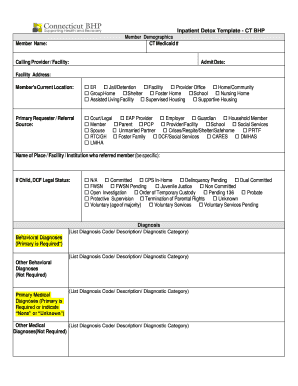
Last updated on Nov 7, 2014

Get the free COBRA Continuation Coverage Denial Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is COBRA Denial Form
The COBRA Continuation Coverage Denial Form is a government document used by applicants to document reasons for denying COBRA continuation coverage under the American Recovery and Reinvestment Act (ARRA).
pdfFiller scores top ratings on review platforms




Who needs COBRA Denial Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to COBRA Denial Form
What is the COBRA Continuation Coverage Denial Form?
The COBRA Continuation Coverage Denial Form is a crucial document that provides a detailed reasoning behind the denial of COBRA coverage, which relates to the Consolidated Omnibus Budget Reconciliation Act (COBRA). This legislation allows individuals to maintain health coverage following employment termination under specific circumstances. It is significant for applicants seeking to understand the reasons behind their denial of COBRA coverage.
This denial form serves a unique purpose by documenting the precise reasons for denying coverage. Additionally, it is essential for the form to be signed under penalty of perjury, underscoring the importance of the applicant's honesty when providing information.
Purpose and Benefits of the COBRA Continuation Coverage Denial Form
Utilizing the COBRA Continuation Coverage Denial Form comes with various advantages that benefit both applicants and insurers alike. This form aids applicants in comprehending their denial decisions, providing a structured format to help them prepare for any necessary appeal processes.
Moreover, it creates a formal record that can be referenced by insurers and employers, ensuring that all parties are aligned on the reasons for denial. In addition, utilizing the denial form guarantees compliance with the American Recovery and Reinvestment Act’s regulations, protecting the rights of individuals facing denials.
Who Needs the COBRA Continuation Coverage Denial Form?
The individuals in need of the COBRA Continuation Coverage Denial Form are primarily those whose COBRA continuation coverage has been denied. This situation commonly arises due to various reasons, such as failure to comply with requisite eligibility criteria.
Employers also play a critical role in this context, as they are obligated to issue the denial form when appropriate. Understanding who requires the form ensures that the right parties are informed and equipped to take the next necessary steps following a denial.
How to Fill Out the COBRA Continuation Coverage Denial Form Online (Step-by-Step)
Filling out the COBRA Continuation Coverage Denial Form online can be efficiently completed using pdfFiller. Here are the steps to follow:
-
Access the COBRA continuation coverage form on pdfFiller.
-
Complete the applicant details section, ensuring accuracy in names and contact information.
-
Provide a detailed denial rationale, clearly stating the reasons for coverage denial.
-
Double-check all filled fields for completeness and accuracy.
-
Sign the form electronically, as required by law.
Accurate information is crucial throughout the process to avoid complications and ensure the validity of the denial form.
Common Errors and How to Avoid Them When Filling Out the COBRA Continuation Coverage Denial Form
Minimizing mistakes during form completion is vital. Here are common pitfalls to be aware of:
-
Missing signatures can lead to immediate rejection of the form.
-
Incorrect dates might cause legal challenges in processing.
-
Incomplete applicant details can delay the denial process.
Tips for avoiding these mistakes include carefully reviewing the form before submission, ensuring all required fields are filled, and confirming that corresponding dates match. Such diligence can significantly impact the likelihood of a successful appeal.
Submission Methods for the COBRA Continuation Coverage Denial Form
Once the COBRA Continuation Coverage Denial Form is completed, there are various submission methods available:
-
Online submission through pdfFiller provides convenience and quick processing.
-
Traditional mail is another option; however, it may take more time.
-
Check for any associated fees or submission deadlines that could affect processing.
It is crucial to keep a record of the submission method used as a reference for any future inquiries regarding the form.
What Happens After You Submit the COBRA Continuation Coverage Denial Form?
Setting expectations post-submission is important. Here’s an overview of what typically happens:
-
The processing timeline may vary depending on the employer or insurance provider.
-
Outcomes can include a confirmation of denial or a request for further information.
-
If the denial is upheld, individuals may need to consider an appeal process or seek alternative coverage options.
Understanding these potential scenarios helps applicants prepare for subsequent actions based on the response received.
Security and Compliance for the COBRA Continuation Coverage Denial Form
Ensuring the protection of sensitive data when using the COBRA Continuation Coverage Denial Form is paramount. pdfFiller implements robust security measures, such as:
-
256-bit encryption to safeguard personal information during transmission.
-
Compliance with regulations like HIPAA and GDPR, ensuring that user data is handled responsibly.
This commitment to privacy instills confidence in users about the safety of their information throughout the process.
Use pdfFiller to Streamline Your COBRA Continuation Coverage Denial Process
Leveraging pdfFiller for completing the COBRA Continuation Coverage Denial Form can significantly streamline the process. Some key benefits include:
-
The ability to eSign forms quickly and securely.
-
Online editing features that allow for easy corrections and adjustments.
-
User testimonials highlight successful experiences with the platform.
Begin using pdfFiller today to enhance your experience in creating and submitting the COBRA form effortlessly.
How to fill out the COBRA Denial Form
-
1.To access the COBRA Continuation Coverage Denial Form on pdfFiller, visit their website and use the search functionality to find the specific form by name.
-
2.Once the form is open in the pdfFiller interface, begin by reviewing the instructions at the top to understand each section’s requirements.
-
3.Gather all necessary information before filling out the form, including details about the applicant, reasons for denial, and significant dates related to the coverage.
-
4.Navigate to each fillable field and click on them to enter the required information; pdfFiller allows you to type directly into the fields easily.
-
5.Utilize the checkboxes where applicable to indicate specific denial reasons; these help clarify the situation for future reference.
-
6.After completing the form, review all entries to ensure accuracy and completeness, especially the critical details like dates and names.
-
7.Once satisfied with your form, click on the 'Preview' option to see a final view before signing.
-
8.To finalize the form, sign it directly on pdfFiller, which provides an electronic signature option.
-
9.Finally, save the completed form to your device, download it for submission, or utilize pdfFiller’s options to submit directly if applicable.

Who is eligible to use the COBRA Continuation Coverage Denial Form?
Any individual who has been denied COBRA continuation coverage, along with their employers or legal representatives, can use this form to document the reasons for denial.
What supporting documents do I need to submit with my COBRA Denial Form?
Typically, you will need to include any relevant documentation that supports the reasons for denial, such as health plan termination details and notices sent to the applicant.
Are there deadlines for submitting the COBRA Continuation Coverage Denial Form?
It is crucial to submit the form as soon as possible after the denial of coverage, typically within 30 days of the denial, to ensure compliance and to maintain eligibility.
What common mistakes should I avoid when filling out the COBRA Denial Form?
Common mistakes include incomplete fields, missing signatures, and not providing sufficient supportive details. Double-check all information before submission.
How can I submit the COBRA Denial Form once completed?
You can submit the form via mail to the relevant health plan administrator or through an electronic submission option if available, using pdfFiller for direct sending.
What is the processing time for COBRA Denial Forms?
Processing times can vary, but generally, you should allow a few weeks for the health benefits provider to review your denial reason and respond appropriately.
Is notarization required for the COBRA Continuation Coverage Denial Form?
No, notarization is not required for this form; however, it must be signed under penalty of perjury.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.