Last updated on May 2, 2015

Get the free GEHA Prior Authorization Criteria Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is GEHA PA Form
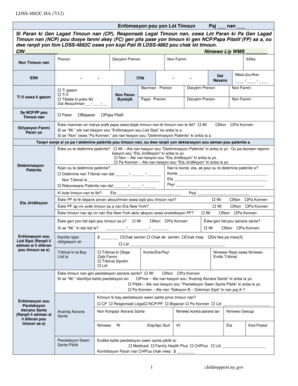
The GEHA Prior Authorization Criteria Form is a healthcare document used by prescribers to request prior authorization for diabetes test strips and kits.
pdfFiller scores top ratings on review platforms




Who needs GEHA PA Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to GEHA PA Form
What is the GEHA Prior Authorization Criteria Form?
The GEHA Prior Authorization Criteria Form is a vital document designed for healthcare providers to request prior authorization for diabetes test strips and kits. This form's primary purpose is to facilitate insurance reimbursement by collecting essential patient and physician details, prescribed drug information, and alternative product inquiries. A critical requirement of this form is the signature from the prescriber, ensuring that the information provided is accurate and legally binding.
Purpose and Benefits of the GEHA Prior Authorization Criteria Form
The GEHA Prior Authorization Criteria Form serves multiple crucial functions in the healthcare system. First, it aids in establishing medical necessity, which is essential for insurance claims to be processed smoothly. The form streamlines the prior authorization process, benefiting both patients and healthcare providers by reducing the time associated with paperwork and approval delays. Additionally, proper documentation through this form is vital for compliance with healthcare regulations, ensuring all parties adhere to required standards.
Who Needs the GEHA Prior Authorization Criteria Form?
This form is primarily utilized by prescribers, including physicians and nurse practitioners, who need to obtain prior authorization for their patients. Specific scenarios that necessitate the use of this form include prescriptions for diabetes test strips, which often require detailed approval to ensure coverage. Additionally, office staff may assist healthcare providers in completing and submitting this form as part of their administrative duties.
How to Fill Out the GEHA Prior Authorization Criteria Form Online (Step-by-Step)
To successfully complete the GEHA Prior Authorization Criteria Form online, follow these step-by-step instructions:
-
Access the form through the designated portal or website.
-
Fill out the patient and physician information sections fully and accurately.
-
Detail the prescribed drug and answer the medical necessity questions carefully, paying attention to specifics.
-
Ensure the prescriber’s signature is included in the required field.
-
Review all sections to ensure completeness before submission.
Special attention should be given to the medical necessity questions and signature fields to avoid processing delays.
Common Errors and How to Avoid Them
When completing the GEHA Prior Authorization Criteria Form, users often encounter several common errors, including:
-
Providing inaccurate patient or physician information.
-
Omitting required signatures or checklist items.
-
Failing to include alternative product inquiries when necessary.
Incorrect or incomplete submissions can lead to significant delays, so it is essential to carefully review the form before submission to ensure all information is accurate and complete.
How to Submit the GEHA Prior Authorization Criteria Form
The submission of the GEHA Prior Authorization Criteria Form can be accomplished through various methods, including online submission, fax, or traditional mail. After sending the form, it is imperative to confirm receipt to ensure the submission was successful. Be mindful of any relevant deadlines associated with the submission process, as timely submission is crucial for maintaining patient care continuity.
What Happens After You Submit the GEHA Prior Authorization Criteria Form?
Following the submission of the GEHA Prior Authorization Criteria Form, insurance providers will undertake several steps, including:
-
Reviewing the submitted information for accuracy and compliance with their guidelines.
-
Communicating the approval status back to the prescriber or designated office staff.
-
Providing a timeline for when patients can expect to hear about their prior authorization status.
Understanding these steps helps users manage expectations regarding timelines and follow-up actions.
Security and Compliance for the GEHA Prior Authorization Criteria Form
When handling sensitive patient information via the GEHA Prior Authorization Criteria Form, security and compliance are paramount. pdfFiller ensures secure editing, filling, and signing of PDFs, with adherence to HIPAA and GDPR regulations to protect patient data. It is vital to utilize secure document management practices within healthcare settings to maintain confidentiality and data integrity.
Utilizing pdfFiller to Optimize Your GEHA Prior Authorization Criteria Form Experience
To enhance the experience of completing the GEHA Prior Authorization Criteria Form, consider leveraging pdfFiller’s comprehensive features. The platform allows users to easily edit documents, eSign, and manage forms efficiently, significantly reducing administrative burdens. Embracing digital solutions, such as those offered by pdfFiller, can markedly improve the efficiency of healthcare operations and ensure a seamless form completion experience.
How to fill out the GEHA PA Form
-
1.Access the GEHA Prior Authorization Criteria Form on the pdfFiller platform by searching for its name in the search bar.
-
2.Once the form is open, familiarize yourself with the layout, including patient and physician information sections.
-
3.Gather necessary information such as patient identification, insurance details, and prescription specifics before starting the form.
-
4.Navigate to the patient information section and fill in the required fields accurately using pdfFiller's text editing features.
-
5.Proceed to complete the physician information and prescribed drug sections, ensuring all relevant details are included.
-
6.Use checkboxes provided for responses to alternative product questions, marking them carefully.
-
7.Review all filled fields for accuracy and completeness, utilizing pdfFiller's review features to check your entries.
-
8.Finalize your form by clicking the signature line to digitally sign, ensuring that you have the prescriber's consent.
-
9.Save your work frequently to avoid data loss, and when completed, utilize the 'Download' or 'Submit' function on pdfFiller to finalize the submission.

Who is eligible to use the GEHA Prior Authorization Criteria Form?
Eligible users include licensed healthcare providers who prescribe diabetes test strips and their patients needing these supplies for medical use.
What information do I need before completing the GEHA form?
Before starting the form, gather patient identification, insurance details, prescription specifics, and any other necessary medical information to ensure accuracy.
How do I submit the completed form?
After filling out and signing the form on pdfFiller, you can submit it electronically, or download it for manual submission to the insurance company.
What common mistakes should I avoid when filling out this form?
Avoid leaving sections blank, providing incorrect patient information, and forgetting to sign the form. Double-check for accuracy before submission.
How long does it take to process a prior authorization request?
Processing times vary, but typically it can take anywhere from a few days to a couple of weeks. It's best to check with the insurance provider for specific timelines.
Are there any fees associated with using the GEHA Prior Authorization Criteria Form?
Generally, there should not be any fees for submitting a prior authorization request. However, verify with your insurance provider for any potential costs.
What should I do if my authorization request is denied?
If your request is denied, you can contact your insurance provider for clarification on the decision and possible steps for appeal or resubmission.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.