Last updated on Aug 1, 2015
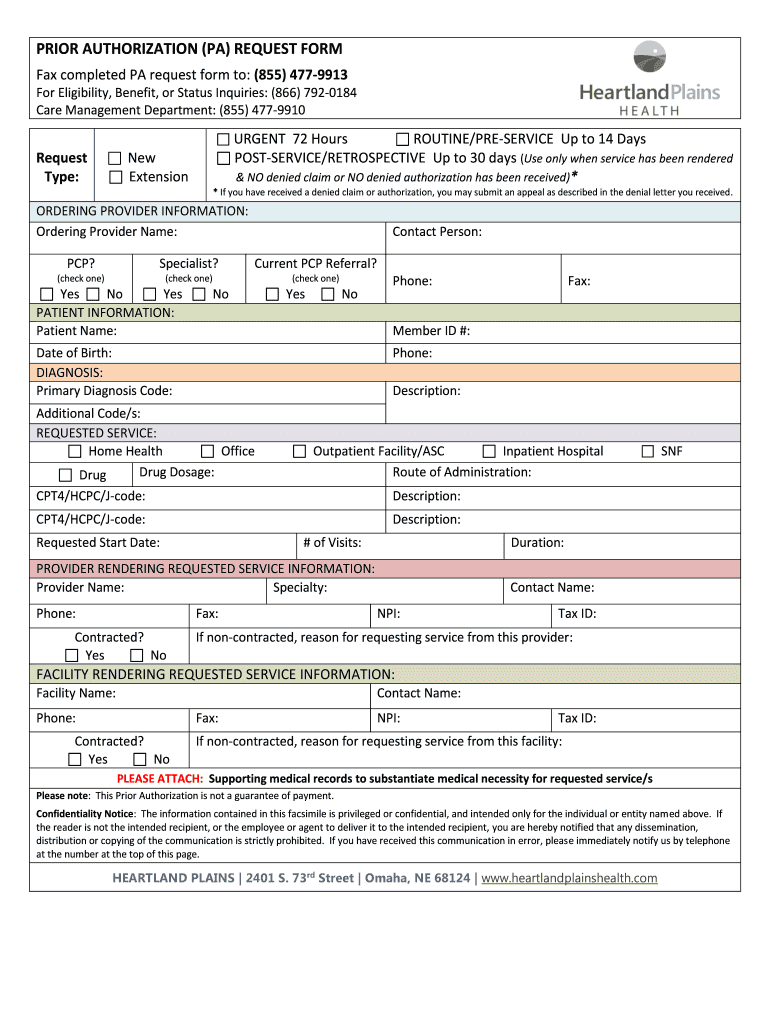
Get the free Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is PA Request Form
The Prior Authorization Request Form is a healthcare document used by providers to obtain approval for medical services or treatments from an insurance company.
pdfFiller scores top ratings on review platforms




Who needs PA Request Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to PA Request Form
What is the Prior Authorization Request Form?
The Prior Authorization Request Form is an essential document used within the healthcare process to obtain prior approval from insurance companies for specific medical services. This form plays a critical role in ensuring that the requested treatments adhere to necessary standards of medical necessity. Insurance companies review these requests to determine if the proposed services are justified based on the patient's health plan.
Purpose and Benefits of the Prior Authorization Request Form
Healthcare providers utilize the Prior Authorization Request Form to streamline the approval process, which provides significant benefits for both patients and practitioners. For patients, this form can lead to cost savings and assurance that they receive required treatments.
-
Facilitates clear communication between service providers and insurers.
-
Timely approvals can enhance the overall quality of patient care.
Key Features of the Prior Authorization Request Form
The form contains several important fillable fields that must be accurately completed. Key components include the Ordering Provider Name, Patient Name, and Primary Diagnosis Code. Clear instructions are provided to assist in fulfilling these fields effectively, and it is crucial to attach any supporting medical records to substantiate the request.
Eligibility Criteria for the Prior Authorization Request Form
Understanding who can submit the Prior Authorization Request Form is essential for efficient healthcare delivery. Typically, licensed healthcare providers such as physicians and specialists are eligible to utilize this form. Furthermore, certain medical services or treatments require prior authorization, while there are also exceptions where authorization may not be necessary.
How to Fill Out the Prior Authorization Request Form Online (Step-by-Step)
Filling out the Prior Authorization Request Form online can be straightforward if followed carefully. Here’s a step-by-step guide:
-
Begin by entering the Ordering Provider Name.
-
Provide the Patient Name and relevant diagnosis information.
