Last updated on May 10, 2015
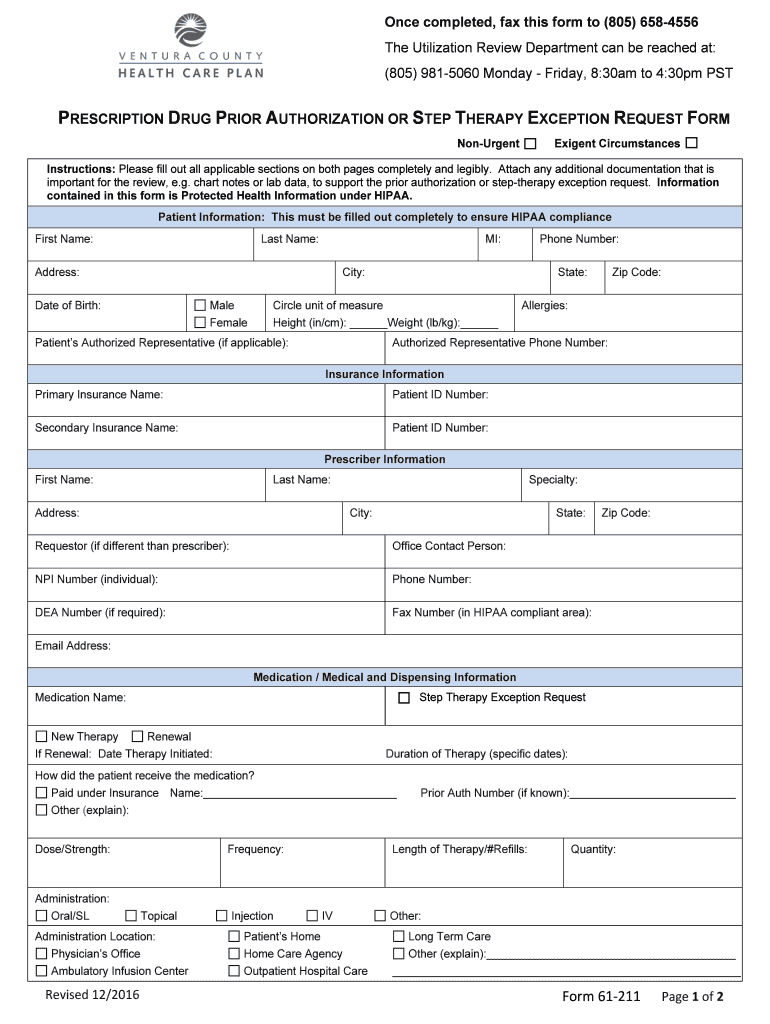
Get the free Prescription Drug Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Form
The Prescription Drug Prior Authorization Form is a healthcare document used by prescribers to request prior authorization or step therapy exceptions for prescription drugs.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Prescription Drug Prior Authorization Form?
The Prescription Drug Prior Authorization Form is a critical document used to request prior authorization for specific prescription medications. This form plays a vital role in the healthcare process by ensuring that necessary medications are covered by insurance plans before they are dispensed to patients.
Key components of the form include comprehensive patient information, detailed insurance details, and specific medication information. Each of these elements is essential for the assessment of coverage eligibility and to facilitate the treatment process.
Understanding the purpose of the Prescription Drug Prior Authorization Form can streamline access to necessary medications, thus enhancing patient care and satisfaction.
Purpose and Benefits of the Prescription Drug Prior Authorization Form
The Prescription Drug Prior Authorization Form serves several vital functions in the healthcare system. Primarily, it ensures that prescriptions for necessary medications receive coverage approval from insurance companies, benefiting both prescribers and patients.
This form helps navigate complex insurance requirements, which can significantly reduce out-of-pocket costs for patients. Furthermore, it plays an essential role in maintaining compliance with healthcare regulations, ensuring that prescribing practices are both legal and ethical.
-
Facilitates access to necessary medications
-
Reduces financial burden on patients
-
Ensures compliance with healthcare regulations
Who Needs the Prescription Drug Prior Authorization Form?
Typically, the Prescription Drug Prior Authorization Form is completed by prescribers who are responsible for initiating treatment plans. They play a crucial role in gathering the necessary information to fill out this form correctly.
Certain patients may require this form based on their individualized treatment plans and the specific medications prescribed. It is crucial that the prescriber has accurate and complete information to enhance the chances of a successful authorization.
-
Prescribers initiating medication requests
-
Patients with specific treatment plans needing certain medications
-
Healthcare providers facilitating the process
Eligibility Criteria for the Prescription Drug Prior Authorization Form
Successful submission of the Prescription Drug Prior Authorization Form requires that specific eligibility criteria are met. These criteria often include requirements associated with different insurance plans and the medications being requested.
Conditions that might warrant a step therapy exception request also need to be considered. It is essential to understand the specific guidelines set by the insurance provider to avoid complications with the submission process.
-
Verification of insurance-related requirements
-
Assessment of medical necessity for medications
-
Understanding the insurance provider’s specific guidelines
How to Fill Out the Prescription Drug Prior Authorization Form Online (Step-by-Step)
Completing the Prescription Drug Prior Authorization Form online involves several steps to ensure accuracy and compliance. Follow these instructions for a successful submission:
-
Begin with filling out the patient information section, including full name and date of birth.
