Last updated on Mar 23, 2026

Get the free Cigna Out of Network Therapy Provider Fax Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is cigna out of network
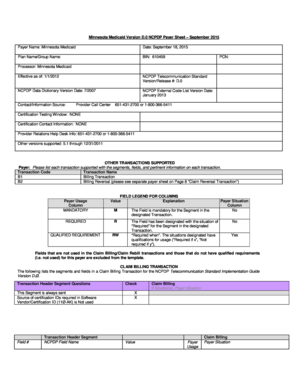
The Cigna Out of Network Therapy Provider Fax Request Form is a medical records release document used by therapy providers to request prior authorization for out-of-network therapy services for Cigna members.
pdfFiller scores top ratings on review platforms




Who needs cigna out of network?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to cigna out of network
What is the Cigna Out of Network Therapy Provider Fax Request Form?
The Cigna Out of Network Therapy Provider Fax Request Form is a specialized document used by therapy providers to request prior authorization for out-of-network services for Cigna members. This form is essential for ensuring that therapy providers receive necessary authorization before delivering services, facilitating smoother patient care and coverage.
Accurate completion and timely submission of the form to OrthoNet are critical for avoiding delays in care and ensuring compliance with Cigna's authorization guidelines. Healthcare providers must familiarize themselves with the requirements of this therapy provider authorization form to streamline their operations.
Purpose and Benefits of the Cigna Out of Network Therapy Provider Fax Request Form
This form serves several important purposes for healthcare providers. First, prior authorization helps streamline the care process by ensuring that services rendered are eligible for coverage. With a standardized form, providers can efficiently manage their authorization requests, reducing administrative burdens.
The process for submitting requests and receiving approvals is designed to be straightforward. Utilizing the Cigna prior authorization form allows providers to maintain a consistent approach when dealing with out-of-network therapy requests, making it easier to track submissions and outcomes.
Eligibility Criteria for the Cigna Out of Network Therapy Provider Fax Request Form
Not all providers can use the Cigna Out of Network Therapy Provider Fax Request Form; specific eligibility criteria apply. Only licensed therapy providers who are seeking authorization for services that fall outside of Cigna’s network can complete this form. Additionally, therapy services requiring prior authorization must align with Cigna's established guidelines.
Cigna members must also meet particular requirements to use out-of-network services, which further defines the circumstances under which this therapy provider authorization form is applicable.
How to Fill Out the Cigna Out of Network Therapy Provider Fax Request Form Online
Completing the Cigna Out of Network Therapy Provider Fax Request Form online involves a series of structured steps. First, gather essential patient information, including the patient’s name, facility name, and therapy details. Each field must be filled with precision, for instance, using black ink and ensuring one character per box.
Here’s a brief overview of the critical fields needed:
-
Patient Name
-
Facility Name
-
Details of Therapy
Following these instructions is vital for correct form submission. Providers should also consider checking the completed form for accuracy before sending it off.
Common Errors and How to Avoid Them
While filling out the Cigna Out of Network Therapy Provider Fax Request Form, providers often encounter common pitfalls. Frequent errors include omitted fields, incorrect patient details, and failure to sign the form. These mistakes can lead to significant delays in authorization.
To avoid these issues, providers should double-check all information before submission. Ensuring completeness can prevent the need for resubmission and help maintain consistent care for Cigna members.
Submission Methods for the Cigna Out of Network Therapy Provider Fax Request Form
The completed Cigna Out of Network Therapy Provider Fax Request Form should be submitted via fax to OrthoNet. Providers must follow specific faxing instructions to ensure successful transmission, where applicable. Additionally, keeping track of the submission confirmation is essential.
Providers may explore alternative submission methods if offered, but fax remains the primary method for this form. Always confirm the fax number and any required documents to accompany the submission.
Tracking Your Submission and What Happens After You Submit
After submitting the Cigna Out of Network Therapy Provider Fax Request Form, providers can track the status of their submissions. Confirmation of receipt and acceptance is vital to ensure that the request has been processed correctly.
Typically, processing times vary based on the request volume; therefore, it is advisable to follow up if no confirmation is received within the expected timeframe. Checking the status of authorization requests can help providers stay informed and prepared for patient care.
Security and Compliance Considerations for Handling the Cigna Out of Network Therapy Provider Fax Request Form
When handling the Cigna Out of Network Therapy Provider Fax Request Form, security and compliance are paramount. pdfFiller employs robust security measures, including data encryption and adherence to HIPAA and GDPR compliance standards, to protect sensitive patient information.
Providers should always prioritize the confidentiality of patient data when submitting forms. Utilizing secure document handling practices helps mitigate risks associated with unauthorized access to sensitive information.
How pdfFiller Can Help with the Cigna Out of Network Therapy Provider Fax Request Form
pdfFiller offers a comprehensive solution for managing the Cigna Out of Network Therapy Provider Fax Request Form. With features such as online editing, e-signature capabilities, and easy form filling, pdfFiller simplifies the entire process for healthcare providers.
The platform enhances operational efficiency by allowing secure sharing and saving of forms online, ensuring that providers can focus more on patient care rather than administrative tasks.
Examples and Templates for the Cigna Out of Network Therapy Provider Fax Request Form
Providing visual aids can significantly help in understanding how to fill out the Cigna Out of Network Therapy Provider Fax Request Form. Examples of completed forms are available to assist providers in brainstorming the necessary fields and formats.
It is also beneficial to note that variations of the form may exist, catering to different types of therapy requests. Downloadable templates and resources within pdfFiller can aid providers in ensuring their submissions are accurate and up to date.
How to fill out the cigna out of network
-
1.Access pdfFiller and search for 'Cigna Out of Network Therapy Provider Fax Request Form'.
-
2.Open the form in pdfFiller by selecting it from the search results.
-
3.Before starting, gather necessary information including the facility and patient details, and therapy service specifications.
-
4.Begin by entering the 'Fax Date' in the respective field at the top of the form.
-
5.Fill in the 'Facility Name', followed by 'First Name' and 'Last Name' of the patient.
-
6.Provide the patient's 'Date of Birth' and ensure all dates are clearly legible.
-
7.Use pdfFiller's tools to check off any relevant therapy requests in the checkboxes provided.
-
8.Review the filled form to ensure all information follows the instruction of one character per box and is printed in black ink.
-
9.Once all sections are completed, verify that all necessary fields are filled as required.
-
10.Save your progress using pdfFiller's save function or export the completed form to your device as a PDF.
-
11.Lastly, fax the completed form along with any required supporting documents to OrthoNet.

Who needs to submit the Cigna Out of Network Therapy Provider Fax Request Form?
The form is required by therapy providers who are requesting prior authorization for out-of-network therapy services on behalf of Cigna members.
What information do I need to fill out the form?
You will need facility details, patient information, and specifics about the requested therapy services to complete the form accurately.
How should the form be submitted?
The completed Cigna Out of Network Therapy Provider Fax Request Form should be faxed along with any supporting documentation to OrthoNet as per instructions.
What should I do if I make a mistake on the form?
If you make a mistake, it's best to clear the field and re-enter the correct information to ensure clarity and avoid any processing delays.
Are there any deadlines for submitting the request?
While specific deadlines may vary, it's advised to submit the request as soon as possible to adhere to therapy service timelines and insurance processing requirements.
What supporting documents are required with the form?
You may need to attach clinical documentation that supports the request for prior authorization, depending on the therapy services requested.
How can I check the status of my request?
To check the status of your authorization request, contact Cigna or OrthoNet directly, and provide them with the details of your faxed submission.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.