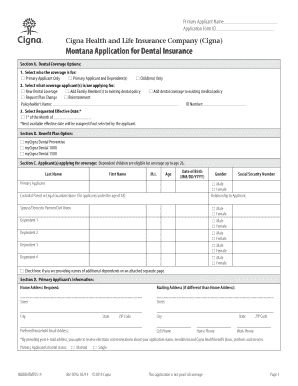
Get the free COBRA Coverage Application
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is COBRA Application
The COBRA Coverage Application is a healthcare form used by employees in Nebraska to apply for continued insurance coverage after termination or reduction in hours.
pdfFiller scores top ratings on review platforms




Who needs COBRA Application?
Explore how professionals across industries use pdfFiller.
How to fill out the COBRA Application
-
1.Access the COBRA Coverage Application on pdfFiller by searching for the form in the platform's search bar or uploading your own copy.
-
2.Once the form is open, navigate through the fillable fields using tooltips for guidance on what information is required in each section.
-
3.Gather necessary information, including your full name, Social Security Number, address, and phone number, before filling out the form to ensure accuracy.
-
4.Fill in all required fields thoroughly, including agreeing to the continuation or termination of your insurance coverage by checking the relevant boxes provided.
-
5.Carefully review each section of the form for any errors or omissions, using pdfFiller's spell check and review features to ensure clarity.
-
6.Once satisfied with the completed form, finalize it by clicking on the 'Submit' button or printing it for physical submission as per provided instructions.
-
7.To save or download the completed form, select 'Save As' from the menu and choose your preferred file format before storing it securely.

What are the eligibility requirements for COBRA coverage?
Eligibility for COBRA coverage typically includes employees who have experienced job loss or reduced hours. Consistent payment of premium and qualifying conditions such as disability may also affect eligibility.
Are there specific deadlines I need to be aware of?
Yes, it’s crucial to submit your COBRA Coverage Application promptly after employment ends. Generally, you have 60 days to elect coverage from the date of a qualifying event.
How do I submit the completed COBRA Coverage Application?
You can submit the completed form electronically through pdfFiller or print it for mailing. Ensure that you follow any specific submission instructions included with the form.
What supporting documents do I need to provide with the application?
Typically, you will need to provide a copy of your termination notice or proof of reduced hours along with the COBRA Coverage Application.
What are common mistakes to avoid when filling out the form?
Common mistakes include omitting personal information, not checking the box for continuation or termination correctly, and failing to sign and date the form.
How long does it take to process my COBRA application?
Processing times can vary. Generally, you should receive a confirmation of your application within 30 days of submission.
What should I do if I have concerns about my COBRA form?
If you have concerns, reach out to your HR department or insurance provider for clarification. You can also consult with a legal advisor specializing in health insurance matters.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.