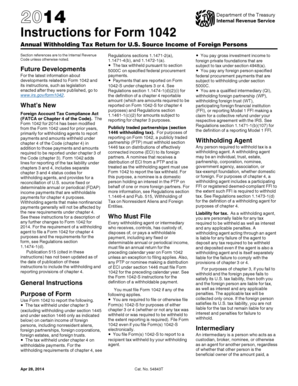Last updated on May 18, 2015

Get the free Request for Prior Authorization
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Request
The Request for Prior Authorization is a healthcare document used by providers to obtain approval for medical services before they are delivered.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Request?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Request
What is the Request for Prior Authorization?
The Request for Prior Authorization form is a critical document used in healthcare to seek approval for services before they are provided. This form plays a crucial role in the continuum of care, ensuring that necessary medical services are pre-approved by insurance providers. By facilitating utilization management reviews, it helps streamline the approval process, thereby maintaining the quality and efficiency of healthcare delivery.
Healthcare prior authorization is essential as it protects providers and patients by verifying coverage ahead of time. Accurate completion of this form minimizes misunderstandings regarding service eligibility, improving the chance of securing necessary treatments.
Why is the Request for Prior Authorization Important?
The significance of the Request for Prior Authorization cannot be overstated. This form benefits healthcare providers by ensuring that services align with insurance requirements, reducing the risk of denied claims. Additionally, it safeguards patients from unexpected out-of-pocket expenses, fostering transparency in healthcare delivery.
Failing to obtain prior authorization may lead to severe consequences, including delayed treatments, escalating healthcare costs, and administrative challenges. Through effective cost management and insurance approval processes, healthcare providers can enhance patient care while remaining compliant with regulatory standards.
Key Features of the Request for Prior Authorization Form
-
The form includes vital fillable fields, such as Member ID and Date of Birth, ensuring accurate identification of patients.
-
It requires a physician's signature to validate the request and confirm understanding of the needed services.
-
Instructions highlight the importance of filling only designated areas, which helps prevent errors during submission.
Who Needs the Request for Prior Authorization?
This form is essential for various stakeholders involved in the healthcare process. Requesting physicians utilize it to obtain necessary approvals for their patients' treatments. Patients requiring specific services, such as specialized procedures or medications, must also engage with this form to ensure their needs are met.
Additionally, certain healthcare situations often necessitate prior authorization, reinforcing the need for this document in numerous clinical contexts.
How to Fill Out the Request for Prior Authorization Online
Filling out the Request for Prior Authorization online simplifies the process significantly. Begin by gathering essential information before starting, which includes patient details, service information, and required authorization codes.
-
Access the online form through a reliable platform.
-
Input the Member ID and Date of Birth in the designated fields.
-
Fill in all required sections thoroughly, ensuring no areas are left blank.
-
Review the information entered for accuracy.
-
Submit the form electronically or follow the subsequent steps for other submission methods.
Submission Process for the Request for Prior Authorization
After completing the Request for Prior Authorization form, various submission methods are available. Users can choose to fax the document, upload it online, or even submit it via mail, depending on the requirements of the insurance provider.
It's important to be aware of specific details related to submission, including any applicable fees, deadlines, and estimated processing times. Ensuring adherence to these guidelines can facilitate smoother approval outcomes.
Common Errors When Submitting the Request for Prior Authorization
-
Incomplete fields can lead to delays; always double-check all information before submitting.
-
Missing physician signatures invalidates the request, so ensure all signatures are included.
-
Using outdated or incorrect procedure codes can result in denials; confirm accuracy prior to submission.
Tracking and Confirming Your Submission
After submitting the Request for Prior Authorization, tracking its status is vital. Utilize online patient portals or contact the insurance provider to confirm that the submission was received.
If a request is denied, it’s crucial to understand the reasons and gather any additional information needed to address concerns raised by the insurance company.
How pdfFiller Can Help with the Request for Prior Authorization
pdfFiller offers several features that enhance the process of completing the Request for Prior Authorization. Users can edit forms, sign electronically, and secure sensitive information through robust security measures, including 256-bit encryption.
The platform also streamlines the prior authorization process, making it easier for users to manage and submit their requests successfully.
Get Started with Your Request for Prior Authorization Today!
Utilizing pdfFiller simplifies form completion, ensuring a user-friendly experience. The platform offers compliance assurances for handling sensitive documents, which is particularly important in healthcare contexts.
How to fill out the Prior Authorization Request
-
1.Access the Request for Prior Authorization form on pdfFiller by searching for the document or uploading it from your files.
-
2.Once opened, review the sections on the form that need to be filled, which include patient and provider information.
-
3.Before starting, gather essential information such as the Member ID, Date of Birth, NPI, and Tax ID to fill out the form accurately.
-
4.In the designated fields, begin entering the required data, ensuring that you adhere to the instruction, ‘Please write only in designated areas.’
-
5.Use pdfFiller’s tools to navigate between fields easily, making sure to fill in all mandatory fields for completeness.
-
6.When you have completed filling all fields, review the information carefully to confirm the accuracy and completeness of the details provided.
-
7.After reviewing, click the save or download button to retain a copy of the completed form for your records or submission.
-
8.Finally, use the submission features on pdfFiller to send your completed Request for Prior Authorization directly where required.

Who is eligible to submit the Request for Prior Authorization?
The Request for Prior Authorization form can be submitted by healthcare providers, specifically physicians, who are requesting approval for medical services on behalf of their patients.
What is the typical processing time for approval?
Processing times for prior authorizations can vary, but typically it takes several days. It’s advisable to submit the request as early as possible to avoid delays in treatment.
What supporting documents are needed when submitting this form?
Supporting documents often include medical records, treatment plans, and any previous authorizations related to the requested services. Check with the insurance provider for specific requirements.
Can patients submit the Request for Prior Authorization directly?
Generally, patients should ask their healthcare providers to submit the Request for Prior Authorization on their behalf, as the physician's signature is required.
What common mistakes should I avoid when filling out this form?
Common mistakes include leaving mandatory fields blank, providing incorrect patient details, and forgetting to sign the form. Ensure all required information is accurate and complete before submission.
When is the best time to submit the Request for Prior Authorization?
It’s best to submit the Request for Prior Authorization as soon as possible, ideally before scheduling the needed medical service or treatment, to allow sufficient time for processing.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.