Last updated on Apr 12, 2026

Get the free Revatio Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is revatio prior authorization form
The Revatio Prior Authorization Form is a healthcare document used by physicians to request insurance coverage for Revatio (sildenafil) for patients with pulmonary arterial hypertension (PAH).
pdfFiller scores top ratings on review platforms




Who needs revatio prior authorization form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to revatio prior authorization form
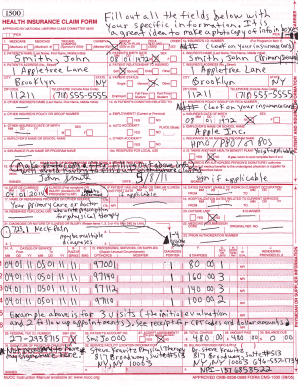
What is the Revatio Prior Authorization Form?
The Revatio Prior Authorization Form is an essential document used in the healthcare system to facilitate medication coverage for patients diagnosed with pulmonary arterial hypertension (PAH). This form plays a critical role in ensuring that patients receive necessary treatments by formally requesting approval from insurance providers.
Key components of the form include specific details such as patient information—name, date of birth, and member ID—as well as physician details. The inclusion of these details is significant as it forms the basis for submitting the request for coverage.
Purpose and Benefits of the Revatio Prior Authorization Form
The primary purpose of the Revatio Prior Authorization Form is to secure medication coverage for patients suffering from PAH. This ensures that those in need of treatment do not face unnecessary delays in receiving their prescribed medications.
Benefits of utilizing this form include expedited insurance approvals, reduced likelihood of medication denials, and the assurance that patients are receiving appropriate care. By clearly defining the medical need, the form helps align treatment plans between healthcare providers and insurers.
Who Needs the Revatio Prior Authorization Form?
This form is primarily used by healthcare providers, including physicians, who are involved in diagnosing and treating patients with Revatio coverage needs. Additionally, patients who have been prescribed Revatio should ensure that their healthcare provider submits this authorization form.
It is important for patients to have a diagnosis from specialists, such as Pulmonologists or Cardiologists, as this demonstrates the medical necessity for medication coverage. Such a diagnosis is crucial for the successful approval of the form.
Eligibility Criteria for the Revatio Prior Authorization Form
To be considered for coverage using the Revatio Prior Authorization Form, patients must meet specific medical criteria. These criteria typically include having a confirmed diagnosis of pulmonary arterial hypertension, which establishes the need for treatment.
Additionally, it is essential to demonstrate that patients have previously excluded calcium channel blocker therapy prior to initiating treatment with Revatio, as this is often a requirement for eligibility.
How to Fill Out the Revatio Prior Authorization Form Online (Step-by-Step)
Filling out the Revatio Prior Authorization Form electronically can streamline the process significantly. Here's a step-by-step guide:
-
Access the form on pdfFiller's platform.
-
Complete the key fields, including the patient's name, date of birth, and member ID.
-
Indicate the diagnosis details and treatment specifics by checking the appropriate boxes.
-
Ensure that the physician includes their signature in the designated area.
-
Review all entered information for accuracy before submission.
Common Errors in Filing the Revatio Prior Authorization Form
When completing the Revatio Prior Authorization Form, users often make several common mistakes. Typical errors include missing signatures, incomplete patient information, and neglecting to provide necessary diagnosis details.
To avoid these pitfalls, it is advisable to double-check all entries for accuracy and completeness before submission. Ensuring that all required fields are filled can help facilitate a smoother processing experience.
Submission Guidelines for the Revatio Prior Authorization Form
Submitting the completed Revatio Prior Authorization Form is crucial to moving forward with medication coverage. The form can be submitted through various methods, such as online through pdfFiller or via fax, depending on your provider's preferences.
After submission, it is important to track the status of the form and follow up if necessary to ensure that the authorization process is completed in a timely manner.
Security and Compliance Considerations for the Revatio Prior Authorization Form
Handling sensitive patient information requires stringent security measures. The Revatio Prior Authorization Form is designed to comply with HIPAA and GDPR regulations, ensuring the privacy and protection of patient data.
Using secure platforms, such as pdfFiller, ensures that all data related to the form remains confidential and is handled in a secure manner, reinforcing the trust needed in healthcare transactions.
Why Use pdfFiller for Your Revatio Prior Authorization Form Needs?
Choosing pdfFiller for filling out the Revatio Prior Authorization Form offers numerous advantages. Users benefit from a user-friendly interface that simplifies editing, filling, and sharing of forms securely.
With features including eSigning and document management, pdfFiller enhances accessibility and efficiency, making the entire process more manageable while also prioritizing security for sensitive documents.
Next Steps After Submitting the Revatio Prior Authorization Form
After submitting the Revatio Prior Authorization Form, users can expect a confirmation from their insurance provider regarding the approval status. Timelines can vary, so it is important to be prepared for potential follow-up actions or additional documentation requests.
Utilizing tools like pdfFiller can aid in ensuring that the form is correctly completed and submitted, contributing to a higher likelihood of successful authorization.
How to fill out the revatio prior authorization form
-
1.Access pdfFiller's website and log in or create an account if you do not have one.
-
2.Search for the 'Revatio Prior Authorization Form' using the search bar on the dashboard.
-
3.Click on the form to open it in the pdfFiller editor interface.
-
4.Begin by filling in the fields labeled 'Patient Name', 'DOB', and 'Member ID#' accurately.
-
5.Check the appropriate boxes to indicate the diagnosis and treatment options pertinent to the patient's condition.
-
6.Gather all necessary documentation, including diagnosis details from the Pulmonologist or Cardiologist to complete the form accurately.
-
7.Review each filled field to ensure accuracy and completeness, as mistakes could delay processing.
-
8.Once satisfied with the information, proceed to the finalize section in pdfFiller.
-
9.Click on the 'Save' option to store your completed form.
-
10.Download the form to your device as a PDF or use the 'Submit' function if it's electronically submitted directly through pdfFiller.

Who is eligible to use the Revatio Prior Authorization Form?
The Revatio Prior Authorization Form is generally for patients diagnosed with pulmonary arterial hypertension (PAH) who need Revatio. Physicians like Pulmonologists or Cardiologists must use it to request coverage from insurance companies.
What supporting documents are required when submitting the form?
Along with the Revatio Prior Authorization Form, you may need to provide supporting documentation, such as diagnosis details, treatment history, and clinical response information. This ensures that the insurance company has all necessary information to approve the request.
How should I submit the completed Revatio Prior Authorization Form?
You can submit the completed Revatio Prior Authorization Form by downloading it and mailing it to the relevant insurance provider, or if available, you may submit it electronically through pdfFiller, ensuring that you follow the submission guidelines provided by the insurance company.
What common mistakes should I avoid when filling out this form?
Common mistakes include incomplete fields, incorrect patient information, and failing to provide required diagnosis documentation. Ensure that all necessary sections are filled out accurately and completely to streamline the authorization process.
How long does it take to process the Revatio Prior Authorization Form?
Processing times for authorization requests can vary by insurance provider but typically range from a few days to two weeks. It’s advisable to follow up with the insurance company if you do not hear back within the expected time frame.
Are there any fees associated with submitting the Revatio Prior Authorization Form?
Generally, there are no direct fees for submitting a prior authorization form itself. However, be aware that health insurance policies may have specific costs associated with the medication that will be determined after the form’s approval.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.