Last updated on Apr 12, 2026

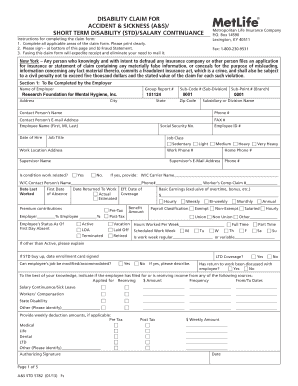
Get the free Provider Appeal/Reconsideration Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is provider appealreconsideration form
The Provider Appeal/Reconsideration Form is a healthcare document used by providers to request a review or reconsideration of denied claims.
pdfFiller scores top ratings on review platforms




Who needs provider appealreconsideration form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to provider appealreconsideration form
Understanding the Provider Appeal/Reconsideration Form
The Provider Appeal/Reconsideration Form is an essential document within the healthcare claims process. This form serves as a formal request for healthcare providers to challenge contested or denied claims. By filing this form, providers can initiate a review of decisions that may affect their reimbursement.
Understanding the significance of the Provider Appeal/Reconsideration Form is crucial for providers aiming to safeguard their financial interests in the complex healthcare environment.
Purpose and Benefits of the Provider Appeal/Reconsideration Form
This form enables healthcare providers to effectively resolve disputes regarding denied claims. Filing the Provider Appeal/Reconsideration Form ensures that providers can advocate for timely payments and clear up any issues that may arise during the claims process.
Among the key benefits are enhanced communication with insurance companies and improved chances of receiving rightful payments, which is vital for maintaining financial stability in healthcare practices.
Who Needs the Provider Appeal/Reconsideration Form
Various healthcare providers, including hospitals, clinics, and individual practitioners, may find themselves in situations warranting the use of this form. Typical scenarios include instances of insurance claim denials or discrepancies in service coverage.
By understanding who needs the Provider Appeal/Reconsideration Form, providers can ensure they are well-prepared to address any disputes that may impact their practice.
Eligibility Criteria and Important Timelines
Eligibility for utilizing the Provider Appeal/Reconsideration Form hinges on specific insurance plan guidelines and the nature of the claim in question. Providers must adhere to strict timelines, which often include submission deadlines as well as response periods from the insurance carrier.
Failing to meet these critical deadlines could result in the loss of the right to appeal, thus jeopardizing the claim’s review process and impacting revenue.
How to Fill Out the Provider Appeal/Reconsideration Form Online
Filling out the Provider Appeal/Reconsideration Form online requires attention to detail. Begin by providing essential fields such as the Member Name, Date of Service, and Provider Name. Additionally, include supporting documentation that substantiates the appeal.
To ensure accuracy, it's recommended to use a checklist to review the completed form before submission. This preparatory step can significantly reduce the likelihood of errors that might delay processing.
Submission Methods and Confirmation Tracking
Providers can submit the completed Provider Appeal/Reconsideration Form through various methods, including mail and online portals. It is crucial to confirm receipt of the appeal to track its status efficiently.
After submitting the form, providers can expect notifications regarding the processing of their appeal, which is important in keeping all parties informed throughout the claims process.
Common Errors When Filing the Provider Appeal/Reconsideration Form
To improve the success rates of appeals, providers must be aware of common pitfalls encountered during filing. Key mistakes include incomplete information, missing required documentation, and failing to adhere to deadlines.
Implementing best practices and thorough reviews can help mitigate these issues, ultimately leading to a smoother appeals process and enhanced chances of favorable resolutions.
Security and Compliance for Healthcare Providers
Ensuring the security of the Provider Appeal/Reconsideration Form is paramount, particularly given the sensitive nature of the information involved. Healthcare providers are obligated to adhere to compliance requirements, including HIPAA regulations, to protect patient data during the submission process.
Utilizing secure platforms, such as pdfFiller, enhances document security through measures like encryption, ensuring that sensitive information remains protected throughout its lifecycle.
How pdfFiller Can Help with the Provider Appeal/Reconsideration Form
pdfFiller offers a range of features to assist healthcare providers in completing and submitting the Provider Appeal/Reconsideration Form with ease. The platform provides tools for editing, filling, and securely submitting documents, streamlining the often complicated appeal process.
Choosing a reliable document management solution like pdfFiller dramatically improves efficiency, providing providers with the tools needed to manage their claims effectively.
Wrap Up Your Appeal Successfully with pdfFiller
Efficiently completing the Provider Appeal/Reconsideration Form is crucial for healthcare providers seeking resolution for disputed claims. pdfFiller's user-friendly tools not only simplify the filing process but also ensure compliance with security standards.
Healthcare providers are encouraged to leverage pdfFiller to maximize their chances of successful appeals and secure their rightful reimbursements.
How to fill out the provider appealreconsideration form
-
1.To access and open the Provider Appeal/Reconsideration Form on pdfFiller, go to the pdfFiller website and use the search bar to locate the form by typing in its name.
-
2.Once you find the form, click on it to open the fillable version. Familiarize yourself with the layout, including the various sections and fields you need to complete.
-
3.Before starting the form, gather all necessary information, including member and provider details, the reason for the appeal, and any supporting documents that may be needed for submission.
-
4.Begin filling in the required fields, such as 'Member Name', 'Date of Service', and 'Provider Name'. Use pdfFiller's tools to ensure all fields are properly filled with clear and concise information.
-
5.As you complete each section, review your entries for accuracy. Correct any errors and ensure that all required checkboxes and fields are marked appropriately.
-
6.Once the form is filled out, proceed to review it thoroughly. Check that all fields are complete and that you have attached any necessary supporting documentation to bolster your appeal.
-
7.After finalizing the form, you can save it directly to your computer, download a copy for your records, or submit it through pdfFiller based on the given instructions from your insurance company.

Who is eligible to use the Provider Appeal/Reconsideration Form?
The form is intended for healthcare providers who have submitted claims that have been denied or disputed. Providers must have the relevant patient and claim information to complete the appeal.
What is the deadline for submitting this form?
Timelines for submission of the Provider Appeal/Reconsideration Form vary by insurance provider. It’s important to check the specific guidelines for each case, but generally, submissions could be required within a standard response window post-denial.
How do I submit the Provider Appeal/Reconsideration Form?
After completing the form, you must mail it to the specified address provided by the insurance company. Ensure you follow the submission guidelines for a review to occur.
What supporting documents are required with the form?
You should include any relevant documentation such as the denial notice, patient medical records, and any additional information that supports the appeal. Be thorough to strengthen your case.
What are common mistakes when filling out this form?
Common errors include incomplete fields, missing signatures, and not including required supporting documents. Ensure all information is accurate and all requested documentation is attached.
What is the typical processing time for appeals?
The processing time for appeals can vary significantly based on the provider and the complexity of the case. Typically, you can expect a response anywhere from a few weeks to several months.
Can the form be filled out electronically?
Yes, you can complete the Provider Appeal/Reconsideration Form electronically using platforms like pdfFiller, which provides fillable fields and easy navigation for completion.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.