Last updated on Aug 9, 2015

Get the free Prior Authorization Standard Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

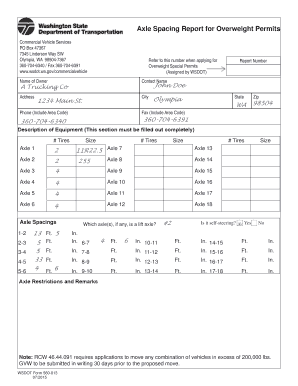
What is Prior Authorization Form
The Prior Authorization Standard Request Form is a medical authorization document used by healthcare providers to request approval for medical services.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Prior Authorization Standard Request Form?
The Prior Authorization Standard Request Form plays a crucial role in healthcare by facilitating the authorization process for medical services. This form is utilized by healthcare providers to obtain approval for various treatments, ensuring that patients receive timely care. However, certain services, such as durable medical equipment (DME) and home health, are excluded from this authorization form. Understanding this form is vital for both healthcare providers and patients, as it streamlines access to necessary medical services.
Purpose and Benefits of the Prior Authorization Standard Request Form
This form simplifies the medical service approval process, ultimately benefiting patients and healthcare providers alike. It reduces delays in patient treatment by providing a clear pathway for authorization requests. Additionally, it enhances communication between providers and insurance companies, ensuring that all parties are aligned on the requirements and processes involved in obtaining authorization.
Who Needs to Utilize the Prior Authorization Standard Request Form?
The Prior Authorization Standard Request Form is primarily intended for healthcare providers who are seeking authorization for treatments. It is essential for providers to understand which patients are eligible under different insurance plans. Furthermore, this form serves as a resource for providers looking to improve their understanding of the authorization process, contributing to better patient outcomes.
Key Features of the Prior Authorization Standard Request Form
The form includes several required fields, such as member information, provider details, diagnosis, and procedure codes. Supporting documentation is critical for processing requests efficiently. Additionally, the form allows space for patient history and notes, making it a comprehensive tool for healthcare providers.
How to Fill Out the Prior Authorization Standard Request Form Online
Filling out the Prior Authorization Standard Request Form online can be done in a few simple steps. First, users should carefully complete each field, ensuring that all information is accurate and complete. Next, instructions for submitting the form via pdfFiller should be followed closely. Lastly, users should be aware of common errors to avoid, such as omitting required documentation or incorrectly filling out fields.
Required Documents and Supporting Materials
When submitting the Prior Authorization Standard Request Form, several types of documents are typically required. These may include medical records, test results, and any other relevant documentation that supports the authorization request. To ensure a smooth submission process, it is advisable to organize all necessary materials beforehand, minimizing the risk of delays.
Submission Process and Delivery of the Prior Authorization Standard Request Form
The submission process for the Prior Authorization Standard Request Form can be completed through various methods. Healthcare providers can submit the form online, via mail, or by fax. Once the form is submitted, processing time typically takes around 14 days. Providers should also ensure they confirm receipt of the submission and track the status of their request for any necessary follow-up.
Common Reasons for Rejection and How to Avoid Them
Claims submitted through the Prior Authorization Standard Request Form may face rejection for a number of reasons. Common pitfalls include incomplete information or lack of sufficient supporting documentation. To enhance the chances of approval, providers should double-check all information and ensure that they have attached all required documents before submission.
Security and Compliance When Handling the Prior Authorization Standard Request Form
When using pdfFiller to submit the Prior Authorization Standard Request Form, users can be assured of data security and compliance with regulations. The platform employs 256-bit encryption and adheres to HIPAA standards, ensuring that sensitive patient information is protected throughout the process. It is crucial to prioritize data protection, especially when dealing with healthcare authorization documents.
Your Solution to Filling the Prior Authorization Standard Request Form with pdfFiller
pdfFiller offers an efficient solution for completing the Prior Authorization Standard Request Form. Users can leverage its cloud-based platform for an easy and convenient filling experience. With features such as fillable forms, eSigning, and document-saving options, providers are encouraged to utilize pdfFiller for a streamlined submission process.
How to fill out the Prior Authorization Form
-
1.Start by accessing the Prior Authorization Standard Request Form on pdfFiller. Go to the pdfFiller website and use the search bar to find the form by its name.
-
2.Once you've located the form, open it in the pdfFiller editor. Familiarize yourself with the layout, including blank fields and checkboxes for user input.
-
3.Before completing the form, gather the necessary information, including member information, provider details, diagnosis and procedure codes, patient history, and any supporting documentation required.
-
4.Begin filling in the fields, starting with the member's details. Use the interactive fields to type in information directly or select options from checkboxes as needed.
-
5.Ensure accuracy while entering diagnosis and procedure codes. You may want to reference medical coding resources to avoid common errors.
-
6.Once all required fields are completed, review the form for any missing information or mistakes. Make sure that all supporting documentation is attached as needed prior to finalizing the form.
-
7.After reviewing, you can save the form directly on pdfFiller or download it to your device. Alternatively, submit the form through the platform, following the on-screen instructions for submission.

What are the eligibility requirements for using this form?
To use the Prior Authorization Standard Request Form, the healthcare provider must be authorized under the patient’s insurance plan to submit authorization requests for their services.
How long does processing take for requests submitted?
The typical processing time for this form is 14 days. Urgent requests should be communicated via phone for expedited handling.
What supporting documents are required with this form?
Supporting documents may include patient history, diagnosis codes, treatment plans, and any other relevant medical records that justify the service request.
How do I submit the completed form?
You can submit the completed Prior Authorization Standard Request Form directly through pdfFiller by following the submission instructions or download it and send it to the appropriate insurance provider.
Are there common mistakes to avoid when filling out this form?
Common mistakes include leaving fields blank, entering incorrect diagnosis and procedure codes, or failing to attach required supporting documents. Always double-check your information before submission.
What should I do if my request is denied?
If your authorization request is denied, contact the insurance company for clarification on the denial reasons and inquire about the appeal process to challenge the decision.
Is notarization required for this form?
No, the Prior Authorization Standard Request Form does not require notarization to be valid.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.