Last updated on Feb 26, 2015

Get the free Prior Authorization Form for Zoladex
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Zoladex Prior Authorization
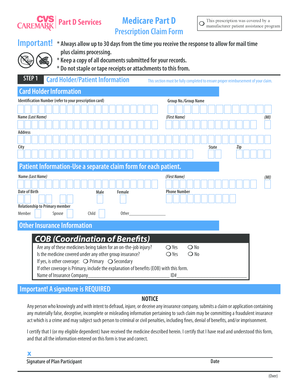
The Prior Authorization Form for Zoladex is a medical consent document used by healthcare providers to request approval from CVS Caremark for the prescription of Zoladex.
pdfFiller scores top ratings on review platforms




Who needs Zoladex Prior Authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Zoladex Prior Authorization
What is the Prior Authorization Form for Zoladex?
The Prior Authorization Form for Zoladex serves as a crucial bridge between healthcare providers and insurance companies. This form is specifically designed to facilitate the approval process for the prescription of Zoladex, a medication commonly used in prostate cancer treatment, breast cancer treatment, and for conditions requiring endometrial thinning.
Completing the Prior Authorization Form is a significant aspect of the healthcare process. It ensures that prescribed medications are covered by insurance, validating their necessity based on medical guidelines. This not only helps patients receive timely care but also assists prescribers in navigating insurance requirements effectively.
Purpose and Benefits of the Prior Authorization Form for Zoladex
The necessity of the Prior Authorization Form for Zoladex cannot be understated. It is a requirement for patients seeking coverage for Zoladex, making it essential for obtaining the medication. This form streamlines the approval process, ultimately benefiting patient care by reducing delays in treatment.
Utilizing this form leads to several key advantages:
-
Faster approval times for medication access
-
Improved patient care coordination among healthcare providers
-
Assistance in advocating for specific treatments
This process aids prescribers by establishing documented justification for medication use in particular diagnoses, ensuring that patients receive the necessary medications without unnecessary obstacles.
Who Needs the Prior Authorization Form for Zoladex?
Understanding who must complete the Prior Authorization Form for Zoladex is essential for ensuring a smooth process. Key individuals involved include the prescribers who initiate the request and the patients who require the medication.
Eligibility for completing this form is determined based on specific diagnoses, primarily concerning conditions managed with Zoladex. The roles played by prescribers, such as physicians and oncologists, are vital in providing accurate information needed for the form.
Filling Out the Prior Authorization Form for Zoladex: Step-by-Step Guide
Filling out the Prior Authorization Form for Zoladex involves several detailed steps. This guide assists users in completing the form accurately, ensuring a smoother approval process.
-
Begin with patient identification information.
-
Provide prescriber details in the designated section.
-
Clearly state the diagnosis associated with the prescription.
-
Specify the intended use of Zoladex and include relevant clinical information.
Common errors to avoid include leaving fields blank or providing incomplete information, which can lead to delays or rejections of the authorization request.
Submission Methods for the Prior Authorization Form for Zoladex
Once the Prior Authorization Form for Zoladex is completed, there are various methods for submitting it. These submission options allow for flexibility in how healthcare providers can transmit the form to the appropriate insurance departments.
-
Fax the completed form directly to CVS Caremark.
-
Submit it online through insurance provider portals where applicable.
Be sure to follow up on the submission to confirm receipt and track processing timelines for the authorization request.
Confirmation and Tracking Your Submission of the Prior Authorization Form for Zoladex
After submitting the Prior Authorization Form for Zoladex, confirming its receipt is a critical step. Healthcare providers can typically call or use online tools to verify submission status. Tracking your application status helps in managing expectations regarding the approval process.
Keeping detailed records and confirmation details is vital, as this documentation can assist in any potential follow-up required.
Security and Compliance When Using the Prior Authorization Form for Zoladex
When handling the Prior Authorization Form for Zoladex, ensuring security and compliance with HIPAA guidelines is paramount. Proper handling of sensitive patient information is crucial in safeguarding privacy.
pdfFiller employs advanced security measures, such as 256-bit encryption, to protect user data while completing healthcare forms. Users are encouraged to adopt best practices to further secure patient information.
How pdfFiller Can Help With the Prior Authorization Form for Zoladex
pdfFiller simplifies the process of filling out the Prior Authorization Form for Zoladex. This cloud-based PDF editor offers features that enhance efficiency and ease of use, including the ability to edit, eSign, and securely share forms.
Utilizing pdfFiller's tools can streamline document management, ensuring compliance and accuracy throughout the authorization process.
Sample Prior Authorization Form for Zoladex
Providing a sample completed Prior Authorization Form for Zoladex helps users understand the correct format and required details. This illustrative example breaks down various sections, ensuring clarity when filling out your own form.
Referring to this sample can guide prescribers in maintaining accuracy and completeness in the authorization request.
Next Steps After Submitting the Prior Authorization Form for Zoladex
After submitting the Prior Authorization Form for Zoladex, users can expect several follow-up actions. Understanding the renewal or resubmission process is essential for ongoing treatments, especially for patients requiring long-term medication.
Encouraging the use of pdfFiller for future forms can help maintain organization and efficiency in managing healthcare documentation.
How to fill out the Zoladex Prior Authorization
-
1.Access the Prior Authorization Form for Zoladex on pdfFiller by searching for the form's name in the platform's search bar.
-
2.Once you locate the form, click on it to open the document in the pdfFiller interface.
-
3.Review the form layout to familiarize yourself with required fields and checkboxes, ensuring you understand where to enter information.
-
4.Before filling out the form, gather all necessary information such as patient details, prescribing physician's information, diagnosis, and intended use of Zoladex.
-
5.Start completing the patient information section by entering the patient's name, date of birth, and relevant identification numbers.
-
6.Move on to the prescriber's information by filling in the prescribing physician's name, address, and contact details, ensuring accuracy for approval.
-
7.Provide detailed information about the patient's diagnosis and current treatment status, using concise yet comprehensive descriptions.
-
8.Indicate the specific use of Zoladex, ensuring that you check relevant boxes and provide additional details as needed to justify the request.
-
9.Review all entered information carefully to ensure completeness and accuracy, paying attention to any missed fields or errors.
-
10.Once satisfied with the completed form, click on the save button to store your work, or use the download option to save a copy to your device.
-
11.If you need to submit the form, use the faxing feature on pdfFiller to send the completed form directly to CVS Caremark.
-
12.Consider printing a copy for your records before submitting to keep a reference of the information provided.

Who is eligible to use the Prior Authorization Form for Zoladex?
The form is primarily intended for healthcare providers who prescribe Zoladex for patients undergoing treatment for conditions like prostate or breast cancer and endometriosis.
What information is required to complete this form?
You will need to provide patient information, details about the prescribing physician, diagnosis specifics, and the intended use of Zoladex on the form.
How do I submit the Prior Authorization Form for Zoladex once completed?
After filling out the form, it must be faxed to CVS Caremark for review and approval. Ensure that all information is accurate before submission.
What common mistakes should I avoid when filling out this form?
Ensure that all required fields are completed accurately, double-check for any missing information, and verify that the physician's signature is included.
What is the typical processing time for the Prior Authorization request?
Processing times may vary, but it generally takes several days for CVS Caremark to review the submitted prior authorization form and respond.
Are there any fees associated with submitting the authorization form?
Typically, there are no fees directly associated with submitting the prior authorization form, but patients should confirm with their healthcare provider.
What should I do if my authorization request is denied?
If a prior authorization request is denied, contact the prescribing physician to discuss the next steps, which may include appealing the decision or considering alternative treatments.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.