Last updated on Oct 24, 2014

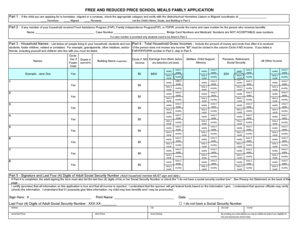
Get the free Clinical Review Pre-Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is clinical review pre-authorization request
The Clinical Review Pre-Authorization Request Form is a medical document used by healthcare providers to request pre-authorization for medical services or procedures from ConnectiCare.
pdfFiller scores top ratings on review platforms




Who needs clinical review pre-authorization request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to clinical review pre-authorization request
What is the Clinical Review Pre-Authorization Request Form?
The Clinical Review Pre-Authorization Request Form serves as a vital tool in the healthcare system, designed to streamline the authorization process for medical services and procedures. This form ensures that healthcare providers can efficiently obtain pre-authorization for necessary treatments, ultimately benefiting both providers and patients. By utilizing this medical pre-authorization form, healthcare professionals communicate effectively with insurance providers, enhancing the overall service delivery.
Purpose and Benefits of the Clinical Review Pre-Authorization Request Form
Pre-authorization is essential for healthcare providers and patients as it facilitates timely access to medical services while ensuring that the treatments are necessary and compliant with insurance policies. Using the healthcare pre-authorization template helps expedite service delivery, minimizes claim denials, and ensures proper documentation. This process not only safeguards financial resources but also enhances patient care by reducing wait times for critical procedures.
Key Features of the Clinical Review Pre-Authorization Request Form
This form includes several critical elements that simplify the pre-authorization process. Key features comprise:
-
Member and provider information sections to ensure accurate identification.
-
Procedure codes, including ICD-9, CPT, and HCPCS codes for precise billing.
-
Checkbox options for different services and procedures to streamline requests.
The inclusion of these features in the medical service authorization form significantly reduces the likelihood of errors during submission, thereby facilitating quicker approvals.
Who Needs the Clinical Review Pre-Authorization Request Form?
The Clinical Review Pre-Authorization Request Form targets healthcare providers, including clinics and hospitals in Connecticut. Professionals such as physicians, specialists, and administrative staff frequently utilize this form to ensure compliance with insurance requirements. Understanding eligibility criteria for the Clinical Review Pre-Authorization Request Form is crucial for facilitating appropriate patient care and coverage authorization.
When and How to Submit the Clinical Review Pre-Authorization Request Form
Healthcare providers should submit the Clinical Review Pre-Authorization Request Form as soon as a service requiring authorization is identified. To enhance efficiency, follow these steps for optimal submission:
-
Fill out the required fields accurately.
-
Attach all necessary supporting documents for a complete submission.
-
Submit the form either online or via fax, depending on your preference.
Being mindful of time-sensitive considerations ensures that patients receive timely care without unnecessary delays.
Required Documents and Supporting Materials
To ensure a successful submission, the following documentation is typically required:
-
Medical records related to the requested services.
-
Treatment plans highlighting the necessity of the requested procedures.
-
Any previous authorization documents, if applicable.
Using a pre-filing checklist can help streamline the preparation process, ensuring that all necessary information is gathered prior to submission.
How to Fill Out the Clinical Review Pre-Authorization Request Form Online (Step-by-Step)
To complete the Clinical Review Pre-Authorization Request Form online using pdfFiller, adhere to these detailed instructions:
-
Open the form and review each field carefully.
-
Input accurate member and provider details as required.
-
Select the appropriate checkboxes for procedures.
-
Attach all supporting documents as necessary.
-
Review your completed form to check for common errors before submission.
Common mistakes include missing fields or incorrect procedure codes, so careful review is essential to prevent issues in the authorization process.
Submission Methods and Confirmation
Completed forms can be submitted through various methods, including online and via fax. After submission, it's crucial to confirm receipt of the Clinical Review Pre-Authorization Request Form. Tracking submissions helps providers stay informed about the status and any potential follow-up requirements.
What Happens After You Submit the Clinical Review Pre-Authorization Request Form?
Once the Clinical Review Pre-Authorization Request Form is submitted, it undergoes a review process by the respective insurance provider. Possible outcomes include:
-
Approval, allowing services to proceed as planned.
-
Denial, which may require further documentation or an appeal.
-
Request for additional information from the provider.
Providers can typically check the application status through the insurance company's dedicated portal or by contacting their representatives.
Ensure Your Submission is Secure and Compliant
pdfFiller takes data security seriously, employing 256-bit encryption and complying with HIPAA and GDPR regulations to ensure the safety of sensitive medical documents. This commitment to privacy and data protection gives healthcare providers peace of mind when handling pre-authorization forms.
Empower Your Practice with Efficient PDF Management
Utilizing pdfFiller allows healthcare providers to manage their Clinical Review Pre-Authorization Request Forms effectively. With capabilities for filling out, editing, and e-signing documents, pdfFiller enhances the overall workflow, ensuring that the pre-authorization process remains smooth and efficient.
How to fill out the clinical review pre-authorization request
-
1.Access the Clinical Review Pre-Authorization Request Form by visiting pdfFiller and searching for the form by name.
-
2.Once located, click to open the form for editing within the pdfFiller interface.
-
3.Begin by gathering all necessary information such as member details, provider information, service dates, and relevant codes (ICD-9/CPT/HCPCS).
-
4.Carefully fill in each blank field, ensuring you input accurate member ID, name, and any additional details required.
-
5.Utilize the checkboxes to indicate the specific services or procedures being requested on the form.
-
6.After completing all sections, review the form for any errors or missing information to ensure completeness.
-
7.Conclude the process by saving the filled form, which can be downloaded or submitted directly through pdfFiller.
-
8.If faxing is required, ensure that the filled form is accompanied by supporting medical documentation before sending it to Clinical Review.

What are the eligibility requirements for submitting the form?
Eligibility to submit the Clinical Review Pre-Authorization Request Form typically includes being a healthcare provider treating a ConnectiCare member. Ensure that the medical services requested fall within the covered benefits.
What information do I need before completing the form?
Before completing the form, gather essential details including the member’s ID number, full name, dates of service, provider information, and relevant medical codes (ICD-9/CPT/HCPCS) to ensure accuracy.
How do I submit the completed form?
Completed forms can be submitted via fax, accompanied by necessary medical documents. If using pdfFiller, you can easily download the form to fax or submit it as instructed in the provider guidelines.
What are common mistakes to avoid when filling out the form?
Common mistakes include failing to provide complete member information, neglecting to check off required services, and submitting without necessary supporting documentation. Double-check all fields for accuracy.
Are there deadlines associated with the pre-authorization requests?
While specifics may vary, it is crucial to submit pre-authorization requests as early as possible before the scheduled service date to avoid delays in approval. Check guidelines for any specific deadlines.
What is the processing time for authorization requests?
Processing times for pre-authorization requests can vary. Generally, it may take a few business days. It is advisable to follow up with Clinical Review regarding status after submission.
What documents need to accompany the Pre-Authorization Request Form?
It is essential to include supporting medical documentation with the Pre-Authorization Request Form, which may consist of medical history, clinical notes, or previous treatment records relevant to the authorization request.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.