Last updated on Dec 25, 2014
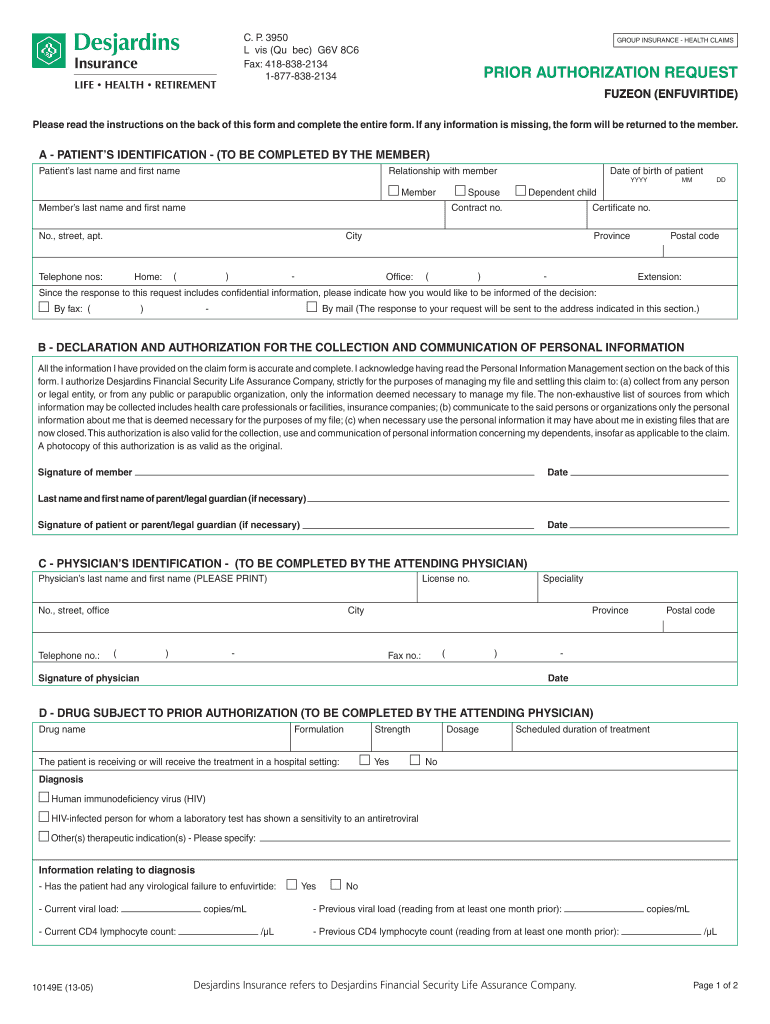

Get the free Group Insurance Health Claims Prior Authorization Request
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Health Claims Form
The Group Insurance Health Claims Prior Authorization Request is a medical document used by patients and their healthcare providers to obtain prior authorization for the drug Fuzeon for HIV treatment in Quebec, Canada.
pdfFiller scores top ratings on review platforms




