Last updated on Oct 29, 2014

Get the free Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

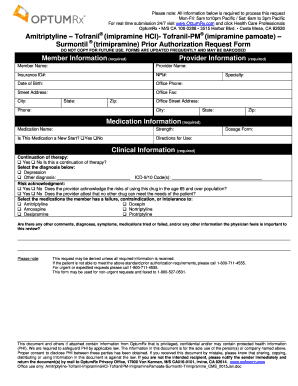
What is Prior Authorization Form
The Prior Authorization Request Form is a healthcare document used by providers to request approval from insurance companies for specific medications or treatments.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Prior Authorization Request Form?
The Prior Authorization Request Form serves a critical purpose in healthcare by enabling healthcare providers to secure necessary approvals for medications and treatments from insurance companies. This form ensures that the prescribed treatments are covered under a patient's health plan, thus preventing unexpected out-of-pocket expenses. Typically, the form requires detailed information including the patient's demographics, the medication or treatment requested, and specific diagnosis codes.
The primary use of this form is to facilitate the approval process for medications, ensuring that patients receive timely access to necessary healthcare. It includes key fields that must be accurately completed to expedite the authorization process and satisfy insurance requirements.
Purpose and Benefits of the Prior Authorization Request Form
The necessity of the Prior Authorization Request Form is twofold, benefiting both healthcare providers and patients. Firstly, it streamlines the insurance authorization process, allowing providers to allocate their time effectively while ensuring that patients receive their medications promptly. Secondly, the form helps prevent delays in treatment, which can greatly impact patient outcomes.
By using this form, healthcare providers can communicate the need for specific treatments clearly, while patients can experience a smoother transition through their healthcare journeys, knowing that they have the potential for new medications covered by insurance.
Who Needs the Prior Authorization Request Form?
The Prior Authorization Request Form is typically utilized by healthcare providers, including physicians, nurse practitioners, and other medical staff involved in patient care. Additionally, patients benefit from this form, especially in scenarios where prior authorization is a requirement for specific medical treatments or medications.
Common scenarios necessitating the use of this form include cases involving specialty medications, high-cost treatments, or new medications that have not been previously covered by insurance. Understanding the specific eligibility criteria and rules that apply is crucial for successful submissions.
How to Fill Out the Prior Authorization Request Form Online (Step-by-Step)
Filling out the Prior Authorization Request Form electronically can be achieved efficiently using pdfFiller. Below are the steps to complete the form:
-
Access the form through pdfFiller’s platform.
-
Fill in the Patient’s Name and Insurance ID accurately.
-
Enter the Date of Birth and other required demographic information.
-
Provide details of the medication or treatment requested.
-
Review all entries for accuracy before submission.
To ensure completeness, double-check all fields, as missing or incorrect information can lead to delays in the approval process.
Field-by-Field Instructions for the Prior Authorization Request Form
Completing the Prior Authorization Request Form correctly is critical. Each section of the form has specific requirements:
-
Patient's Information: Include full name, date of birth, and insurance details.
-
Medication Details: Specify the requested medication, dosage, and prescribing physician.
-
Diagnosis Codes: Clearly indicate relevant diagnosis codes accompanying the treatment request.
Common mistakes to avoid include entering incorrect patient information, neglecting to include all required fields, and failing to sign where applicable. Ensuring that each field is meticulously filled reduces the likelihood of rejection.
Submission Methods for the Prior Authorization Request Form
Once the Prior Authorization Request Form is completed, it can be submitted through various methods. Predominantly, healthcare providers can fax the completed form to OptumRx or submit it electronically via insurance company portals.
It is essential to adhere to submission guidelines, such as whether to include additional documentation or specific references. Confirming receipt of the submission with the insurance provider is critical to ensure it is processed timely.
What Happens After You Submit the Prior Authorization Request Form?
Following the submission of the Prior Authorization Request Form, insurance companies undertake a review process. They evaluate the request to determine coverage based on medical necessity.
Typically, providers should expect communication regarding the approval status within several business days. Tracking the status of the request ensures that any additional information required is promptly supplied, helping avoid unnecessary delays in patient care.
Common Issues and Solutions with Prior Authorization Requests
Frequently encountered issues with prior authorization requests include rejections due to incomplete information or lack of clinical justification. Addressing these issues often involves contacting the insurance provider to clarify requirements and submitting necessary documentation.
If a request is denied, understanding the steps for renewal or resubmission is vital. Providers should be prepared to revise requests with additional information and justification to improve the chances of successful authorization.
Security and Compliance for the Prior Authorization Request Form
Data protection is paramount when handling the Prior Authorization Request Form, given the sensitivity of patient information involved. pdfFiller ensures robust security measures with 256-bit encryption and maintains compliance with HIPAA regulations, safeguarding personal health information.
During the completion and submission of the form, adhering to privacy considerations is essential. Healthcare providers must ensure that all data is handled confidentially to maintain compliance with healthcare regulations.
Enhance Your Experience with pdfFiller
Utilizing pdfFiller for filling out the Prior Authorization Request Form offers numerous benefits, such as electronic signing, streamlined document management, and real-time editing features. These capabilities enable users to handle their forms efficiently, minimizing time spent on administrative tasks.
Cloud-based solutions provided by pdfFiller facilitate seamless access and sharing of documents from any location. Positive user outcomes highlight the effectiveness of pdfFiller in simplifying healthcare form processing.
How to fill out the Prior Authorization Form
-
1.Access pdfFiller and search for the Prior Authorization Request Form using the search bar.
-
2.Open the form by clicking on its link in the search results.
-
3.Familiarize yourself with the layout of the form, including fillable fields and checkboxes.
-
4.Gather patient information such as the Patient's Name, Insurance ID, and Date of Birth before starting.
-
5.Begin filling in the form by clicking on each field and entering the necessary information.
-
6.Use the instructions provided in the form to ensure you include all required details.
-
7.For sections needing a checkmark, click the appropriate checkbox for 'Yes' or 'No' responses.
-
8.Review the information completed to avoid errors, ensuring all fields are filled adequately.
-
9.Once satisfied with the information entered, finalize your form by checking for completeness.
-
10.Save your form by clicking the save option, then choose to download it in your desired format or submit it as indicated.

Who is eligible to use the Prior Authorization Request Form?
The Prior Authorization Request Form is primarily for healthcare providers seeking approval for medications or treatments, but patients may also need it to facilitate their medication coverage through their insurance.
What information do I need to fill out the form?
You will need detailed patient information such as name, insurance ID, date of birth, medication details, and diagnosis codes to accurately complete the Prior Authorization Request Form.
How do I submit the completed form?
After completing the form, it should be faxed to OptumRx for coverage determination as instructed in the form submission guidelines.
Is notarization required for this form?
No, the Prior Authorization Request Form does not require notarizing before submission, which simplifies the process for healthcare providers.
What common mistakes should I avoid when filling out the form?
Ensure all sections are accurately filled, including patient details and medication information, and double-check for any missed signatures to avoid delays in processing.
What is the processing time for the Prior Authorization Request?
The processing time can vary depending on the insurance provider but typically ranges from a few hours to a few days after submission. It's wise to follow up if you don't receive confirmation.
Can I edit the form once I've started filling it out?
Yes, you can edit the form at any time while using pdfFiller. Just click on the field you want to change and update the information accordingly before finalizing.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.