gather all necessary information including your personal details, provider's details, and an itemized receipt of the services received.
-
4.Begin by filling in your personal information in the designated fields such as name, address, and contact number.
-
5.Next, enter the provider's information, including their name, address, and any other requested details in the relevant sections.
-
6.Provide details about the vision services you received, specifying dates and any other requested descriptions.
-
7.Attach your itemized receipt: use the options in pdfFiller to upload a scanned copy of your receipt, ensuring it's clear and legible.
-
8.Carefully review the form for any missing information or errors before signing. Verify all details are accurate.
-
9.Finalize the form by signing in the required section using pdfFiller's signature tool.
-
10.When finished, save your completed form using the save option. Consider downloading it as a PDF for your records.
-
11.Submit the claim by mailing the signed form to OptiCare Managed Vision's address in Rocky Mount, NC. Check the mailing option in pdfFiller if you prefer to send it electronically.

Who is eligible to use the Member Claim Form for Routine Vision?
Members of the OptiCare Managed Vision network who receive routine vision services outside the network are eligible to use this claim form.
What deadlines should I be aware of when submitting my claim?
It's important to submit your claim as soon as possible after receiving services. Check OptiCare's policies for any specific deadlines to ensure prompt processing.
How do I submit the Member Claim Form once completed?
After filling out the form, you should print it and mail it to OptiCare Managed Vision in Rocky Mount, NC. Ensure that it is signed before sending.
What supporting documents do I need to include with my claim?
You will need to attach an itemized receipt of the services received, along with your completed claim form, to support your reimbursement request.
What common mistakes should I avoid when filling out the claim form?
Common mistakes include missing signatures, providing incorrect information, or failing to attach the necessary receipts. Double-check all sections before submission.
How long does it take for claims to be processed by OptiCare?
Processing times can vary, but claims are typically processed within a few weeks. Confirm with OptiCare for specific details on processing timelines.
What should I do if I have a question about my claim status?
If you have inquiries about your claim status, contact OptiCare customer service directly with your claim reference number for assistance.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.