Last updated on Mar 12, 2015
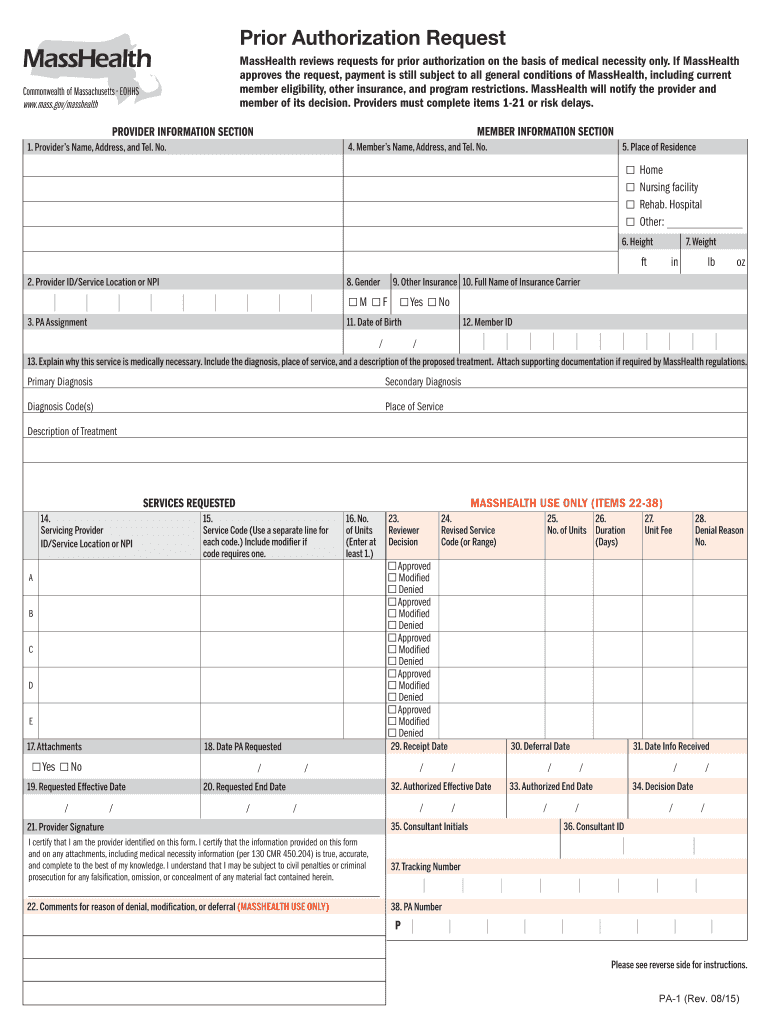

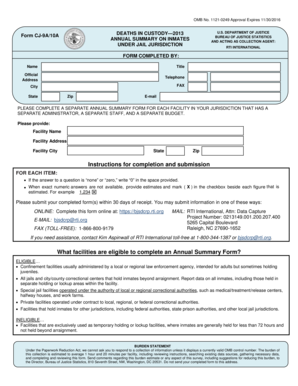
Get the free MassHealth Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is MassHealth PA Form
The MassHealth Prior Authorization Request Form is a medical authorization document used by healthcare providers in Massachusetts to obtain prior approval for medical services from MassHealth.
pdfFiller scores top ratings on review platforms




