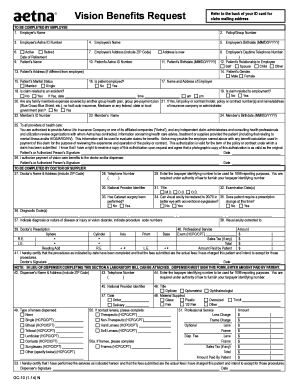
Last updated on Oct 17, 2014

Get the free Out-of-Network Vision Claim Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Vision Claim Form
The Out-of-Network Vision Claim Form is a healthcare document used by members of Blue View Vision plans to request reimbursement for vision care services received from out-of-network providers.
pdfFiller scores top ratings on review platforms




Who needs Vision Claim Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Vision Claim Form
What is the Out-of-Network Vision Claim Form?
The Out-of-Network Vision Claim Form is essential for members of Blue View Vision plans. This form facilitates the reimbursement process for vision care services received from providers outside the network. By utilizing this form, members can effectively document their vision expenditures and ensure they are compensated promptly. It is vital for members seeking to recover costs associated with their vision care, thus enhancing their overall healthcare experience.
Purpose and Benefits of the Out-of-Network Vision Claim Form
This form serves multiple purposes that significantly benefit users. First and foremost, it allows members to reclaim expenses incurred during vision-related treatments. By submitting the form, users can gain a clearer understanding of the reimbursements they are entitled to for the services they have received. Furthermore, it helps in processing claims efficiently, ensuring that benefits are utilized correctly.
Who Needs the Out-of-Network Vision Claim Form?
The Out-of-Network Vision Claim Form is primarily intended for several groups. Members of Blue View Vision plans, including both patients and their guardians, should complete this form when seeking reimbursement. It is particularly beneficial in situations where members have received care from out-of-network providers, ensuring they can access their entitled benefits seamlessly.
How to Fill Out the Out-of-Network Vision Claim Form Online (Step-by-Step)
Filling out the Out-of-Network Vision Claim Form requires careful attention. Follow these steps for successful completion:
-
Begin by entering Patient Information, including name and ID number.
-
Add the Date of Service, detailing when the vision care took place.
-
Complete the Vision Plan Information section, specifying your insurance details.
-
In the Request for Reimbursement section, input all relevant service costs.
-
Ensure you sign the form, confirming that the information provided is accurate.
Avoid common pitfalls, such as neglecting signatures or leaving sections incomplete, to ensure a smooth submission process.
Required Documents and Supporting Materials
To accompany the Out-of-Network Vision Claim Form, specific documents must be submitted. Below is a list of necessary paperwork:
-
Itemized paid receipts from the service provider.
-
Proof of service, outlining the treatments received.
-
Any additional information that the insurance plan may require.
Including complete documentation is crucial for the successful processing of claims and avoiding delays.
Submission Methods for the Out-of-Network Vision Claim Form
Members have multiple methods to submit the completed Out-of-Network Vision Claim Form. Options include:
-
Mailing the form to the specified claims address.
-
Using online submission through the Blue View Vision portal.
-
Faxing the form to the designated claims department.
To ensure your submission is received, consider following up to confirm receipt and tracking your claim status effectively.
Consequences of Not Filing or Late Filing
Failing to submit the Out-of-Network Vision Claim Form on time can lead to significant consequences. Members may lose their reimbursement claims if deadlines are missed, emphasizing the importance of timely submission. It is vital to note that claims must be submitted within one year from the date of service to qualify for reimbursement.
Common Errors and How to Avoid Them
When filling out the Out-of-Network Vision Claim Form, users often make several common errors. To avoid these mistakes, be mindful of the following:
-
Ensure all required signatures are included.
-
Review the form for any incomplete sections.
-
Double-check that all supporting documents are attached.
Utilizing a review and validation checklist before submission can significantly decrease the likelihood of errors and expedite the claims process.
How pdfFiller Can Help You with Your Out-of-Network Vision Claim Form
pdfFiller stands out as an excellent tool for completing the Out-of-Network Vision Claim Form. With its cloud-based platform, users can fill, edit, and eSign the claim form seamlessly. This ensures that sensitive information is handled securely, given pdfFiller's adherence to robust security standards, including HIPAA and GDPR compliance. Moreover, its user-friendly interface simplifies the form-filling process, enhancing the overall experience for its users.
Sample of a Completed Out-of-Network Vision Claim Form
For better understanding, users can refer to a sample of a completed Out-of-Network Vision Claim Form. This sample highlights key sections and provides annotations that explain best practices in filling out the actual form. Familiarizing yourself with a completed form can substantially ease the process of filling out your own, ensuring that you are well-prepared.
How to fill out the Vision Claim Form
-
1.Start by accessing pdfFiller and searching for the 'Out-of-Network Vision Claim Form'. You can find it easily by typing the form name in the search bar.
-
2.Once you've located the form, click to open it in pdfFiller's editing interface. Ensure that you are familiar with the layout of the form before you begin filling it out.
-
3.Gather all necessary information including patient details, vision plan information, and itemized receipts for services rendered before you start filling out the form.
-
4.Begin filling out the 'Patient Information' section with accurate details. Include the patient's name, address, and any identification numbers associated with their vision plan.
-
5.Next, move on to the 'Date of Service' field. Clearly indicate the date when the vision care services were provided. Make sure to double-check the accuracy of this date.
-
6.Fill in the 'Vision Plan Information' to specify the details of the Blue View Vision plan. This might include the policy number and any coverage details you may have.
-
7.In the 'Request For Reimbursement' section, clearly state the amount being claimed for reimbursement and provide details for each service received.
-
8.Attach the itemized paid receipts as evidence of the services provided. Ensure that all receipts are legible and match the dates and totals being claimed.
-
9.After filling in all sections, review the completed form for any errors or missing information. Ensure that everything is accurately represented.
-
10.Sign the form in the designated area, as this is mandatory for submission. If necessary, have a guardian or patient sign if they are not the primary member.
-
11.Finally, save your completed form. You can download it directly or submit it electronically through pdfFiller if supported.

Who is eligible to use the Out-of-Network Vision Claim Form?
Eligibility to use the Out-of-Network Vision Claim Form extends to members of Blue View Vision plans and their guardians or patients who received vision care from out-of-network providers.
What is the deadline for submitting this claim form?
The form must be submitted within one year from the date of service. Ensure that you keep track of your submission timeline to avoid claim denial.
How should I submit the completed form?
You can submit the completed Out-of-Network Vision Claim Form electronically through pdfFiller if available or print and mail it to the claim address provided by Blue View Vision.
What documents do I need to support my claim?
You will need itemized paid receipts for the vision care services rendered and possibly additional insurance proof if relevant. Ensure all documents are clear and complete.
What are common mistakes to avoid when filling out this form?
Common mistakes include not signing the form, providing incorrect dates, and failing to attach required receipts. Review your form thoroughly before submission to avoid these issues.
How long does processing take for vision claims?
Processing time for vision claims can vary, but generally, you can expect it to take 2 to 6 weeks after submission. Track your claim status for any updates.
What do I do if my claim is denied?
If your claim is denied, review the explanation from the insurer. You have the right to appeal the decision using the proper channels as specified in your policy.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.