-
Provide detailed insurance details, ensuring accurate policy numbers and coverage information.
-
Complete the medication section, specifying dosage and frequency as prescribed.
-
Input necessary clinical information to support the request for authorization.
-
Review all entries for accuracy before submission to avoid common errors.
Taking the time to double-check your form can help prevent issues that may delay medication access.
Submission Methods and Delivery for the Prescription Drug Prior Authorization Form
Once the Prescription Drug Prior Authorization Form is completed, it must be submitted following the designated methods. One common method is to fax the completed form to the Utilization Review Department of the insurance company.
Confidentiality is paramount when transmitting sensitive information, so using secure methods to send the form is essential. Additionally, tracking the submission status is crucial to confirm receipt and processing.
-
Options for submitting the form include faxing or electronic submission.
-
Implement secure methods to maintain confidentiality.
-
Follow up on submission to track approval status.
Common Rejection Reasons and Solutions
Understanding potential reasons for rejection of authorization requests can help streamline the process. Common pitfalls include incomplete information, lack of medical necessity, or deviation from prescribing guidelines.
If the form is rejected, it is vital to know how to amend and resubmit effectively. Familiarizing oneself with the insurance policy requirements can significantly reduce the likelihood of future rejections.
-
Ensure all sections are completely filled out to avoid incomplete submissions.
-
Verify that all medical necessity criteria are well-documented.
-
Consult with the insurance provider for specific rejection reasons and steps to reapply.
Security and Compliance for Handling the Prescription Drug Prior Authorization Form
When handling the Prescription Drug Prior Authorization Form, the importance of document security and compliance cannot be overstated. Ensuring the protection of sensitive data is a priority, with platforms like pdfFiller employing measures such as 256-bit encryption.
Compliance with regulations like HIPAA and GDPR safeguards patient data privacy and promotes responsible handling of sensitive forms. Users are encouraged to utilize secure platforms for filling and submitting these important documents.
-
Utilize platforms with strong encryption measures for enhanced security.
-
Ensure compliance with HIPAA and GDPR regulations.
-
Be mindful of privacy when handling sensitive medical information.
Utilizing pdfFiller to Streamline Your Prescription Drug Prior Authorization Process
Leveraging pdfFiller can significantly simplify the process of completing the Prescription Drug Prior Authorization Form. With features designed for ease of use, including eSigning and form editing, it enhances accessibility and convenience.
The cloud-based platform allows users to manage documents from anywhere, all while ensuring robust security safeguards are in place. By adopting pdfFiller, users can focus on completing submissions without the hassle of complicated procedures.
-
eSigning capabilities streamline the authorization process.
-
Cloud access ensures convenience from any location.
-
Security measures protect sensitive information throughout the process.
How to fill out the Prior Authorization Form
-
1.Access pdfFiller and log into your account. If you don't have one, create a new account to get started.
-
2.In the search bar, type 'Prescription Drug Prior Authorization Form' to quickly locate the form.
-
3.Open the form by clicking on it. You will see the form displayed in the editing interface of pdfFiller.
-
4.Gather all necessary information before filling out the form, including patient details, insurance information, and medication specifics.
-
5.Begin filling in the patient information section accurately, ensuring the name, date of birth, and insurance ID are correct.
-
6.Next, move to the insurance details area and provide necessary information such as the insurance provider's name and policy number.
-
7.Fill in the medication details section with accurate drug names, dosages, and prescribing instructions.
-
8.Provide relevant clinical information that supports your authorization request, adhering to all sections needing detailed responses.
-
9.Use the checkboxes and dropdowns carefully as instructed, making sure you're completing all applicable sections.
-
10.Once all fields are filled, review the document for accuracy and completeness to prevent any processing delays.
-
11.Make use of the 'Preview' function to see how the finished form will appear.
-
12.After confirming all information is correct, you can save the document or download it for submission.
-
13.Submit the completed form via fax according to the instructions provided, preferably to the Utilization Review Department.

Who needs to fill out the Prescription Drug Prior Authorization Form?
The Prescription Drug Prior Authorization Form is primarily filled out by prescribers, such as doctors or nurse practitioners, who are requesting drug authorizations for their patients.
What information do I need to complete the form?
You will need patient information, insurance details, and specific medication information, including dosage and prescribing instructions, to properly complete the form.
How do I submit the completed form?
The form should be faxed to the Utilization Review Department as per the submission guidelines specified in the form.
What are common mistakes to avoid when filling out this form?
Ensure that all sections are filled out completely. Double-check patient details, and avoid leaving any required fields blank to prevent delays in the authorization process.
Are there any deadlines for submitting the form?
While specific deadlines may vary, it is advisable to submit the Prescription Drug Prior Authorization Form as early as possible to ensure timely processing and avoid disruptions in patient medication.
What happens if my request is denied?
If your prior authorization request is denied, you will typically receive notice from the insurance company detailing the reason for denial and possible next steps for appealing the decision.
What supporting documents do I need to include?
Along with the form, be prepared to submit any required clinical information or other documentation that supports the need for the medication to ensure a successful authorization request.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.






















