Last updated on Sep 16, 2014
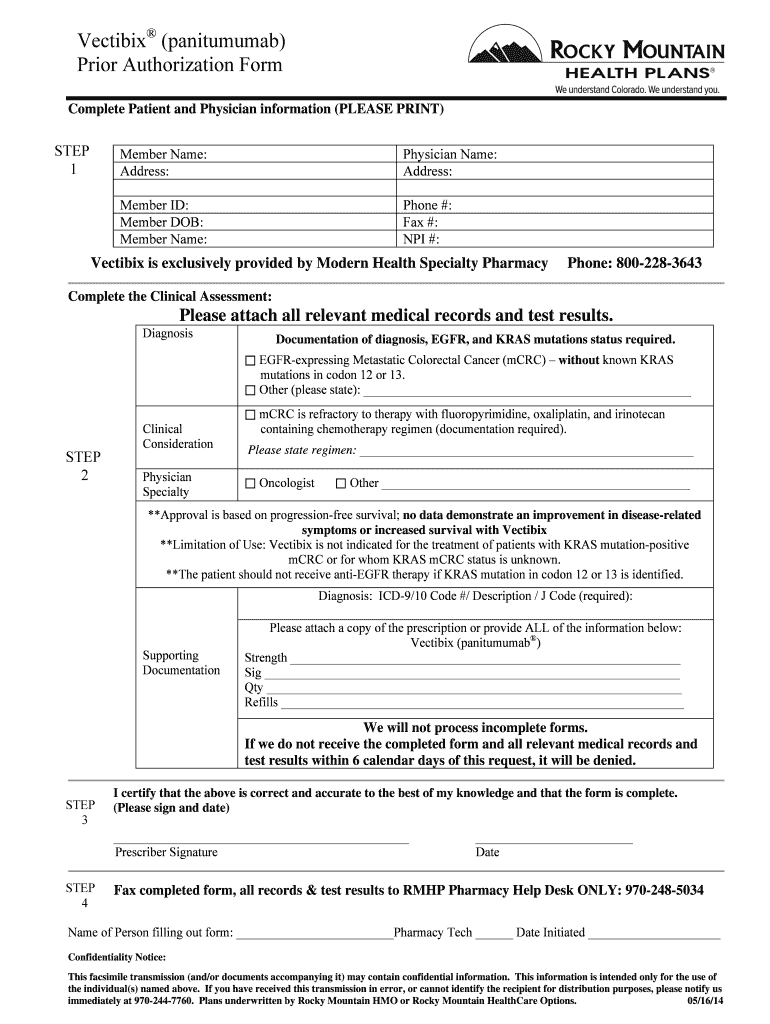
Get the free Vectibix Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is vectibix prior authorization form
The Vectibix Prior Authorization Form is a medical consent document used by healthcare providers to request approval for Vectibix (panitumumab) treatment for EGFR-expressing metastatic colorectal carcinoma.
pdfFiller scores top ratings on review platforms




Who needs vectibix prior authorization form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to vectibix prior authorization form
What is the Vectibix Prior Authorization Form?
The Vectibix Prior Authorization Form is a crucial document utilized by healthcare providers to request prior authorization for Vectibix (panitumumab), specifically for patients diagnosed with EGFR-expressing metastatic colorectal carcinoma. This form ensures that patients have access to necessary treatments by facilitating communication between physicians and insurance providers. It was last updated in May 2014, making it essential for users to refer to the most current guidelines.
This authorization process forms the backbone of treatment access, as it directly impacts coverage decisions made by insurance companies concerning this important medication.
Purpose and Benefits of the Vectibix Prior Authorization Form
The Vectibix Prior Authorization Form serves multiple purposes for both patients and healthcare providers. Primarily, it is needed to gain insurance approval, ensuring that treatment with Vectibix is covered, which is vital for patient care and cost management.
By acquiring prior authorization, patients can prevent unexpected medical costs, and providers streamline the process, saving time for both physicians and pharmacy techs involved in patient care. Additionally, it minimizes the risk of delays in treatment, thereby enhancing the overall patient experience.
Who Needs the Vectibix Prior Authorization Form?
The Vectibix Prior Authorization Form is designed for healthcare providers, specifically physicians and pharmacy technicians. Physicians are required to sign the form, confirming its accuracy and necessity for the patient's treatment plan, while pharmacy techs assist in processing but do not need to provide a signature.
This form is essential for patients receiving treatment for EGFR-expressing metastatic colorectal cancer, as it directly affects their access to prescribed therapies.
Field-by-Field Instructions for Completing the Vectibix Prior Authorization Form
Completing the Vectibix Prior Authorization Form accurately is critical to avoid delays. Key fields include:
-
Patient Information: Ensure all personal details are correct.
-
Diagnosis: Clearly state the patient's condition, which impacts treatment decisions.
-
Signature Fields: The physician's signature is mandatory.
Tips to provide complete information include double-checking entries and reviewing prior submissions for common mistakes, which can lead to unnecessary rejections or delays in authorization.