Who needs Health Claims Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Health Claims Form
What is the Group Insurance Health Claims Prior Authorization Request?
The Group Insurance Health Claims Prior Authorization Request form is a crucial document in Quebec, Canada, used to request prior authorization for Fuzeon (Enfuvirtide), an essential medication for HIV treatment. This form plays a significant role in the healthcare process, ensuring that patients who may benefit from this medication receive timely access. It must be completed and signed by the member, patient or guardian, and physician, guaranteeing that all necessary stakeholders are involved in the request.
In summary, the health claims form streamlines the prior authorization request process, making it essential for those needing Fuzeon to adhere to healthcare insurance policies.
Purpose and Benefits of the Group Insurance Health Claims Prior Authorization Request
The Group Insurance Health Claims Prior Authorization Request is necessary for several reasons. Firstly, it ensures that eligible patients have timely access to crucial medications, such as Fuzeon, thereby improving treatment outcomes. Furthermore, this form protects patient rights and ensures that requests are compliant with health insurance policies, helping patients navigate the often-complex healthcare landscape.
In conclusion, the benefits of prior authorization go beyond mere compliance; they foster improved healthcare experiences for patients in Quebec who are managing serious health conditions.
Key Features of the Group Insurance Health Claims Prior Authorization Request
The Group Insurance Health Claims Prior Authorization Request form boasts user-friendly features that facilitate efficient completion. These features include:
-
Multiple fillable fields and checkboxes enhancing usability.
-
Sections dedicated to patient identification, allowing for accurate data entry.
-
Specific areas for physician identification and drug information relevant to Fuzeon.
These aspects contribute to a streamlined experience, making it easier for users to fill out the physician authorization form correctly.
Who Needs to Complete the Group Insurance Health Claims Prior Authorization Request?
Several key stakeholders are involved in completing the Group Insurance Health Claims Prior Authorization Request form, which requires signatures from:
-
The member, who is typically the policyholder.
-
The patient or their parent/legal guardian.
-
The physician prescribing the medication.
Each of these roles is critical in the submission process, ensuring that all necessary information is provided for a successful authorization request.
How to Fill Out the Group Insurance Health Claims Prior Authorization Request Online
Filling out the Group Insurance Health Claims Prior Authorization Request online can be accomplished by following these steps:
-
Begin by accessing the form on the appropriate platform.
-
Carefully fill in each section, ensuring accurate information is provided.
-
Review the form for potential errors, paying special attention to required fields.
-
Submit the completed form via the preferred method outlined in the submission guidelines.
Additionally, be aware of common pitfalls that can lead to errors to avoid unnecessary delays in processing.
Submission Methods for the Group Insurance Health Claims Prior Authorization Request
Once the Group Insurance Health Claims Prior Authorization Request form is completed, it can be submitted through various methods:
-
Online via the designated healthcare portal.
-
By mail to the appropriate insurance provider's address.
-
By fax, if this option is available.
It is crucial to be mindful of important deadlines and processing times associated with each submission method to ensure timely authorization.
What Happens After You Submit the Group Insurance Health Claims Prior Authorization Request?
After submitting the Group Insurance Health Claims Prior Authorization Request, applicants can expect to undergo a review process managed by the insurer. During this time, users have the ability to track the status of their application. In the event of a potential rejection, understanding common rejection reasons can assist individuals in improving their next submission.
It is advisable for applicants to remain proactive and familiar with the renewal or resubmission process to mitigate any disruptions in accessing necessary treatments.
Security and Compliance for Handling the Group Insurance Health Claims Prior Authorization Request
When handling the Group Insurance Health Claims Prior Authorization Request, security and compliance are of utmost importance. The form utilizes robust security measures, including 256-bit encryption, and complies with HIPAA standards to ensure that sensitive personal and health information is adequately protected.
Maintaining privacy and data protection when submitting the form not only fosters trust but also adheres to legal requirements, safeguarding the information of all parties involved.
How pdfFiller Can Help You Complete the Group Insurance Health Claims Prior Authorization Request
pdfFiller offers a user-friendly platform tailored to assist users in completing the Group Insurance Health Claims Prior Authorization Request. Key benefits of using pdfFiller include:
-
Easy editing and filling of the health claims form.
-
Secure eSigning capabilities to finalize the document.
-
Accessibility from any browser, eliminating the need for downloads.
This document management platform streamlines the process, making it simple and efficient for users to facilitate their authorization requests.
Example of a Completed Group Insurance Health Claims Prior Authorization Request
Providing an example of a completed Group Insurance Health Claims Prior Authorization Request can be invaluable for users. A visual sample of a filled-out form, complete with annotations, serves as an effective reference.
Each section can be explained using the sample to guide users in understanding how to fill out their forms accurately, facilitating a smoother submission process.
How to fill out the Health Claims Form
-
1.Access the Group Insurance Health Claims Prior Authorization Request form on pdfFiller by typing the name in the search bar or navigating through the Healthcare Forms section.
-
2.Once the form is opened, familiarize yourself with the fillable fields by scrolling through the document using the navigation pane.
-
3.Gather necessary information such as patient identification details, physician information, and specific drug information to expedite the filling process.
-
4.Begin by entering the patient's details in the designated fields using pdfFiller's interactive interface, ensuring all required information is accurately provided.
-
5.Next, complete the physician section with accurate identification details. Be sure to check for any specific instructions for this part of the form.
-
6.Fill in the drug information section, specifically for Fuzeon, including dosage and any other relevant details that may be requested.
-
7.After completing all fields, carefully review the information inputted to ensure accuracy and completeness. Look for any highlighted areas indicating missing information.
-
8.Once verified, navigate to the signature fields, ensuring all required parties—member, patient or guardian, and physician—can sign electronically using pdfFiller's signature tools.
-
9.Finalize the form by selecting 'Save' to keep the document in your pdfFiller account, or choose 'Download' to save it locally to your device.
-
10.If submission is required, follow the instructions provided in your group's insurance plan for sending the completed form. You may also submit directly via pdfFiller, if an integrated submission option is available.

Who needs to sign the Group Insurance Health Claims Prior Authorization Request?
The form requires signatures from the member, the patient or their legal guardian, and the physician to ensure that all parties agree to the consent and information provided.
What information is necessary to complete the form?
You will need patient identification details, physician information, and specific drug details pertaining to Fuzeon. It's wise to gather these details before starting to complete the form.
How can I submit the completed authorization request?
Submission methods may vary by insurance provider. Typically, the form can be submitted via mail, fax, or through the insurance provider's online portal. Check your insurance guidelines for specific submission methods.
Are there any deadlines for submitting the authorization request?
While specific deadlines can vary by provider, it's advisable to submit the authorization request as soon as possible to avoid delays in receiving treatment. Check with your insurance for specific timelines.
What are some common mistakes to avoid when filling out this form?
Common mistakes include missing signatures, failing to provide complete information, or leaving required fields blank. Always double-check your entries before finalizing the form.
How long does it take to process a prior authorization request?
Processing times for prior authorization requests can vary widely, typically ranging from a few days to a couple of weeks. It's best to follow up with your insurance company for updates.
Will I need to provide supporting documents with the form?
Supporting documents may include medical records or previous treatment histories. Check with your insurer to see what additional documentation may be required for this authorization request.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.