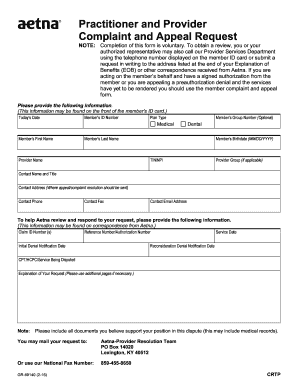
Aetna GR-67656 2007 free printable template
Show details
Once eligible Members have completed the applicable appeal process they may request review of coverage denials that were based upon lack of medical necessity or the experimental or investigational nature of the requested or proposed service or supply by an independent review organization IRO. Members must submit requests for external review within the timeframe specified in the final coverage denial letter. 2. A copy of the coverage denial as well as all other information the Member wishes to...
pdfFiller is not affiliated with any government organization
Get, Create, Make and Sign aetna po box 14020 lexington ky form
Edit your Aetna GR-67656 form online
Type text, complete fillable fields, insert images, highlight or blackout data for discretion, add comments, and more.
Add your legally-binding signature
Draw or type your signature, upload a signature image, or capture it with your digital camera.

Share your form instantly
Email, fax, or share your Aetna GR-67656 form via URL. You can also download, print, or export forms to your preferred cloud storage service.
How to edit Aetna GR-67656 online
To use our professional PDF editor, follow these steps:
1
Set up an account. If you are a new user, click Start Free Trial and establish a profile.
2
Upload a document. Select Add New on your Dashboard and transfer a file into the system in one of the following ways: by uploading it from your device or importing from the cloud, web, or internal mail. Then, click Start editing.
3
Edit Aetna GR-67656. Rearrange and rotate pages, add new and changed texts, add new objects, and use other useful tools. When you're done, click Done. You can use the Documents tab to merge, split, lock, or unlock your files.
4
Save your file. Select it from your list of records. Then, move your cursor to the right toolbar and choose one of the exporting options. You can save it in multiple formats, download it as a PDF, send it by email, or store it in the cloud, among other things.
pdfFiller makes working with documents easier than you could ever imagine. Try it for yourself by creating an account!
Uncompromising security for your PDF editing and eSignature needs
Your private information is safe with pdfFiller. We employ end-to-end encryption, secure cloud storage, and advanced access control to protect your documents and maintain regulatory compliance.
Aetna GR-67656 Form Versions
Version
Form Popularity
Fillable & printabley
How to fill out Aetna GR-67656
How to fill out Aetna external review form:
01
Make sure you have all the necessary information and documentation ready, including your medical records, invoices, and any supporting documents related to your request for review.
02
Carefully read and understand the instructions provided on the form. Familiarize yourself with the required sections, fields, and any specific guidelines provided.
03
Begin by providing your personal information, such as your name, contact details, and Aetna member ID number. Ensure the accuracy of this information to avoid any processing delays.
04
Proceed to fill out the sections requesting details about the medical service or treatment you are seeking external review for. Include relevant information, such as the date of service, name of the healthcare provider, and a brief description of the treatment received.
05
If applicable, provide information regarding any insurance claim related to the medical service or treatment in question. This may include details about the claim number, date submitted, and any correspondence with Aetna or the healthcare provider.
06
Next, explain the reason for your request for an external review. Clearly state the issue you are disputing and provide any supporting evidence or documentation. Be concise yet thorough in this section.
07
If there are any additional documents you are submitting along with the form, clearly label and attach them, ensuring they are relevant to your request for review.
08
Carefully review the filled-out form to ensure all sections are completed accurately and legibly. Double-check for any errors or missing information before submitting the form.
09
Sign and date the form to certify the accuracy of the information provided. Failure to sign the form may result in a processing delay.
10
Submit the completed form and all accompanying documentation to the specified address, either by mail or electronically as instructed. Keep copies of all documents for your records.
Who needs the Aetna external review form?
01
Individuals who have received medical treatment or services covered by their Aetna insurance policy and wish to dispute a decision made by Aetna regarding coverage or reimbursement.
02
Patients or policyholders who believe their healthcare provider is not in agreement with Aetna's decision regarding coverage or reimbursement and wish to escalate the issue for an external review.
03
Any Aetna member seeking a third-party evaluation and review of benefits, medical necessity, or coverage denials by Aetna.
Fill
form
: Try Risk Free






