Last updated on Apr 10, 2026

Get the free Long-Acting Opioid Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is long-acting opioid prior authorization
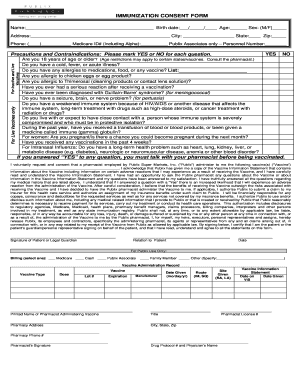
The Long-Acting Opioid Prior Authorization Request Form is a document used by healthcare providers to request prior authorization for opioid medications to ensure coverage and approval.
pdfFiller scores top ratings on review platforms




Who needs long-acting opioid prior authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to long-acting opioid prior authorization
What is the Long-Acting Opioid Prior Authorization Request Form?
The Long-Acting Opioid Prior Authorization Request Form serves as a crucial tool for healthcare providers in the management of pain through medications such as OxyContin and oxycodone CR. This form facilitates the process of gaining approval from insurance companies for the prescription of these controlled substances. By utilizing this specific authorization request form, prescribers ensure that their patients receive necessary medication while adhering to regulatory requirements.
This form is designed to simplify the process of obtaining necessary approvals, ultimately supporting effective pain management strategies. Understanding its importance can greatly enhance compliance and access to vital treatments for patients.
Purpose and Benefits of the Long-Acting Opioid Prior Authorization Request Form
Prior authorization is a requirement for certain controlled substances, making the Long-Acting Opioid Prior Authorization Request Form essential for both prescribers and patients. By completing this form, healthcare providers can assure that the prescribed medication is covered under the patient's pharmacy benefits plan.
Benefits of the form include:
-
Improved access to necessary medications for patients.
-
Streamlined communication between prescribers and insurance providers.
-
Increased likelihood of approval for medication coverage.
Ultimately, this form plays a vital role in medication authorization requests, helping ensure that treatment is both safe and effective.
Key Features of the Long-Acting Opioid Prior Authorization Request Form
The Long-Acting Opioid Prior Authorization Request Form contains several essential components that facilitate the submission process. Required fields include:
-
Member information, such as name and insurance details.
-
Provider details, including name and contact information.
-
Treatment history, outlining previous interventions and outcomes.
In addition to these fields, the form includes various checkboxes as well as specific instructions to guide the prescriber through the process effectively.
Who Needs to Use the Long-Acting Opioid Prior Authorization Request Form?
This form is intended for healthcare providers who prescribe long-acting opioid medications. Prescribers carry the responsibility of ensuring that they submit all necessary details accurately to avoid any delays in medication coverage.
Situations where this form is required include:
-
Initiating treatment with OxyContin or oxycodone CR.
-
Switching medications or altering dosages.
Understanding who needs to utilize the form ensures that pain management protocols can be followed efficiently.
How to Complete the Long-Acting Opioid Prior Authorization Request Form Online
Completing the Long-Acting Opioid Prior Authorization Request Form online using pdfFiller is straightforward. Follow these steps:
-
Access the form through pdfFiller and type in the member details.
-
Fill in the provider information accurately.
-
Document treatment history by including relevant diagnoses and previous medications.
-
Review all sections for completeness and accuracy.
-
Submit the form as instructed.
We recommend double-checking common mistakes to ensure a smooth submission process.
Submission Methods for the Long-Acting Opioid Prior Authorization Request Form
Once the Long-Acting Opioid Prior Authorization Request Form is completed, there are specific methods for submitting it to OptumRx. Providers can choose between:
-
Faxing the completed form directly to OptumRx.
-
Utilizing electronic submission methods, if available.
Understanding these submission methods is vital for ensuring timely processing of authorizations.
What Happens After You Submit the Long-Acting Opioid Prior Authorization Request Form?
After submission, the Long-Acting Opioid Prior Authorization Request Form undergoes a review process by OptumRx. Typically, this review can take a few business days, depending on the specifics of the case.
Providers can take the following actions to follow up on their submission:
-
Contact OptumRx for confirmation of receipt.
-
Inquire about the status of the authorization request.
This ongoing communication can help manage patient expectations effectively.
Security and Compliance in Handling the Long-Acting Opioid Prior Authorization Request Form
When handling the Long-Acting Opioid Prior Authorization Request Form, maintaining the privacy and security of patient information is paramount. pdfFiller employs robust security measures, including encryption, to protect sensitive data throughout the authorization process.
Additionally, compliance with regulations such as HIPAA and GDPR highlights the commitment to safeguarding personal health information, ensuring users that their data is handled with the utmost care.
Sample Completed Long-Acting Opioid Prior Authorization Request Form
Providing users with a visual reference, a sample completed Long-Acting Opioid Prior Authorization Request Form can clarify expectations for filling out the form correctly. Key areas in the example will be annotated to highlight common mistakes and aspects that must be addressed accurately.
Secure Your Prescribing Confidence with pdfFiller
The use of pdfFiller for the Long-Acting Opioid Prior Authorization Request Form enhances usability and accessibility. Features such as eSigning and comprehensive document management further support prescribers in their efforts to streamline authorization requests.
With an emphasis on security and user support, pdfFiller ensures that healthcare providers feel confident in their submission processes.
How to fill out the long-acting opioid prior authorization
-
1.Access the Long-Acting Opioid Prior Authorization Request Form by navigating to pdfFiller's website and searching for the form name.
-
2.Open the form and review the header for mandatory fields which include Member Name, Provider Name, and medication specifics.
-
3.Use the fill feature to enter the member's details, ensuring accuracy in spelling and dates.
-
4.Locate checkboxes for medical conditions relevant to the member's case and select the appropriate ones.
-
5.Collect necessary information such as treatment history and clinical diagnoses before starting the form to expedite completion.
-
6.Fill in any additional details required in the designated spaces, including prescriber attestation and clinical rationale.
-
7.Once all fields are completed, review the form for completeness and accuracy, ensuring that all required sections are filled.
-
8.Use the 'Save' feature to securely store your form after completion, then choose to 'Download' for a physical copy if required.
-
9.Finally, use the 'Submit' option to fax the completed form to OptumRx, following any specific submission instructions provided.

Who is eligible to use the Long-Acting Opioid Prior Authorization Request Form?
The form is designed for healthcare providers who prescribe long-acting opioids, such as OxyContin or oxycodone CR, requiring prior authorization for their patients.
What information is necessary to complete the form?
You will need the member’s personal details, provider information, medication specifics, and clinical information, including diagnoses and treatment history, before filling out the form.
How do I submit the completed form?
After completing the form, you can submit it by faxing it to OptumRx. Make sure to check their submission guidelines to avoid delays.
Are there any common mistakes to avoid when filling out this form?
Common mistakes include missing signature fields, incorrect medication names, and failing to provide complete clinical information, which may lead to authorization delays.
What are the processing times for prior authorization requests?
Processing times can vary but typically range from a few days to a week. Always check with the provider or insurance for specific timelines related to your request.
Do I need to notarize the Long-Acting Opioid Prior Authorization Request Form?
No, notarization is not required for this form. It should be completed and submitted directly without the need for a notary's signature.
What should I do if my authorization request is denied?
If your request is denied, contact the insurance company for clarification and ask about the appeals process to reconsider their decision.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.