Last updated on Jun 17, 2012

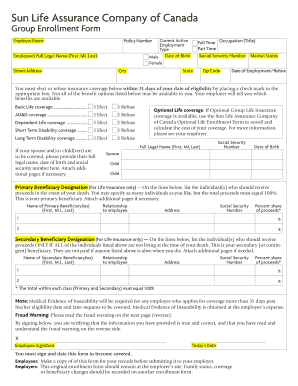
Get the free ARRA Premium Reduction Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is arra premium reduction request
The ARRA Premium Reduction Request Form is a healthcare document used by individuals who have experienced an involuntary loss of employment to apply for a reduction in COBRA premiums.
pdfFiller scores top ratings on review platforms




Who needs arra premium reduction request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to arra premium reduction request
What is the ARRA Premium Reduction Request Form?
The ARRA Premium Reduction Request Form is essential for individuals who have faced involuntary job loss, allowing them to apply for a reduction in COBRA premiums. This form was created during a specific historical context, related to the events between September 2008 and May 2010. To be valid, the form must be signed by the employee, dependents, and the employer or plan administrator. It plays a crucial role in assisting individuals who need financial relief through lowered health insurance premiums.
Purpose and Benefits of the ARRA Premium Reduction Request Form
Using the ARRA Premium Reduction Request Form is vital for individuals who have lost their jobs involuntarily. The form not only facilitates the application for premium reductions but also offers significant financial relief by allowing access to reduced health insurance premiums. It can ease the burden on those struggling with unexpected unemployment, helping ensure they maintain health coverage during challenging times.
Who Needs the ARRA Premium Reduction Request Form?
This form is intended for a variety of individuals connected to the employment and health coverage process. Employees who have experienced an involuntary loss of employment, their dependents who are eligible for COBRA, and employers or plan administrators are all included in the eligibility criteria. Specific scenarios that warrant filing include layoffs and terminations, whereby individuals are qualified for the benefits the form provides.
How to Fill Out the ARRA Premium Reduction Request Form Online (Step-by-Step)
Completing the ARRA Premium Reduction Request Form online through pdfFiller is straightforward. Follow these step-by-step instructions:
-
Access the form in pdfFiller.
-
Fill in the personal information section, which includes your name and address.
-
Enter employment details, including the date of job loss.
-
Review all the required fields for accuracy.
-
Obtain necessary signatures from yourself, your dependents, and your employer.
-
Finalize and save the document for submission.
Common Errors and How to Avoid Them When Filing the ARRA Form
When filling out the ARRA Premium Reduction Request Form, recognizing common errors is key to a successful submission. Frequent mistakes include leaving fields incomplete or failing to provide the required signatures. To mitigate these issues, verify the following:
-
All required fields are filled out completely.
-
Signatures are provided where necessary.
-
The information entered matches documentation and is accurate.
Submission and Delivery of the ARRA Premium Reduction Request Form
Once the ARRA Premium Reduction Request Form is completed, several submission methods are available. Individuals can submit the form online using pdfFiller, which streamlines the process. Alternatively, the form can be mailed or faxed, depending on your preference and the requirements set forth by your employer or plan administrator.
What Happens After You Submit the ARRA Premium Reduction Request Form?
After submission, applicants can expect a confirmation and tracking of the application status. This process typically involves a response from the relevant authority. It is essential to stay informed about potential timelines for application processing, ensuring any necessary follow-ups are conducted promptly.
Security and Compliance When Handling the ARRA Premium Reduction Request Form
pdfFiller prioritizes security and compliance when managing sensitive information associated with the ARRA Premium Reduction Request Form. They implement security measures such as 256-bit encryption and comply with HIPAA and GDPR regulations. This commitment to data protection is crucial for safeguarding personal health information throughout the submission process.
Get Started with pdfFiller to Complete Your ARRA Premium Reduction Request Form
pdfFiller offers a user-friendly platform for filling out and submitting the ARRA Premium Reduction Request Form. Users can take advantage of features such as editing, eSigning, and secure storage options. With a focus on ease of use and security, pdfFiller simplifies the process, making it accessible for all users needing to navigate health insurance applications.
How to fill out the arra premium reduction request
-
1.Access the ARRA Premium Reduction Request Form on pdfFiller by searching for it in the document library.
-
2.Click to open the form in editable mode, where you can fill in the required fields directly.
-
3.Before starting, gather necessary personal information, including your name, address, and details surrounding your employment loss.
-
4.Use the mouse to click on each blank field to enter your information as prompted by the form.
-
5.Check the box next to any statements that apply to you, ensuring all selections are accurate and complete.
-
6.Review the entire form after filling out, checking for any missing or incorrectly entered information.
-
7.Finalize the form by ensuring all required signatures are included, especially from you, your dependents, and your employer or plan administrator.
-
8.Save your completed form on pdfFiller by using the save option or download it directly to your device for submission.

Who is eligible to use the ARRA Premium Reduction Request Form?
Individuals who have lost their employment involuntarily and wish to seek a reduction in COBRA premiums can use this form. Eligibility is typically linked to specific job loss circumstances and COBRA continuation coverage.
What is the deadline for submitting this form?
Though the form references events that occurred from September 1, 2008, to May 31, 2010, check current regulations for any relevant deadlines regarding healthcare premium reductions or COBRA enrollment.
How can I submit the completed ARRA Premium Reduction Request Form?
Once completed, you can submit the form to your employer or the plan administrator handling your COBRA coverage. Some may also allow electronic submissions, so confirm their preferences.
What supporting documents are required when submitting the form?
Typically, you may need to provide identification and documentation proving your involuntary job loss. Check with your employer for specific requirements.
What common mistakes should I avoid when completing this form?
Ensure all fields are filled out accurately, double-check that all required signatures are present, and confirm the details about your employment loss match provided documentation.
How long does it take to process the ARRA Premium Reduction Request Form?
Processing times can vary; typically, you should expect a response within a few weeks. Follow up with your employer for specific timelines.
Where can I find more information about COBRA and premium reductions?
Visit the official COBRA website or consult your HR department for detailed information on COBRA eligibility, rights, and premium reduction application processes.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.