People Also Ask about
Is Aetna good insurance reviews?
Aetna is rated A (excellent) by AM Best, and has high ratings from several other financial ratings services. AM Best is a credit rating firm that assesses the creditworthiness of and/or reports on over 16,000 insurance companies worldwide.
What is an external review in health insurance?
A review of a plan's decision to deny coverage for or payment of a service by an independent third-party not related to the plan. If the plan denies an appeal, an external review can be requested.
How do I appeal a denied claim with Aetna?
You can file a grievance or appeal using our online grievance and appeal form. 1-855-772-9076 (TTY: 711). You can send a secure fax to Aetna® grievances and appeals at 959-888-4487. Your doctor can file a grievance or request an appeal on your behalf after you give them your written permission.
What is an external review request?
What is an external review? External review is a process where you may seek an independent review of a health insurance company decision to refuse to pay for or authorize a treatment or service.
What is external review in healthcare?
What is an external review? External review is a process where you may seek an independent review of a health insurance company decision to refuse to pay for or authorize a treatment or service. External review is limited to health insurance company decisions based on medical necessity.
How long does an external review take?
Standard external reviews are decided as soon as possible – no later than 45 days after the request was received. Expedited external reviews are decided as soon as possible – no later than 72 hours, or less, depending on the medical urgency of the case, after the request was received.
Our user reviews speak for themselves
Read more or give pdfFiller a try to experience the benefits for yourself
For pdfFiller’s FAQs
Below is a list of the most common customer questions. If you can’t find an answer to your question, please don’t hesitate to reach out to us.
Where do I find Aetna GR-67656?
The premium pdfFiller subscription gives you access to over 25M fillable templates that you can download, fill out, print, and sign. The library has state-specific Aetna GR-67656 and other forms. Find the template you need and change it using powerful tools.
Can I create an electronic signature for the Aetna GR-67656 in Chrome?
Yes. You can use pdfFiller to sign documents and use all of the features of the PDF editor in one place if you add this solution to Chrome. In order to use the extension, you can draw or write an electronic signature. You can also upload a picture of your handwritten signature. There is no need to worry about how long it takes to sign your Aetna GR-67656.
Can I edit Aetna GR-67656 on an iOS device?
Use the pdfFiller mobile app to create, edit, and share Aetna GR-67656 from your iOS device. Install it from the Apple Store in seconds. You can benefit from a free trial and choose a subscription that suits your needs.
What is Aetna GR-67656?
Aetna GR-67656 is a specific group health insurance plan offered by Aetna, designed to provide various healthcare benefits to eligible members.
Who is required to file Aetna GR-67656?
Employers or plan sponsors who provide health benefits under the Aetna GR-67656 plan are required to file necessary documentation for compliance and reporting.
How to fill out Aetna GR-67656?
To fill out Aetna GR-67656, one must gather the required information regarding employees or members, accurately complete the forms as per instructions, and submit them as directed by Aetna.
What is the purpose of Aetna GR-67656?
The purpose of Aetna GR-67656 is to ensure compliance with health insurance regulations and to provide a structured way for employers to report employee health benefits.
What information must be reported on Aetna GR-67656?
Information that must be reported on Aetna GR-67656 includes employee identification details, coverage levels, and any relevant enrollment information for the health plan.
Fill out your Aetna GR-67656 online with pdfFiller!
pdfFiller is an end-to-end solution for managing, creating, and editing documents and forms in the cloud. Save time and hassle by preparing your tax forms online.

Aetna GR-67656 is not the form you're looking for?Search for another form here.
Relevant keywords
Related Forms
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.