Last updated on Feb 20, 2026

Get the free 497334874
Show details
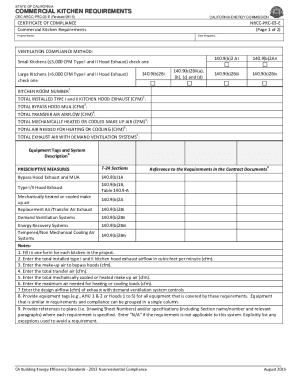
This Employment & Human Resources form covers the needs of employers of all sizes.
We are not affiliated with any brand or entity on this form
Why choose pdfFiller for your legal forms?
All-in-one solution
pdfFiller offers a PDF editor, eSignatures, file sharing, collaboration tools, and secure storage—all in one place.
Easy to use
pdfFiller is simple, cloud-based, has a mobile app, and requires no downloads or a steep learning curve.
Secure and compliant
With encryption, user authentication, and certifications like HIPAA, SOC 2 Type II, and PCI DSS, pdfFiller keeps sensitive legal forms secure.

What is introductory cobra letter
An introductory COBRA letter is a notification sent to eligible employees regarding their rights to continue health benefits under COBRA after leaving employment.
pdfFiller scores top ratings on review platforms




ok so far.
ok so far. Good for the basic editing i needed.
Everything working good!
Good document site
Good document site, however the use is not intuitively obvious.
simple to use and practical
Easy to use!
Easy to use! All interfaces worked well
good to use
good to use. but it has a watermark alongside my digital signature. don't know why.
Who needs 497334874 template?
Explore how professionals across industries use pdfFiller.
A comprehensive guide to filling out the introductory COBRA letter form
How does COBRA coverage work?
The Consolidated Omnibus Budget Reconciliation Act (COBRA) provides an important health coverage safety net for those who have recently lost their job or experienced a reduction in work hours. It allows eligible employees to continue their existing employer-sponsored health insurance for a limited time, typically up to 18 months. To benefit from COBRA, individuals must meet specific eligibility criteria and receive proper notification from their employer.
-
It provides temporary health coverage after employment termination.
-
Employees must have been part of a group health plan and qualify under the act's conditions.
-
Coverage generally lasts for 18 months but can be extended under certain circumstances.
What are the key components of the introductory COBRA letter?
An introductory COBRA letter needs to contain specific information to ensure it is processed correctly. Each component plays a vital role in the application process, helping beneficiaries know how to proceed with their COBRA health coverage.
-
Accurately entering the date is crucial for tracking deadlines.
-
Make sure to provide the correct name and address for processing the letter.
-
Clear, step-by-step instructions help beneficiaries understand how to fill out the letter.
What are the costs and coverage details?
Costs can vary substantially based on whether the coverage is for an individual or a family. Typically, the monthly premium is due by a certain date, and the coverage covers essential services such as medical, dental, and prescription drugs. It is important to understand the individual's financial responsibilities after enrollment in COBRA.
-
The monthly costs for individual COBRA coverage are generally lower than family costs.
-
Included benefits often encompass medical, dental, and prescription drug plans.
-
Failure to pay premiums on time can lead to loss of coverage.
When does COBRA coverage end?
COBRA coverage automatically ends after the maximum period of 18 months unless the beneficiary qualifies for an extension. Additionally, failure to pay premiums on time or eligibility for another employer’s health plan or Medicare can also lead to termination of COBRA benefits.
-
COBRA coverage concludes after 18 months unless special circumstances apply.
-
Neglecting to pay premiums can result in abrupt coverage loss.
-
Beneficiaries should transition to other plans as necessary once they become eligible.
Who qualifies for dependent coverage under COBRA?
Dependent coverage is a crucial aspect of the COBRA program, allowing eligible family members to secure continued health insurance. It’s essential to understand which family members qualify, how they can apply, and the events that may change their eligibility status.
-
Dependents often include spouses and children under certain circumstances.
-
Dependent children can apply for individual COBRA coverage following the group's guidelines.
-
Specific events, such as marriage or aging out, may alter a dependent's eligibility.
What steps should you take to accept your COBRA coverage?
To accept COBRA coverage, there are critical steps that must be followed within specific timeframes. Failure to adhere to these deadlines can result in loss of coverage rights, underscoring the importance of prompt action.
-
You must submit your application within 60 days upon receiving the letter.
-
Ensure that the application form is thoroughly completed and signed before submission.
-
Know whether to simply make monthly payments or do a one-time upfront payment.
How can you access further assistance?
If you have questions or need additional resources regarding COBRA coverage, reaching out to Human Resources is a beneficial first step. Providing relevant details in your correspondence can streamline the help you receive.
-
Reach out to your HR department for detailed inquiries about your COBRA coverage.
-
Make sure to include your pertinent information to expedite support.
-
Additional resources attached to the letter can support your understanding of your rights.
How does pdfFiller enhance your documentation process?
Using pdfFiller provides a seamless way to manage your COBRA documents, from editing to signing. The platform's collaborative features allow both individuals and teams to streamline their document processing in a secure cloud-based environment.
-
pdfFiller makes it easy to edit the COBRA letter without hassle.
-
The eSigning capability saves time and provides legal compliance.
-
pdfFiller allows users to share and collaborate on documents, simplifying the management process.
How to fill out the 497334874 template
-
1.Open the introductory COBRA letter template on pdfFiller.
-
2.Fill in the employee's name and address in the designated fields.
-
3.Include the date of employment termination and reason for termination in the appropriate sections.
-
4.Specify the type of health coverage the employee is eligible for under COBRA.
-
5.Clearly state the time frame in which the employee can elect to continue coverage, generally 60 days from the receipt of this letter.
-
6.Mention the premiums and payment deadlines associated with the coverage.
-
7.Add the contact information for the benefits administrator or HR representative who can answer questions.
-
8.Review the filled document for accuracy, ensuring all required fields are completed.
-
9.Save the document and send it to the employee via their preferred method of communication, such as mail or email.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.