Last updated on May 26, 2015
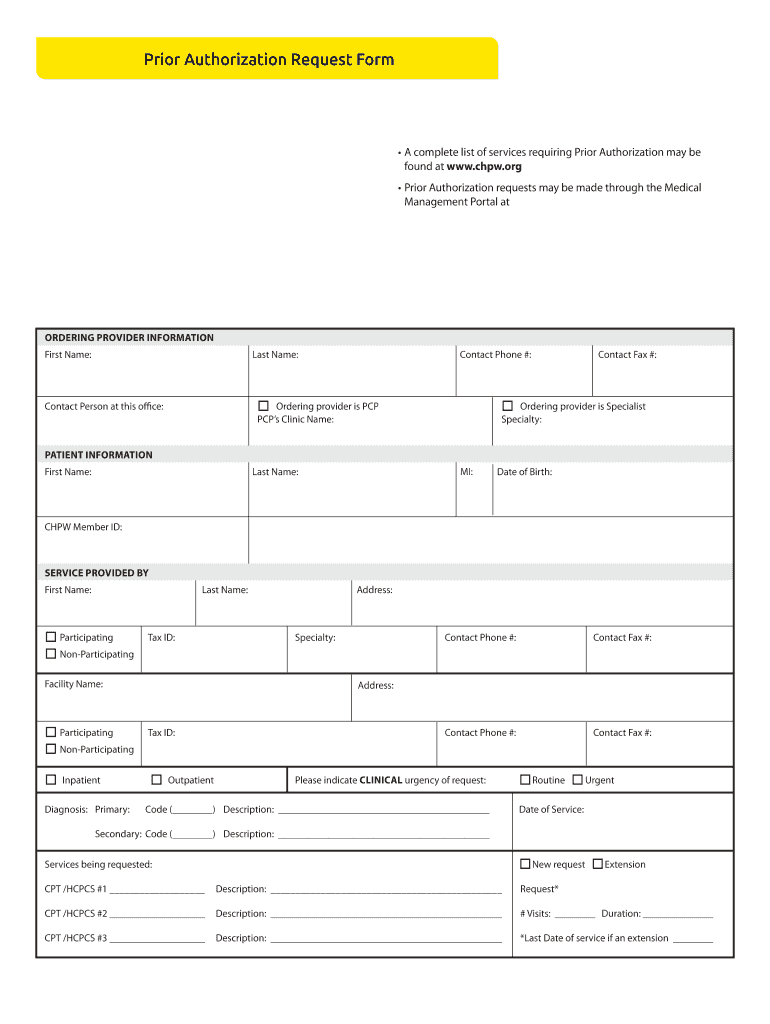
Get the free Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Form
The Prior Authorization Request Form is a medical document used by healthcare providers to request prior authorization for services from CHPW for Medicare Advantage plan members.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Prior Authorization Request Form?
The Prior Authorization Request Form is a critical document used by healthcare providers to obtain necessary approvals for medical services. This form is essential for streamlining the authorization process within the healthcare system, ensuring proper communication between providers and insurers. Its significance extends to both patients and healthcare providers, as it can impact treatment timelines and patient access to care.
For providers, correctly using the prior authorization request form enhances efficiency in managing care for their patients, especially within plans like Medicare Advantage. By submitting this healthcare prior authorization form, providers help prevent delays in treatment and ensure their patients receive timely services.
Purpose and Benefits of the Prior Authorization Request Form
The primary purpose of the prior authorization request form is to secure authorization for medical services before they are provided. This ensures that the proposed services are necessary and covered by the patient's insurance plan. Both healthcare providers and Medicare Advantage members can experience significant advantages through its use.
-
Facilitates timely approvals, which can accelerate access to needed care.
-
Reduces the likelihood of claim denials, ensuring financial clarity for both providers and patients.
-
Enhances communication between all parties involved in the patient's care.
By utilizing the Medicare Advantage prior authorization, providers can navigate the complexities of patient care more efficiently.
Who Needs the Prior Authorization Request Form?
This form is predominantly required for healthcare providers seeking authorization on behalf of their patients. It is essential for those working within systems that necessitate prior approval for specific tests, treatments, or medications.
Common scenarios in which the prior authorization request form is needed include:
-
When a provider plans to prescribe a costly medication.
-
Before conducting specialized tests or procedures requiring authorization.
-
In cases where non-emergency services are sought under insurance plans.
How to Fill Out the Prior Authorization Request Form Online (Step-by-Step)
Filling out the prior authorization request form online is a straightforward process that can be accomplished with a few key steps. Follow this step-by-step guide to ensure thorough completion:
-
Open the form in a compatible online PDF editor.
-
Enter the patient's First Name and Last Name.
-
Provide the necessary Contact Phone # and CHPW Member ID.
-
Specify the Diagnosis and relevant CPT /HCPCS #1 codes.
-
Attach any required supporting clinical documentation.
-
Review all information for accuracy and completeness before submission.
Information You'll Need to Gather for the Form
Before beginning to fill out the prior authorization request form, it's crucial to gather all necessary information to avoid delays. This includes specific patient and provider details that are essential for completing the form.
