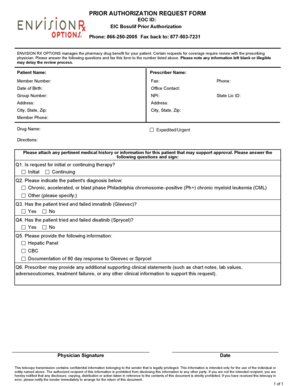Last updated on Oct 6, 2014

Get the free Korlym Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is korlym prior authorization request
The Korlym Prior Authorization Request Form is a healthcare document used by physicians to request prior authorization for the drug Korlym.
pdfFiller scores top ratings on review platforms




Who needs korlym prior authorization request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to korlym prior authorization request
What is the Korlym Prior Authorization Request Form?
The Korlym Prior Authorization Request Form is crucial for healthcare providers seeking prior authorization for the medication Korlym. This form is necessary to ensure that patients receive the appropriate treatment covered by their insurance. The prior authorization process verifies that the prescribed therapy aligns with the patient's medical plan, ensuring both compliance and appropriate care.
The Korlym medication is used in the treatment of specific conditions and requires careful documentation. Submission of this prior authorization request form moves patients one step closer to receiving the treatments they need, while also helping healthcare providers streamline the approval process.
Purpose and Benefits of the Korlym Prior Authorization Request Form
The primary purpose of the Korlym Prior Authorization Request Form is to facilitate access to the medication for patients. For healthcare providers, this treatment authorization form represents a critical element in securing medication coverage for their patients. The process ensures that treatment options align with insurance guidelines and patient needs.
By obtaining prior authorization, both parties benefit from enhanced clarity and communication regarding treatment paths. This authorization process not only improves patient outcomes but also provides healthcare providers with reassurance that the necessary treatments are covered and accessible.
Key Features of the Korlym Prior Authorization Request Form
The Korlym Prior Authorization Request Form includes essential features that need to be understood for effective use. It contains various fillable fields requiring specific patient information, medical history, and treatment details. Key elements include checkboxes for selecting treatment plans and spaces reserved for documenting required signatures from physicians.
A physician’s signature form is mandatory for validation, particularly where detailed medical documentation is essential. Ensuring all required information is correctly filled out increases the chances of a smooth authorization process.
Who Needs the Korlym Prior Authorization Request Form?
This prior authorization request form targets various stakeholders in the healthcare ecosystem. Physicians and healthcare providers must complete the form to initiate the authorization process for their patients. Additionally, patients may need to understand the importance of this medical authorization form in the context of their treatment.
The need for the form arises in specific scenarios, such as when a certain medication is not on the insurance formulary or when prior authorization is mandated for a prescribed therapy. Familiarity with the pharmacy drug benefit form is essential for all parties involved.
How to Fill Out the Korlym Prior Authorization Request Form Online (Step-by-Step)
Completing the Korlym Prior Authorization Request Form online is straightforward when following these steps:
-
Access the form on a secure platform.
-
Fill out all required fields including patient and provider information.
-
Select the appropriate checkboxes related to treatment history and proposed therapy.
-
Include any necessary medical documentation to support the request.
-
Obtain the required physician signature before submission.
To avoid common pitfalls, ensure all fields are accurately filled out. Double-check for any missing information that could delay the approval process.
Submission Methods and Delivery for the Korlym Prior Authorization Request Form
Submitting the completed Korlym Prior Authorization Request Form can be done through various methods. Options typically include faxing the form or submitting it through an electronic portal. Depending on the method chosen, there may be specific deadlines to observe for processing.
For faster processing, electronic submissions are often preferred. Be sure to follow precise instructions on where to submit the Korlym Prior Authorization Request Form to ensure it reaches the review team promptly.
What Happens After You Submit the Korlym Prior Authorization Request Form?
Once the Korlym Prior Authorization Request Form is submitted, applicants can expect a processing timeframe to receive approval or denial notifications. It is important to be aware of the anticipated timeline, which can vary based on the insurance provider's policies.
To check your application status, healthcare providers or patients should refer to the communication channels established by the insurance company. Knowing how to track the submission is crucial for timely follow-ups and avoiding unnecessary delays.
Common Rejection Reasons and How to Avoid Them
Users should be prepared for the possibility of rejection when submitting the Korlym Prior Authorization Request Form. Common reasons for denial may include insufficient medical documentation, incomplete forms, or the drug not being included in the insurer's formulary.
To enhance the chances of approval, ensure that all required fields are meticulously completed and that necessary supporting documents are included. Consulting with a physician early in the process can help identify any potential gaps in the submission.
Security and Compliance for the Korlym Prior Authorization Request Form
When handling the Korlym Prior Authorization Request Form, it is vital to prioritize data security and compliance. pdfFiller employs secure document handling procedures that meet rigorous standards, including HIPAA and GDPR regulations. This ensures that sensitive patient information remains protected throughout the process.
Understanding the importance of privacy and data protection can help mitigate concerns during the completion and submission of authorization requests. Providers can have confidence in using secure platforms for sensitive documentation.
Empower Your Practice with pdfFiller
Utilizing pdfFiller for filling out the Korlym Prior Authorization Request Form offers numerous benefits. The platform’s features include seamless eSigning, secure document storage, and easy access from any browser, all of which streamline the form-filling process.
Healthcare providers can benefit from the platform's user-friendly interface and dedicated customer support, making it a reliable choice for handling online form-filling solutions efficiently.
How to fill out the korlym prior authorization request
-
1.Access the Korlym Prior Authorization Request Form on pdfFiller by searching for it or uploading it directly.
-
2.Once the form is open, navigate through the interactive fields using the menu tools provided.
-
3.Before filling out the form, gather necessary patient information, prescriber details, and specific medical records related to the patient's diagnosis and treatment.
-
4.Start filling in the required fields, including patient demographics and prescriber information. Use the fillable fields carefully, ensuring all details are accurate.
-
5.For any checkboxes or multiple-choice questions, click the appropriate option to select it, ensuring that responses are clear.
-
6.After completing the form, review each section for accuracy. Make sure the document is signed by the prescribing physician as required.
-
7.Once reviewed, save your progress on pdfFiller using the 'Save' feature. You can also download a copy of the completed form to your device.
-
8.Finally, submit the form according to the instructions provided, which may include faxing it to the specified number for prior authorization review.

What are the eligibility requirements for the Korlym prior authorization?
Eligibility typically requires a patient's physician to fill out the Korlym Prior Authorization Request Form with valid medical justification for the drug use. Ensure that all sections are completed accurately to avoid delays.
Is there a deadline for submitting this authorization request?
While specific deadlines may vary, it is advisable to submit the Korlym Prior Authorization Request Form as soon as possible. This helps ensure timely medication access for your patient.
How do I submit the completed form?
The completed form needs to be faxed to the specified number provided on the form. Ensure that you keep a copy for your records before sending.
What supporting documents are required with the form?
Common supporting documents may include patient medical history, clinical notes, or detailed treatment plans. Check with the payer for any specific requirements.
What are some common mistakes when filling out the form?
Common mistakes include incomplete fields, missing physician signatures, or incorrect patient information. Always double-check the form before submission to avoid rejections.
How long does it take to process the authorization request?
Processing times can vary, but usual turnaround for prior authorizations ranges from a few days to a week. Follow up with the payer if you do not receive a decision promptly.
Are there any fees associated with submitting this request?
Typically, there are no fees directly associated with submitting a prior authorization request. However, verify any potential charges with your billing department or the insurance provider.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.