-
Complete other essential fields as required in the form.
-
Attach necessary supporting medical records as instructed.
-
Review the filled form to ensure accuracy.
Common pitfalls include missing information or incorrect coding, which should be avoided to ensure timely processing.
Submission Methods and Delivery for the Prior Authorization Request Form
The submission of the Prior Authorization Request Form can be carried out through various methods. Electronic submission via platforms like pdfFiller is a convenient option, allowing for quick processing.
-
Traditional methods include mail and fax, but these can lead to delays.
-
Confirmation processes should be adopted to track the submission status promptly.
What Happens After You Submit the Prior Authorization Request Form?
Once the Prior Authorization Request Form is submitted, the insurance company undertakes a review process. Typically, applicants can expect a response within a specified timeline, which varies by insurer. Outcomes can differ, leading to either approval or denial of services, and understanding these implications is vital.
-
In cases of denial, it is possible to remedy the situation through resubmission, which may entail providing additional information.
Security and Compliance when Handling the Prior Authorization Request Form
When dealing with sensitive information, security and compliance are paramount. pdfFiller employs extensive security measures, including 256-bit encryption and adherence to HIPAA and GDPR regulations, ensuring patient data protection.
-
Best practices for protecting information should be followed during the filling and submission process.
-
Safeguarding medical records shared with insurers is also essential.
Enhancing Your Experience with pdfFiller
Utilizing pdfFiller's platform offers numerous advantages when handling the Prior Authorization Request Form. The platform supports various functionalities such as eSigning, editing, and document sharing, allowing users to manage their forms efficiently.
-
Accessing the service from any device adds significant convenience.
-
Enhanced user-friendliness contributes to an efficient document management experience.
Ready to Get Started?
Start taking control of your healthcare journey today by utilizing pdfFiller’s tools to complete the Prior Authorization Request Form. With these resources, you can ensure that your necessary medical services are authorized promptly and efficiently.
How to fill out the PA Request Form
-
1.Visit pdfFiller and log in or create an account to access the Prior Authorization Request Form.
-
2.Use the search bar or navigate to the healthcare forms section to find the Prior Authorization Request Form.
-
3.Begin by entering information in the 'Ordering Provider Name' field. Collect necessary details about the provider beforehand.
-
4.Complete the 'Patient Name' field with the patient's full name. Ensure the name matches exactly as recorded in the insurance documents.
-
5.Fill in the 'Primary Diagnosis Code' with the accurate code corresponding to the patient's condition. Refer to the latest coding systems for accuracy.
-
6.Specify the 'Requested Start Date' for the medical service. Confirm with the patient or their medical provider to set the correct date.
-
7.Use the checkboxes to indicate if the patient is under a Primary Care Physician or if a Specialist is involved. Review the options carefully.
-
8.Attach any required supporting medical records or documents that validate the medical necessity of the requested service using the ‘upload’ feature.
-
9.Once all fields are filled out correctly, review the form for any inaccuracies or missing information. Use pdfFiller’s editing tools for adjustments.
-
10.Click 'Save' to ensure your progress is not lost. You can also download a copy of the form for your records or future reference.
-
11.To submit the form, follow the specified submission process outlined by your insurance company, or use the 'Submit' feature in pdfFiller to send it directly.

Who is eligible to use the Prior Authorization Request Form?
The Prior Authorization Request Form is typically used by licensed healthcare providers seeking approval for medical services on behalf of their patients from insurance companies.
What information is required to complete the form?
Key information includes the ordering provider's details, patient name, primary diagnosis code, requested service, and supporting documentation to substantiating medical necessity.
How do I submit the Prior Authorization Request Form?
Once the form is completed, it can be submitted according to the procedures established by the patient's insurance company, which may include electronic submission or mailing.
What are some common mistakes to avoid when filling out the form?
Common mistakes include incorrect patient or provider information, missing signature fields, and failing to attach necessary supporting documents. Always double-check your entries.
How long does it take to process the Prior Authorization Request?
Processing times for prior authorization requests can vary. Typically, it may take several days to a few weeks, depending on the insurance company and the complexity of the request.
Are there any fees associated with submitting the Prior Authorization Request?
Generally, there are no direct fees for submitting the Prior Authorization Request Form, but it is advised to check if your healthcare provider or insurance plan has any specific charges.
Where can I find additional guidance on completing the form?
You can find further assistance by reviewing guidelines provided by the insurance company or consulting with administrative staff at your healthcare facility.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.






