Who needs MassHealth PA Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to MassHealth PA Form
What is the MassHealth Prior Authorization Request Form?
The MassHealth Prior Authorization Request Form (PA-1) is a critical document utilized by healthcare providers in Massachusetts to obtain prior authorization for various medical services. This form not only facilitates efficient communication between providers and the MassHealth program but is also integral for ensuring compliance with local healthcare regulations.
Understanding the purpose of the form is vital, as it reinforces the framework of medical oversight within the state. It highlights the legal and regulatory importance of documentation in healthcare practices, ensuring that both providers and patients are aligned on treatment decisions.
Purpose and Benefits of Using the MassHealth Prior Authorization Request Form
Utilizing the MassHealth Prior Authorization Request Form streamlines the process of accessing necessary medical services, ensuring that patients receive timely care. This form plays a significant role in helping providers maintain meticulous documentation, which is essential for patient care and for reducing liability risks.
Moreover, MassHealth relies on the details provided in the form to make informed coverage decisions. Properly filled-out forms can enhance the speed of processing authorizations while protecting the rights of both providers and patients.
Who Needs the MassHealth Prior Authorization Request Form?
The MassHealth Prior Authorization Request Form must be completed by a variety of healthcare providers, including physicians, specialists, and medical facilities that seek authorization for specific services. It's essential for these providers to understand their responsibility in submitting this form to comply with MassHealth requirements.
In addition, patient members who require certain treatments may be affected by the authorization requirements that necessitate the use of this form. Organizations involved in patient care should also be familiar with the submission process to comply effectively with MassHealth protocols.
Eligibility Criteria and Submission Timeline for the MassHealth Prior Authorization Request Form
To qualify for services covered under MassHealth, patients must meet specific eligibility criteria, which are detailed on the form. Understanding when to submit the MassHealth Prior Authorization Request Form is crucial; timely submission can influence the approval process significantly.
Failing to submit the form within the designated timeline can result in denial of authorization, which emphasizes the importance of adhering to these regulatory timelines. Providers should familiarize themselves with these deadlines to avoid complications in patient care.
How to Fill Out the MassHealth Prior Authorization Request Form Online
Filling out the MassHealth Prior Authorization Request Form requires careful attention to detail. The form consists of several sections, labeled from items 1 to 21, that gather essential information regarding the provider, patient, and services requested.
Each section will require specific details—accurate filling of both provider and member information is critical for a successful submission. Additionally, providers should be cautious to avoid common errors, such as misplacing signatures or omitting required fields.
Required Documents and Supporting Materials for Submission
When submitting the MassHealth Prior Authorization Request Form, certain supporting documents are typically required to strengthen the authorization request. These documents may include previous medical records, diagnostic reports, and letters of medical necessity.
Organizing these materials effectively is integral; providers should ensure that all supporting documents are attached and in compliance with MassHealth documentation standards to facilitate a smoother approval process.
How to Submit the MassHealth Prior Authorization Request Form
Healthcare providers can submit the MassHealth Prior Authorization Request Form via various methods including online, by mail, or via fax. Adhering to the submission deadlines is essential to ensure timely processing of authorization requests.
After submission, providers should track their requests to verify the status and receive confirmation of filing. Understanding these processes can help mitigate delays in patient care.
Security and Compliance Considerations for the MassHealth Prior Authorization Request Form
Data security is paramount when dealing with the MassHealth Prior Authorization Request Form, given the sensitive information it contains. Adhering to HIPAA regulations and data protection standards is essential for healthcare providers to maintain patient confidentiality.
Moreover, leveraging secure platforms, such as pdfFiller, enhances document security and ensures compliance throughout the form submission process, allowing providers to manage sensitive information with confidence.
Enhance Your Experience with pdfFiller for the MassHealth Prior Authorization Request Form
By utilizing pdfFiller, healthcare providers can simplify the process of filling out, editing, and eSigning the MassHealth Prior Authorization Request Form. This platform offers numerous benefits, including ease of use and cloud-based management for enhanced security.
Providers can also rest assured knowing that pdfFiller is designed to support the completion of vital forms while maintaining robust security features, making it a reliable choice for managing sensitive documentation efficiently.
How to fill out the MassHealth PA Form
-
1.Access the MassHealth Prior Authorization Request Form on pdfFiller by navigating to the provided link or searching for the form in the pdfFiller interface.
-
2.Once opened, familiarize yourself with the form layout which contains various fillable fields and checkboxes to complete.
-
3.Before filling out the form, gather necessary documents such as medical necessity reports, diagnosis codes, and treatment descriptions to ensure accurate information.
-
4.Start by entering the provider's information in the designated fields at the top of the form. Make sure name, address, and contact details are accurate.
-
5.Proceed to fill in the member’s information section with the correct patient details including name, date of birth, and MassHealth ID number.
-
6.For the services requested section, clearly specify the requested medical services, including relevant codes and descriptions to justify the request.
-
7.As you fill out the form, refer to the instructions provided within the document to ensure all items from 1-21 are completed as required.
-
8.Once all fields are filled, review the completed form thoroughly for accuracy and completeness. Ensure that there are no missing or incorrect entries.
-
9.Finalize the form by obtaining your signature in the appropriate section, confirming that all information is correct and that you are authorized to submit this request.
-
10.After signing, save the completed form in your pdfFiller account, download it for your records, or submit the form directly via the platform according to specified submission guidelines.

Who is eligible to use the MassHealth Prior Authorization Request Form?
The form is specifically for healthcare providers in Massachusetts who are seeking prior authorization for medical services from MassHealth on behalf of their patients.
What is the deadline for submitting the authorization request?
While specific deadlines can vary based on services, it is advisable to submit the MassHealth Prior Authorization Request Form as soon as the service is planned to avoid delays in approval.
How should I submit the completed form?
You can submit the completed MassHealth Prior Authorization Request Form electronically through pdfFiller or print and mail it to the designated MassHealth office, following the submission instructions provided.
What supporting documents are required with the form?
Typically, supporting documents such as medical necessity statements, relevant treatment plans, and diagnosis codes must accompany the MassHealth Prior Authorization Request Form for proper review.
What common mistakes should I avoid while filling out the form?
Ensure all required fields are filled accurately, particularly the provider and member information, and avoid common errors such as submitting without a signature or missing supporting documents.
How long does it take to process the authorization request?
Processing times can vary, but applicants can generally expect a response from MassHealth within a few weeks depending on the completeness of the request and current processing loads.
What should I do if my request is denied?
If your request for prior authorization is denied, review the denial letter for reasons, consult with a billing specialist, and consider appealing the decision according to the guidelines provided by MassHealth.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.