-
Patient demographics, including name, contact information, and insurance details.
-
Provider information, such as name, contact information, and NPI number.
-
Diagnosis codes and details about the proposed medical services.
Moreover, ensure that you have all supporting clinical documentation ready, as this is vital to substantiate the request.
Common Errors and How to Avoid Them
While filling out the prior authorization request form, several common errors can occur that may delay processing. Being aware of these can help in avoiding them.
-
Inaccurate or incomplete patient and provider information.
-
Failure to attach required clinical documentation.
-
Missing signatures, if necessary, on the form.
To minimize these errors, thoroughly review the finished form before submission. Ensure that each field is adequately filled out and that all documentation is attached correctly.
Submission Methods and Delivery for the Prior Authorization Request Form
Once the prior authorization request form is completed, it's essential to know the various methods for submission. Several channels exist to deliver the form efficiently.
-
Fax directly to the relevant insurance provider.
-
Send via traditional mail to the specified address.
-
Use online submission options, if available.
It's also important to track submissions, as this can provide confirmation and peace of mind regarding the status of the authorization request.
What Happens After You Submit the Prior Authorization Request Form?
After submitting the prior authorization request form, it enters a review process by the insurance provider. Understanding what happens next can alleviate concerns over timelines and approval.
-
The insurance company will assess the request based on coverage criteria.
-
They will communicate the decision within a predetermined timeline, usually within a few days to weeks.
-
Patients and providers can check prior authorization request status through the insurance company’s customer service or online portal.
Security and Compliance for the Prior Authorization Request Form
When handling sensitive information through the prior authorization request form, security and compliance are paramount. The form incorporates robust security measures to protect user data.
-
Utilization of 256-bit encryption for data protection during transfer.
-
Compliance with HIPAA and GDPR regulations to ensure patient privacy.
-
Regular audits to maintain the integrity of security protocols.
These measures provide assurance that personal and medical information is handled with the utmost care and security.
Why Choose pdfFiller for Your Prior Authorization Request Form?
pdfFiller offers a range of features that enhance the process involved with the prior authorization request form. With an easy-to-use interface, users can efficiently edit, fill, and submit their forms online.
-
Ability to create fillable forms and edit text/images easily.
-
Integration of e-signature capabilities for seamless submissions.
-
A cloud-based system that promotes easy access from anywhere.
With over 100 million users benefiting from these capabilities, pdfFiller stands out as a preferred solution for managing forms like the prior authorization request effectively.
How to fill out the Prior Authorization Form
-
1.To begin, access pdfFiller and search for the Prior Authorization Request Form using the search bar.
-
2.Open the form, which will load into the pdfFiller interface.
-
3.Before completing the form, gather essential information including patient details, provider information, required diagnosis codes, and service specifics.
-
4.Start filling in the form by clicking on the designated fields using the cursor. You will see that each field is interactive.
-
5.Enter patient information such as 'First Name', 'Last Name', and 'Contact Phone #'.
-
6.Fill in the 'CHPW Member ID' field accurately to avoid processing delays.
-
7.Provide detailed information about the diagnosis and the necessary treatment services. Enter the applicable CPT/HCPCS codes for the requested services.
-
8.Attach supporting clinical documentation by navigating to the attachments section of pdfFiller, following the interface prompts.
-
9.Ensure all required fields are completed to avoid incomplete submissions that can lead to processing delays.
-
10.Once all data is entered, review the entire form for accuracy to confirm all information is correct and attached documents are included.
-
11.Finalizing the form is crucial; double-check each entry carefully.
-
12.To save, click the 'Save' icon. You can download the finalized form or submit directly through pdfFiller's interface, based on your submission preference.

What are the eligibility requirements for submitting this form?
To submit the Prior Authorization Request Form, the patient must be enrolled in a CHPW Medicare Advantage plan, and the requested services must be covered by their plan. Verify all patient details carefully to ensure eligibility.
Are there any deadlines for submitting this prior authorization request?
While specific deadlines may vary, it’s crucial to submit the Prior Authorization Request Form as soon as possible before the scheduled medical service to allow adequate processing time.
How do I submit the Prior Authorization Request Form?
The form can be submitted electronically through pdfFiller or faxed directly to CHPW. Ensure that all required fields are completed, and attached documents are included before submission.
What supporting documents do I need to attach?
Supporting clinical documentation should include medical records, treatment plans, and any relevant test results that substantiate the need for the requested services. Ensure all documents are legible and clearly labeled.
What are common mistakes to avoid when filling out this form?
Common mistakes include leaving fields blank, submitting without attaching required documentation, and providing inaccurate patient or provider information. Double-check all entries before finalizing.
What is the processing time for a prior authorization request?
Processing times can vary, but generally, you should allow at least several business days for the request to be reviewed. Delays may occur if forms are incomplete or require additional documentation.
Is there a fee associated with submitting this form?
Typically, requesting prior authorization does not incur a fee for the provider or patient, but it's advisable to check with your specific insurance policy to confirm.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.






















