Last updated on Apr 30, 2026

Get the free Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Auth Form
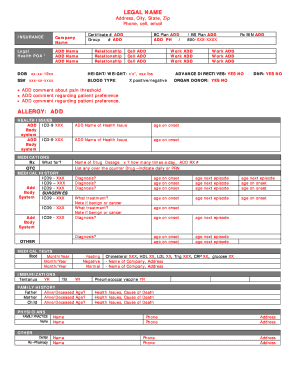
The Prior Authorization Form is a healthcare document used by providers to request approval for specific medical services or procedures from insurance plans.
pdfFiller scores top ratings on review platforms




Who needs Prior Auth Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Auth Form
What is the Prior Authorization Form?
The Prior Authorization Form is a crucial component in healthcare that allows providers to obtain approval for specific medical services or procedures. It is essential for healthcare practices to facilitate access to necessary treatments while ensuring compliance with insurance policies. This form typically contains important member information, including patient details, provider contact information, service type, and clinical indications.
The necessity of prior authorization arises from the need for insurance companies to validate the medical necessity of certain services. Without appropriate authorization, healthcare providers may face challenges in securing coverage for treatments, thus impacting patient care.
Purpose and Benefits of the Prior Authorization Form
This form plays a vital role in obtaining insurance approvals and presents numerous benefits for patients and healthcare providers alike. By using the prior authorization form, healthcare providers can streamline the process of securing necessary services, leading to improved workflows and timely access to medical treatments.
Additionally, the use of this form helps ensure compliance with insurance requirements, ultimately enhancing the quality of patient care. Understanding the purpose of the form can empower both professionals and patients in navigating the complexities of healthcare authorization.
Who Needs the Prior Authorization Form?
Typically, the need for a prior authorization form arises from several key stakeholders, including healthcare providers and patients. Various medical services, such as specialized treatments or referral consultations, often require this form for prior approval from insurance companies.
Healthcare professionals across disciplines must familiarize themselves with when prior authorization is necessary to ensure that patients receive timely and appropriate care. Understanding the parties involved in the authorization process can help facilitate better communication and a smoother experience.
How to Fill Out the Prior Authorization Form Online
Completing the prior authorization form online can be done efficiently with a guided approach. Follow these steps to access and fill out the form on the pdfFiller platform:
-
Access the pdfFiller website and navigate to the prior authorization form.
-
Fill in the required member information, including patient details and provider information.
-
Complete the service details section by accurately detailing the treatment or procedure requested.
-
Review the form for accuracy and completeness before submission.
Common pitfalls during form completion can include missing required fields or providing incorrect information. Attention to detail is essential in avoiding submission errors that may delay the approval process.
Required Documents and Supporting Materials
To ensure successful submission of the prior authorization form, certain documentation is typically required. This may include:
-
Patient information, including demographics and insurance details.
-
Clinical notes outlining the medical necessity for the requested service.
-
Any relevant test results or previous treatment records that support the request.
The accuracy and completeness of supporting materials significantly impact the approval process. It is advisable to gather and organize all required documents before filling out the form to streamline submission.
Submission Methods and Tracking Your Prior Authorization Form
Submitting the completed prior authorization form can be accomplished through various methods, ensuring convenience for users. The most common submission options include:
-
Submitting online through the pdfFiller platform.
-
Faxing the completed form directly to the insurance company.
-
Delivering the form in-person to the appropriate healthcare or insurance office.
Once submitted, users should confirm the submission and track processing status to manage follow-ups. Understanding typical processing times and procedures can help reduce anxiety during the wait for approval.
Common Rejection Reasons and Solutions
Users should be prepared for potential denial of prior authorization requests. Common reasons for rejection often stem from:
-
Insufficient information provided in the request.
-
Lack of medical necessity documentation.
-
Failure to adhere to insurance protocols or policy guidelines.
In case of rejection, it is important to understand how to respond effectively and amend submissions as needed. Implementing strategies to improve chances of approval on future requests involves thorough preparation and attention to detail.
Security and Privacy When Using the Prior Authorization Form
When filling out the prior authorization form, users can feel reassured regarding the secure handling of sensitive information. pdfFiller employs robust security measures, including encryption and HIPAA compliance, to protect user data during the form completion process.
The importance of maintaining privacy and confidentiality while handling healthcare forms online cannot be overstated. Ensuring your data remains secure is a priority for pdfFiller as it streamlines healthcare documentation processes.
How pdfFiller Can Simplify Your Prior Authorization Process
Using pdfFiller to manage your prior authorization forms can greatly enhance your experience. Key features that contribute to this simplification include:
-
Ease of editing and filling out forms directly in the platform.
-
The ability to eSign documents quickly, eliminating the need for physical signatures.
-
Organizational tools to keep all medical documents in one accessible location.
Many users have reported reduced stress and improved efficiency by taking advantage of pdfFiller’s features for prior authorization. The platform’s accessibility from any device further enhances user experience without the need for cumbersome downloads.
Getting Started with pdfFiller for Your Prior Authorization Needs
To begin utilizing pdfFiller for your prior authorization tasks, follow these simple instructions:
-
Create an account on pdfFiller’s website.
-
Explore available templates specifically designed for healthcare forms.
-
Take advantage of features that simplify the filling and submission process.
By integrating pdfFiller into your workflow, you can streamline your prior authorization requests, making it a beneficial tool for both healthcare professionals and patients alike.
How to fill out the Prior Auth Form
-
1.Access the Prior Authorization Form on pdfFiller by searching for 'Prior Authorization Form' in the template library.
-
2.Open the document to view all the available fillable fields and instructions.
-
3.Before starting, gather necessary information including member details, provider information, type of service requested, and clinical indications.
-
4.Use the cursor to navigate through the form fields. Click on each field to enter the required information.
-
5.Fill in member information, including name, date of birth, and insurance details in the designated sections.
-
6.Provide your healthcare provider's name, contact number, and NPI in the relevant fields.
-
7.Indicate the specific medical service or procedure requested and any essential clinical indications that support the request.
-
8.Once all fields are completed, carefully review the entered information for accuracy and completeness.
-
9.Utilize pdfFiller's built-in tools to correct any mistakes before finalizing the form.
-
10.After reviewing, save your progress to ensure your information is secure.
-
11.You can download the form as a PDF, or submit it directly through pdfFiller using the submission options available.

Who is eligible to use the Prior Authorization Form?
Typically, healthcare providers who need to obtain approval for specific medical services from insurance companies are eligible to use the Prior Authorization Form. Patients might also indirectly use it by having their providers fill it out.
What documents do I need to complete the form?
You will need to gather member details, provider information, the specific service requested, and any clinical indications or supporting documents that justify the request before filling out the Prior Authorization Form.
How do I submit the Prior Authorization Form once completed?
Upon completion, you can submit the Prior Authorization Form directly through pdfFiller or download it and send it to the relevant insurance company via email or postal service, as dictated by their submission guidelines.
Are there any common mistakes to avoid when filling out the form?
Common mistakes include missing required fields, incorrect member or provider information, and not including necessary supporting documents. It's crucial to double-check all entries before submission.
What is the processing time for a prior authorization request?
Processing times for prior authorizations vary by insurance companies, generally ranging from a few hours to several days. It's advisable to submit requests as early as possible to prevent delays in receiving medical services.
Is notarization required for the Prior Authorization Form?
No, the Prior Authorization Form typically does not require notarization. Ensure that all sections are filled out properly for validation during submission to the insurance.
What happens if my prior authorization request is denied?
If a prior authorization request is denied, healthcare providers usually receive a notification explaining the reasons. They can appeal the decision or provide additional documentation to support the request.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.