How to Fill Out the Vectibix Prior Authorization Form Online
To fill out the Vectibix Prior Authorization Form online using pdfFiller, follow these simple steps:
-
Access the form through pdfFiller's platform.
-
Complete the required fields, ensuring accuracy.
-
eSign the document if necessary, or obtain a signature from the physician.
-
Save and securely store the completed form.
This cloud-based platform offers users ease of access and enhances data security, reassuring patients and providers that sensitive information is protected throughout the process.
Submission Methods and Delivery of the Vectibix Prior Authorization Form
The completed Vectibix Prior Authorization Form can be submitted in several ways:
-
Electronically: Use secure email or online submission portals.
-
Traditional Mail: Send the form directly to the insurance company.
It is crucial to adhere to submission deadlines to avoid disruptions in patient care and treatment plans. Users should also keep track of their submission status to ensure timely responses from insurance providers.
Consequences of Not Filing or Late Filing the Vectibix Prior Authorization Form
Failing to submit the Vectibix Prior Authorization Form or submitting it late can have serious repercussions for patients. Without timely filing, there may be delays in the start of treatment or complications in insurance coverage, potentially affecting overall treatment outcomes.
Maintaining compliance with insurance requirements is essential to avoid these risks and to ensure that patients receive the medications they need without interruption.
Security and Compliance for the Vectibix Prior Authorization Form
Utilizing pdfFiller for the Vectibix Prior Authorization Form guarantees that sensitive documents are handled securely. The platform complies with HIPAA and GDPR regulations, providing users with the confidence that their data is protected.
pdfFiller employs 256-bit encryption and maintains SOC 2 Type II compliance to ensure that user data is kept confidential, fostering trust among healthcare providers and patients alike.
How to Check Your Application Status After Submission
After submitting the Vectibix Prior Authorization Form, it is important to follow up to ensure approval. Users should keep track of crucial information, such as:
-
Submission date and method.
-
Any unique reference or tracking numbers provided by the insurance company.
This information will aid in inquiries regarding the application's status and understanding any common rejection reasons that may arise during the approval process.
Enhance Your Experience with pdfFiller
pdfFiller enhances the experience of filling out the Vectibix Prior Authorization Form by offering a variety of capabilities, such as eSigning, editing, and secure storage of documents. Users benefit from a streamlined process that simplifies form completion and increases efficiency.
Success stories and testimonials highlight the platform's effectiveness, assuring users of a reliable and user-friendly experience in managing their healthcare documentation.
How to fill out the vectibix prior authorization form
-
1.To access the Vectibix Prior Authorization Form on pdfFiller, visit the website and search for the form by name or upload the PDF directly onto your dashboard.
-
2.Once the form is open, familiarize yourself with the fillable fields, including patient and physician information sections.
-
3.Before completing the form, gather necessary information such as the patient's diagnosis, EGFR, and KRAS mutation statuses, as well as the details of any prior therapies.
-
4.Start by entering the patient's information in the designated fields, ensuring accuracy and completeness.
-
5.Next, include the physician's details and add a signature in the prescribed area using the electronic signature tool in pdfFiller.
-
6.Use the checkboxes to indicate the specific therapy and any relevant prior authorizations needed.
-
7.After filling out all required fields, revisit the form to review the information for any potential errors or missing data.
-
8.Once you're confident that the information is accurate, finalize the form by following the prompts to save your progress.
-
9.Finally, choose to download the completed form, submit it directly through pdfFiller, or share it with the appropriate stakeholders via email or printing options.

What are the eligibility requirements for using the Vectibix Prior Authorization Form?
To use the Vectibix Prior Authorization Form, you must be a healthcare provider authorized to prescribe medication for patients diagnosed with EGFR-expressing metastatic colorectal carcinoma.
Is there a deadline for submitting the Vectibix Prior Authorization Form?
While specific deadlines may vary, it's important to submit the Vectibix Prior Authorization Form as soon as possible to avoid delays in treatment. Contact the patient's insurance provider for any specific timelines.
How can I submit the Vectibix Prior Authorization Form once completed?
You can submit the completed Vectibix Prior Authorization Form through pdfFiller by selecting the submission method indicated on the form, which usually includes direct submission to the insurance company or printing to fax.
What supporting documents are required when submitting the Vectibix Prior Authorization Form?
You may need to provide supporting documents such as the patient's medical history, diagnosis details, and previous treatment information alongside the Vectibix Prior Authorization Form.
What are common mistakes to avoid when filling out the form?
Common mistakes include incomplete fields, incorrect patient or physician information, and failure to sign the document. Double-check all entries to ensure accuracy before submission.
How long does it take to process the Vectibix Prior Authorization Form?
Processing times can vary based on the insurance provider's policies, but typically it can take anywhere from a few days to several weeks. Stay in contact with your insurance provider for updates.
Are there any fees associated with the Vectibix Prior Authorization Form submission?
Generally, there are no fees directly associated with submitting the Vectibix Prior Authorization Form. However, charges may apply depending on the specific services or therapies covered by the patient's insurance.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.






















