Last updated on Mar 25, 2015

Get the free COBRA Continuation of Coverage Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

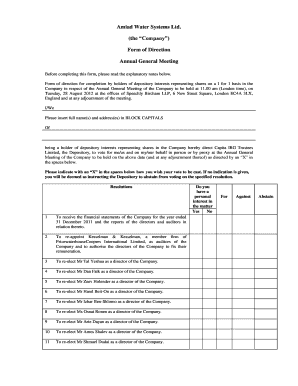
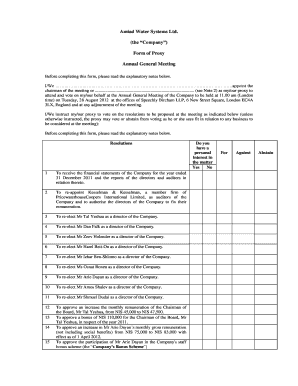
What is COBRA Form
The COBRA Continuation of Coverage Form is a legal document used by employees and employers in Louisiana to continue health insurance coverage under COBRA regulations.
pdfFiller scores top ratings on review platforms




Who needs COBRA Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to COBRA Form
What is the COBRA Continuation of Coverage Form?
The COBRA Continuation of Coverage Form is vital for allowing eligible employees, along with their spouses and children, to continue their health insurance coverage after employment ends. Under COBRA and state group continuation laws, this document plays a crucial role in ensuring that individuals maintain necessary health benefits. The form is indispensable not only for employees, who wish to secure ongoing coverage, but also for employers, who are required to facilitate this process.
Why You Need the COBRA Continuation of Coverage Form
Filling out the COBRA continuation form offers significant benefits that protect your health coverage after you leave a job. By completing this form, you can obtain essential healthcare services without interruption. Conversely, failing to file the form may result in loss of coverage and potential legal consequences for employers who overlook their obligations under COBRA regulations.
Who Should Complete the COBRA Continuation of Coverage Form?
The COBRA Continuation of Coverage Form must be completed by eligible employees, including their spouses and dependent children. Employers have specific obligations regarding this form, as they are responsible for providing it to eligible employees in a timely manner. Both the employee and employer play vital roles in the smooth completion of this essential document.
How to Fill Out the COBRA Continuation of Coverage Form
To fill out the COBRA continuation form correctly, follow these step-by-step instructions:
-
Begin by entering the 'NAME OF GROUP' as it appears on the policy.
-
Input the 'GROUP POLICY NO.' to identify your specific insurance plan.
-
Detail the 'REASON(S) FOR GROUP COVERAGE ENDING,' ensuring accurate information.
-
Complete all required fields, ensuring clarity and accuracy.
-
Review the form to avoid common errors, such as missing signatures from both employee and employer.
Submission and Processing of the COBRA Continuation of Coverage Form
Upon completing the COBRA continuation form, it's essential to know how to submit it properly. Choose among various submission methods, such as:
-
Mailing the form to the designated employer address.
-
Utilizing electronic submission options if available.
Take note of any associated fees, deadlines for submission, and processing times. To ensure a smooth process, familiarize yourself with the confirmation methods and how to track the status of your submission.
Security and Compliance When Handling the COBRA Continuation of Coverage Form
Given the sensitive nature of the information on the COBRA continuation form, security and compliance are paramount. pdfFiller employs robust security measures, including 256-bit encryption, to protect personal and health information. Additionally, it adheres to industry standards such as HIPAA and GDPR to uphold privacy and data protection principles.
Utilizing pdfFiller for Completing the COBRA Continuation of Coverage Form
pdfFiller is an excellent tool for simplifying the process of completing the COBRA continuation form. It allows users to easily edit, fill, and eSign their forms using a cloud-based solution. This platform streamlines document management, making it easier for both employees and employers to handle form submissions efficiently and securely.
Commonly Asked Questions & Concerns About the COBRA Continuation of Coverage Form
Many users have common inquiries regarding the COBRA continuation form, including eligibility, filing processes, and deadlines. It is essential to address these concerns proactively, as understanding the nuances of COBRA coverage can mitigate confusion. Should any additional questions arise, reaching out for assistance using pdfFiller can provide the necessary guidance.
Sample Completed COBRA Continuation of Coverage Form
To further assist users, a sample completed COBRA continuation form illustrates how to fill it out correctly. This visual guide highlights key fields and demonstrates proper entries, assisting users in understanding the form's layout and specific requirements. Familiarity with the example can enhance accuracy in form completion.
Get Started With Your COBRA Coverage Today
Completing the COBRA Continuation of Coverage Form accurately is crucial for securing ongoing health insurance coverage. Using pdfFiller can streamline this process, offering a secure and efficient means of managing necessary documentation. Explore additional resources available through pdfFiller to support you on your journey toward maintaining your health coverage.
How to fill out the COBRA Form
-
1.Begin by accessing pdfFiller and searching for the COBRA Continuation of Coverage Form. You can find it by entering relevant keywords or the exact form name in the search bar.
-
2.Once located, click on the form to open it. The pdfFiller interface will allow you to view and fill out the document easily.
-
3.Before you start filling in the COBRA form, gather all necessary information such as your group policy number, names, and contact details of the continuing employee, and reason for the coverage termination.
-
4.Use the pdfFiller interface to click on each field, and type in the required information. All fields marked with an asterisk are mandatory, so ensure to complete them.
-
5.If you need to fill out multiple sections, maintain your progress by navigating through the form with the previous and next buttons provided in pdfFiller.
-
6.After you finish filling in the COBRA form, review all details carefully to verify the accuracy of the information provided, including spelling names and numbers.
-
7.To finalize the form, make sure both the employee and employer sign in the designated signature fields. You can use pdfFiller's signature feature for this.
-
8.Once reviewed, save your form within pdfFiller. You also have the option to download it or submit it directly to your employer through the platform.

What is the eligibility requirement for using the COBRA form?
Employees who have recently experienced a qualifying event, such as job termination or reduction in hours, are eligible to use the COBRA Continuation of Coverage Form to maintain health insurance.
Are there any deadlines I should be aware of?
Yes, individuals must submit the COBRA form within 60 days of the qualifying event to ensure their continuation of coverage is not jeopardized.
How do I submit the completed COBRA form?
Once completed, the COBRA form should be signed by both the employee and employer and then submitted to the employer or designated COBRA administrator as instructed.
What supporting documents are needed with the COBRA form?
Typically, you will need to provide the reason for coverage ending, details about the group policy, and any relevant personal identification information for the continuing employee or family members.
What common mistakes should I avoid when filling out the COBRA form?
Be sure to fill in all mandatory fields, double-check the signatures of both parties, and ensure that the information provided is accurate to avoid processing delays.
How long does it take to process the COBRA form?
Processing times can vary, but typically allow 30 days for the employer to notify you of your coverage options once your COBRA form is submitted.
Who can assist me if I have questions about the COBRA form?
You can contact your employer's HR department or the COBRA administrator for assistance with any specific questions you may have about the form or the continuation process.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.