Last updated on Jul 6, 2015

Get the free Direct Member Reimbursement Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Reimbursement Form
The Direct Member Reimbursement Form is a healthcare document used by members to request reimbursement for prescriptions purchased without their PBM Plus card.
pdfFiller scores top ratings on review platforms




Who needs Reimbursement Form?
Explore how professionals across industries use pdfFiller.
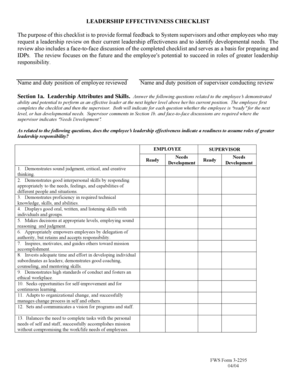
Comprehensive Guide to Reimbursement Form
What is the Direct Member Reimbursement Form?
The Direct Member Reimbursement Form is essential for healthcare plan members seeking to request reimbursement for prescriptions purchased without using their PBM Plus card. This form serves as a formal request, enabling members to recover treatment costs efficiently.
By utilizing this submission, members ensure that they can reclaim expenses for their prescriptions, especially in scenarios where the PBM Plus card was unavailable during the purchase. It acts as a crucial resource for those managing their healthcare expenses.
Purpose and Benefits of the Direct Member Reimbursement Form
The Direct Member Reimbursement Form offers numerous advantages that streamline the reimbursement process. This includes fast reimbursement for eligible prescriptions, allowing members to quickly address their financial needs.
Moreover, the use of this form can significantly facilitate a smoother claims process. With clear guidelines on how to submit claims, members can avoid common pitfalls that might delay their reimbursements.
Who Needs the Direct Member Reimbursement Form?
The form is primarily intended for healthcare plan members and their designated legal representatives. Cardholders who have incurred expenses for prescription costs but did not use their PBM Plus card are typically the ones who need to complete this documentation.
It is important to highlight that legal representatives may also fill out the form on behalf of a cardholder, ensuring claims can be processed accurately for those who may require assistance.
How to Fill Out the Direct Member Reimbursement Form Online (Step-by-Step)
Follow these steps to complete the Direct Member Reimbursement Form electronically using pdfFiller:
-
Access the form through pdfFiller’s platform.
-
Enter your Cardholder ID, Cardholder Name, and Patient Name in the appropriate fields.
-
Attach necessary receipts to substantiate your claim.
-
Review all entered information for accuracy.
-
Complete the signature section by the cardholder or legal representative.
-
Submit the form for processing.
Ensuring accurate completion of fields such as Date of Birth is crucial to prevent submission delays.
Common Errors and How to Avoid Them
When filling out the Direct Member Reimbursement Form, users often make a few common errors that can jeopardize their reimbursement. These include:
-
Missing required fields, which can lead to processing delays.
-
Incorrect information, making it difficult for claims to be approved.
To boost approval chances, implement a thorough review process prior to submission. Double-check all entries and ensure all supporting documents are included.
Submission Methods and Delivery for the Direct Member Reimbursement Form
Once the form is completed, users have multiple submission methods available. These include electronic submission via pdfFiller or physical mailing options, providing flexibility based on user preferences.
Tracking submission status is vital, as it allows members to follow up on processing times and ensure their reimbursement is being handled appropriately. Being aware of expected timelines can enhance user experience.
What Happens After You Submit the Direct Member Reimbursement Form?
After submitting the Direct Member Reimbursement Form, members can anticipate receiving confirmation notifications. Typically, members are informed about processing timelines, allowing them to plan accordingly.
In cases where additional information is needed to process the claim, members should be prepared to respond promptly to avoid delays in their reimbursements.
Security and Compliance for Handling Your Reimbursement Information
Users can rest assured that their data is handled with utmost care. The Direct Member Reimbursement Form adheres to security measures aligned with HIPAA and GDPR compliance, ensuring privacy is a top priority.
PdfFiller implements advanced data encryption protocols to protect sensitive reimbursement information throughout the entire process.
Discover How pdfFiller Streamlines the Direct Member Reimbursement Process
PdfFiller enhances the Direct Member Reimbursement Form experience with a suite of features designed to simplify document management. Key capabilities include eSigning, form completion, and secure document storage, making the entire process user-friendly.
In addition, pdfFiller provides editing capabilities and tutorials that can guide users through the form-filling process, ensuring a seamless experience from start to finish.
Sample or Example of a Completed Direct Member Reimbursement Form
For reference, users can access a sample of a completed Direct Member Reimbursement Form. This example illustrates how to fill out various fields, ensuring clarity in the submission process.
By following the sample closely, members can increase accuracy when filling out their own forms, reducing the likelihood of errors that can occur during the process.
How to fill out the Reimbursement Form
-
1.To begin, access the Direct Member Reimbursement Form on pdfFiller by visiting the platform and using the search bar to locate the specific form.
-
2.Once you open the form, familiarize yourself with its fields and layout. Look for designated areas such as 'Cardholder ID No:', 'Cardholder Name:', and 'Patient Name.'
-
3.Before filling out the form, gather necessary information including the cardholder's identification details, patient details, prescription receipts, and any other required documentation.
-
4.As you complete the fields, click to enter information in each blank. Use pdfFiller's tools to navigate smoothly between sections.
-
5.Be sure to verify that all the information entered is accurate. Check for spelling mistakes or missing details that may delay processing.
-
6.Once the form is filled out completely, take a moment to review it. Confirm that all signatures are provided where necessary, especially from the cardholder or legal representative.
-
7.After reviewing, save your progress and choose the 'Download' option if you prefer a saved copy, or go directly to the submission process on pdfFiller.

Who is eligible to use the Direct Member Reimbursement Form?
The form is designed for members of a healthcare plan who have incurred out-of-pocket expenses for prescriptions and wish to seek reimbursement from their insurance provider.
Are there specific deadlines for submitting this form?
While the metadata does not specify deadlines, it is typical for reimbursement forms to have submission deadlines aligned with your insurance policy. Check with your provider for specific timelines.
What documents are required when submitting this form?
You will need to include receipts for the prescriptions purchased, along with any applicable patient and cardholder information. Ensure all supporting documents are attached to avoid processing delays.
How do I submit the completed Direct Member Reimbursement Form?
After completing the form on pdfFiller, you can submit it directly through the platform or download it for mailing to your insurance provider. Confirm submission methods with your health plan.
What are common mistakes to avoid when filling out this form?
Common mistakes include incomplete fields, missing signatures, and incorrect or unclear supporting documents. Double-check your entries to ensure accuracy and compliance with form requirements.
How long does it usually take to process reimbursement requests?
Processing times can vary, but typically, reimbursements may take several weeks. For specific timelines, consult your insurance provider for their processing expectations.
Can I complete the Direct Member Reimbursement Form electronically?
Yes, you can fill out the Direct Member Reimbursement Form electronically using pdfFiller, which provides an easy-to-use interface for completing and saving your form.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.