Last updated on Oct 22, 2014

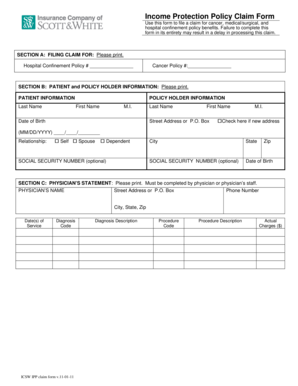
Get the free Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is prior authorization request form
The Prior Authorization Request Form is a medical consent document used by healthcare providers to request insurance coverage for specific drugs related to psoriasis treatment.
pdfFiller scores top ratings on review platforms




Who needs prior authorization request form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to prior authorization request form
What is the Prior Authorization Request Form?
The Prior Authorization Request Form is a crucial tool in the healthcare system, particularly for obtaining prescription drug coverage. This form plays a pivotal role in facilitating access to necessary treatments, including those for psoriasis. By providing essential details, healthcare providers can effectively communicate with insurance companies to secure coverage for medications needed for patients suffering from this condition.
Purpose and Benefits of the Prior Authorization Request Form
This form is essential for healthcare providers to ensure that prescribed medications are covered by insurance plans. It streamlines the authorization process, which is vital for both prescribers and patients. Key benefits include:
-
Improved treatment accessibility through enhanced communication with insurance providers.
-
Increased likelihood of coverage for prescribed medications.
-
Reduction in administrative burden for healthcare providers.
Overall, the form enhances the efficiency of the prescription approval process, which is pivotal for patient care.
Key Features and Sections of the Prior Authorization Request Form
The structure of the Prior Authorization Request Form includes several essential components that facilitate proper completion. Key features consist of:
-
Fillable fields designed to capture patient and prescriber details.
-
Checkboxes for indicating specific drug requests and medical conditions.
-
Sections that require thorough medical history information to support the authorization request.
These design elements are vital in ensuring that all necessary information is collected for a successful submission.
Who Needs to Use the Prior Authorization Request Form?
The primary audience for the Prior Authorization Request Form includes healthcare providers who prescribe medications. Prescribers, such as doctors and nurse practitioners, must utilize this form in specific situations, particularly when a patient’s treatment requires prior approval from an insurance provider for medications related to conditions like psoriasis. It is crucial in scenarios where immediate treatment initiation depends on insurance authorization.
How to Fill Out the Prior Authorization Request Form (Step-by-Step)
Filling out the Prior Authorization Request Form requires attention to detail. Follow these steps to ensure a complete submission:
-
Gather necessary documentation, such as patient identification and medical history records.
-
Complete patient details, including name, date of birth, and insurance information.
-
Fill in prescriber information, ensuring accurate contact details are included.
-
Provide detailed information about the drug being prescribed, including dosage and treatment plan.
-
Review all sections thoroughly to avoid errors before submission.
Having this checklist can help streamline the completion of the form.
Common Errors and How to Avoid Them
When completing the Prior Authorization Request Form, certain pitfalls can impede the submission process. Common errors include:
-
Inaccurate patient or prescriber information, leading to delays.
-
Missing documentation that is required for review.
-
Not reviewing the form for completeness before sending.
To avoid these issues, it is essential to double-check all entries and ensure all requested materials accompany the submission.
Where and How to Submit the Prior Authorization Request Form
Submission of the Prior Authorization Request Form can be done through various channels, accommodating different preferences. Common submission methods include:
-
Faxing the completed form to the designated insurance provider.
-
Using online portals specific to the insurance company.
Ensure that any additional documentation, such as medical records, is included with the submission to facilitate the approval process.
What Happens After You Submit the Prior Authorization Request Form?
Once the Prior Authorization Request Form is submitted, it undergoes a review process by the insurance provider. Here’s what to expect after submission:
-
The request is reviewed for completeness and accuracy by the insurer.
-
Prescribers and patients will be notified regarding the approval or denial of coverage.
-
If denied, common reasons include lack of medical necessity or missing documentation.
Understanding these steps helps set expectations for the timeline of the authorization process.
How pdfFiller Can Simplify the Prior Authorization Request Form Process
pdfFiller offers an effective solution for managing the Prior Authorization Request Form. Key features include:
-
The ability to effortlessly edit and fill forms online without downloads.
-
eSigning capabilities streamlined for added convenience.
-
Secure document storage to protect sensitive information.
This platform enables healthcare providers to navigate the form-filling process with ease, enhancing productivity and compliance.
Taking the Next Steps with pdfFiller
By leveraging pdfFiller for your form needs, you can significantly enhance your experience with the Prior Authorization Request Form. The platform's focus on security and user-friendly features empowers both prescribers and patients to manage their healthcare documentation efficiently. Begin your journey with pdfFiller today and explore the benefits it offers.
How to fill out the prior authorization request form
-
1.To access the Prior Authorization Request Form on pdfFiller, start by visiting the pdfFiller website and using the search bar to enter the form's name. Once located, click on the form to open it in the pdfFiller editor.
-
2.Familiarize yourself with the pdfFiller interface. Use the navigation tools to scroll through the form and identify all the necessary fields that need to be completed, such as patient information, medication details, and prescriber contact information.
-
3.Before filling out the form, gather all necessary information, including patient medical history, prescriber details, and specifics about the drug being requested. Ensure you have accurate and complete data to streamline the process.
-
4.Begin filling the form by clicking on each text field to type the required information. Use checkboxes for any applicable sections and follow prompts for additional details or explanations as needed, referring to any attached instructions for guidance.
-
5.Once all fields are completed, review the entire form carefully for accuracy and completeness. Check all entries and confirm that the required signature is in place before moving to final steps.
-
6.To save your work, click on the save icon or 'Save' option found within the editor. You can download the completed form as a PDF for your records or to submit.
-
7.If submitting the form electronically, follow any specific instructions given by the healthcare organization. If faxing, ensure that you have the right fax number for Scott & White Prescription Services and confirm the transmission of the document.

Who is eligible to complete the Prior Authorization Request Form?
The Prior Authorization Request Form must be completed by licensed healthcare providers who are prescribing medication for psoriasis treatment, ensuring they provide adequate justification for the drug request.
What information is required before completing the form?
Before filling out the form, healthcare providers should gather detailed information about the patient, including their medical history, the specific medication being requested, and prescriber information.
What are the submission methods for this form?
Completed forms must be signed by the prescriber and can be faxed directly to Scott & White Prescription Services for review. Ensure all fields are filled out correctly before submission.
Are there any common mistakes to avoid while filling out this form?
Common mistakes include incomplete fields, incorrect patient information, or failure to sign the form. It's essential to double-check all entries before submission.
How long does it take to process the Prior Authorization Request?
Processing times may vary, but typically allow several days to a week for the review of a prior authorization request. It's advisable to submit early to prevent delays in medication access.
Is notarization required for this form?
No, notarization is not required for the Prior Authorization Request Form. However, ensure that the prescriber has signed the form before submitting.
Can patients fill out this form themselves?
No, patients cannot fill out the Prior Authorization Request Form themselves. It is intended to be completed and signed by a qualified healthcare provider.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.