Last updated on Apr 11, 2026

Get the free Prior Authorization of Benefits Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is prior authorization of benefits
The Prior Authorization of Benefits Form is a healthcare document used by physicians to request medication coverage approval for their patients.
pdfFiller scores top ratings on review platforms




Who needs prior authorization of benefits?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to prior authorization of benefits
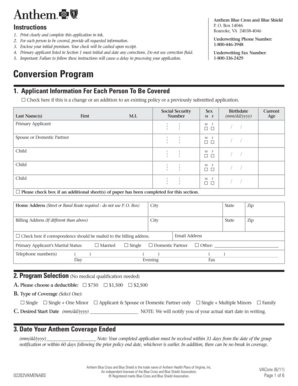
What is the Prior Authorization of Benefits Form?
The Prior Authorization of Benefits Form is a critical document in the healthcare system, primarily used by physicians to obtain approval for medication coverage. This form facilitates communication between healthcare providers, patients, and insurance companies to ensure that necessary treatments are accessible. Key contents of the form include essential fields such as patient information, medication details, and diagnosis specifics. A notable aspect is the physician's involvement; a signature from the healthcare provider is mandatory, emphasizing their professional endorsement of the medication request.
Purpose and Benefits of the Prior Authorization of Benefits Form
The main purpose of this authorization form is to enhance patient access to medications, ensuring timely treatment. By providing a structured way to obtain approvals, physicians can more effectively manage medication costs, benefiting both their practice and the patients. Accurate completion of the form is vital to prevent delays in the medication approval process, as any errors can lead to extended waiting periods for patients needing urgent care.
Key Features of the Prior Authorization of Benefits Form
This form is designed with several fillable fields, including checkboxes to streamline the input of patient and medication details. Some notable features include:
-
Sections dedicated to patient demographics and medical history
-
Specific fields for medication name, dosage, and frequency
-
Assurances of confidentiality, ensuring patient information is protected
-
Legal disclaimers to inform users of their rights and responsibilities
Utilizing a digital platform like pdfFiller enhances usability, allowing for convenient online completion and submission.
Who Needs the Prior Authorization of Benefits Form?
This form is essential for multiple stakeholders, including physicians, patients, and insurance companies. Specific scenarios warrant the use of this form, such as requests for high-cost medications or new treatments not previously covered. Generally, patients facing chronic conditions or those prescribed certain medications are more likely to require prior authorization, making this form a necessity for timely care.
How to Fill Out the Prior Authorization of Benefits Form Online (Step-by-Step)
Completing the Prior Authorization Form online is straightforward when using pdfFiller. Here are the steps to fill it out effectively:
-
Gather all necessary patient information, including medical history and current medications.
-
Access the form via pdfFiller and begin inputting data into the required fields.
-
Ensure accurate documentation of medication specifics, including dosages and diagnosis.
-
Review the filled form for completeness and accuracy before submission.
-
Securely save your completed document within the pdfFiller platform.
Common Errors and How to Avoid Them
Filling out the Prior Authorization of Benefits Form can be prone to errors. Frequent mistakes include:
-
Omitting critical patient information or medication details
-
Incorrect or incomplete diagnosis entries
-
Failing to obtain a physician's signature where required
To enhance the accuracy of submissions, it is advisable to double-check all entries and confirm that the completed form adheres to all necessary guidelines before sending it off.
How to Submit the Prior Authorization of Benefits Form
After completing the form, several submission methods are available, including:
-
Faxing the form directly to the insurance provider
-
Mailing it to the designated address noted on the form
-
Utilizing online submission options provided by the insurance company
Each method has its specifications regarding where to send or deliver the form. Ensuring that you track the submission status is important for confirming its receipt and following up if necessary.
What Happens After You Submit the Prior Authorization of Benefits Form?
Once the form is submitted, the processing timeline can vary. Typically, you can expect an initial review phase, which may take several days. Potential outcomes include approvals or denials, and understanding how to handle delays or rejections is crucial. Follow-up actions may be required to address any issues that arise, ensuring continuous communication with the insurance provider during this phase.
Security and Compliance for the Prior Authorization of Benefits Form
Patient data security is paramount when handling the Prior Authorization of Benefits Form. Compliance with regulations such as HIPAA is essential to maintain confidentiality. pdfFiller employs 256-bit encryption and is both HIPAA and GDPR compliant, assuring users that their information remains protected even during electronic submissions.
Leverage pdfFiller for Your Prior Authorization of Benefits Form
Using pdfFiller for the Prior Authorization of Benefits Form streamlines the process of filling, signing, and managing your documents. The platform offers features that enable users to edit, store, and securely share completed forms in a cloud-based environment, enhancing overall efficiency and convenience.
How to fill out the prior authorization of benefits
-
1.Access the Prior Authorization of Benefits Form on pdfFiller by searching for its title or browsing the healthcare forms section.
-
2.Once the form is open, begin filling in the necessary patient details such as name, date of birth, and insurance information in the designated fields.
-
3.Gather the required medication specifics, including the medication name, dosage, and frequency, before starting the form.
-
4.Make sure to include the diagnosis related to the medication request to provide context for approval criteria.
-
5.Use the checkboxes to confirm any medical necessity criteria that apply to the patient's situation.
-
6.If applicable, enter additional notes that may support the authorization request.
-
7.Review all filled fields for accuracy and completeness to avoid delays in processing.
-
8.Once finished, use the save feature on pdfFiller to create a copy of the completed form.
-
9.You can download the form in your preferred format or share it directly via email.
-
10.Finally, submit the form to the appropriate insurance company according to their specified submission guidelines.

Who is eligible to use the Prior Authorization of Benefits Form?
Physicians are eligible to use this form when requesting medication coverage on behalf of their patients who have insurance plans requiring prior authorization.
What information is needed to complete the form?
You will need detailed patient information, specifics about the requested medication, the patient's diagnosis, and any criteria necessary for approval.
How do I submit the completed form to my insurance company?
After completion, the form can typically be faxed or uploaded through the insurance provider's website. Always check with your specific insurance company for their submission guidelines.
Are there any common mistakes to avoid while filling the form?
Common mistakes include incomplete fields, missing physician signatures, or failing to include necessary supporting documentation, which can delay approval.
What are the processing times for prior authorizations?
Processing times can vary by insurance provider, but it generally takes anywhere from a few days to a couple of weeks. Check with your insurance for specifics.
Is notarization required for the Prior Authorization of Benefits Form?
No, the Prior Authorization of Benefits Form does not require notarization but must be signed by the prescribing physician.
Can patients submit the form directly?
Typically, patients cannot submit the form directly; it must be submitted by the prescribing physician. However, patients can assist by providing necessary information.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.