Last updated on Aug 18, 2015
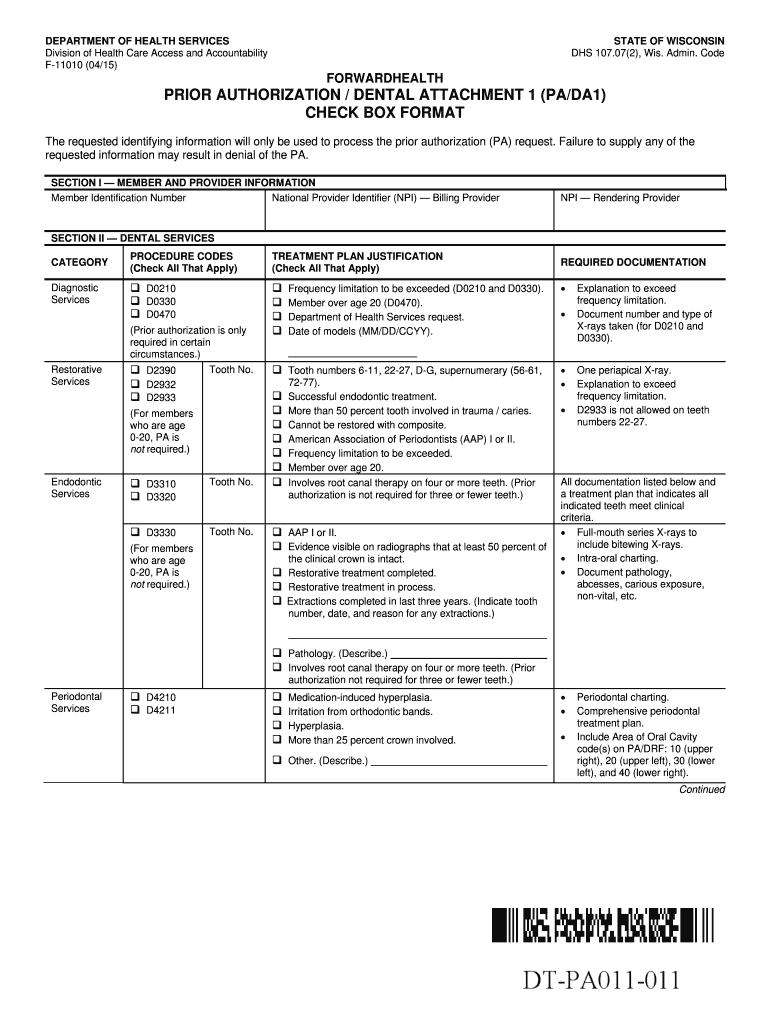
Get the free Wisconsin Dental Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Wisconsin Dental PA
The Wisconsin Dental Prior Authorization Form is a healthcare document used by providers to request prior authorization for dental services in Wisconsin.
pdfFiller scores top ratings on review platforms




Who needs Wisconsin Dental PA?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Wisconsin Dental PA
What is the Wisconsin Dental Prior Authorization Form?
The Wisconsin Dental Prior Authorization Form (PA/DA1) serves a critical role in healthcare by allowing providers to request authorization for dental services. This form is essential in ensuring that necessary procedures are pre-approved, which benefits both patients and healthcare providers. It requires specific information, including member and provider details along with the description of the dental procedures requested.
In addition to identifying requesting providers and members, the form also includes sections dedicated to the justification for the requested services, which must be completed accurately to avoid any potential delays.
Purpose and Benefits of the Wisconsin Dental Prior Authorization Form
This form is primarily used to clarify the necessity of prior authorization in dental treatment. By completing it correctly, healthcare providers can ensure the approval of services that their patients need. This not only aids providers in managing their practices efficiently but also helps patients access the appropriate care without unnecessary out-of-pocket costs.
Key benefits include:
-
Facilitating proper approval for dental services
-
Reducing costs through appropriate treatment validation
-
Streamlining the communication between healthcare providers and insurance companies
Who Needs the Wisconsin Dental Prior Authorization Form?
The primary users of the Wisconsin Dental Prior Authorization Form are healthcare providers in Wisconsin who seek authorization from insurance carriers. Eligibility criteria must be met to ensure the requesting provider can utilize this form effectively. Typically, the requesting provider is required to sign the form, affirming the necessity of the services outlined.
It's important for providers to be well-informed about the roles involved to navigate the process smoothly.
How to Fill Out the Wisconsin Dental Prior Authorization Form Online?
To fill out the Wisconsin Dental Prior Authorization Form online, providers can utilize pdfFiller, which simplifies the process significantly. Here’s a step-by-step guide:
-
Access the form through the pdfFiller platform.
-
Input member and provider information in the designated sections.
-
Detail the dental procedures and any necessary justifications.
-
Review the completed sections for accuracy to prevent submission delays.
Accurate completion of the form is crucial to ensure that all requests are processed promptly without complications.
Common Errors and How to Avoid Them When Completing the Form
When filling out the Wisconsin Dental Prior Authorization Form, users often make several common errors. These include incomplete fields or providing incorrect information that can lead to the rejection of requests.
To mitigate mistakes, consider these tips:
-
Double-check all information before submission.
-
Ensure all necessary fields are filled out completely.
-
Follow the given instructions meticulously to avoid misunderstandings.
Submission Methods and Important Deadlines for Wisconsin Dental Prior Authorization Form
Once completed, the Wisconsin Dental Prior Authorization Form can be submitted to various insurance carriers through multiple methods. Providers can choose between digital submission via platforms like pdfFiller or traditional mailing for physical forms. Adhering to submission deadlines is essential; failing to submit in a timely manner could result in delays or rejections of service requests.
Providers should be aware of specific deadlines to prevent late filing consequences and ensure efficient processing of prior authorization requests.
Tracking Your Submission and What Happens After You Submit the Form
After submitting the Wisconsin Dental Prior Authorization Form, providers can confirm their submission through various means, such as tracking numbers or confirmation emails. Understanding the review process is important, as it typically takes a defined amount of time for insurance providers to process requests.
Providers should be prepared for potential communication from insurance carriers regarding the status of their submissions, including approvals or requests for additional information.
How pdfFiller Can Help You Complete the Wisconsin Dental Prior Authorization Form
pdfFiller offers several features that greatly enhance the experience of filling out the Wisconsin Dental Prior Authorization Form. These include fillable fields, eSignature capabilities, and an intuitive platform for easy editing.
In addition to usability, pdfFiller ensures high levels of security and compliance when handling sensitive health information. This includes 256-bit encryption and adherence to legal standards, making it a trustworthy option for managing healthcare documents.
Sample or Example of a Completed Wisconsin Dental Prior Authorization Form
Providing a visual guide, such as a sample of a completed Wisconsin Dental Prior Authorization Form, can significantly aid users in understanding how to fill out the form effectively. This example highlights the significance of each section and showcases best practices observed in real submissions.
Accessing a downloadable sample can further reduce confusion and help ensure that all required fields are completed correctly.
Ensuring Security and Privacy When Using the Wisconsin Dental Prior Authorization Form
When utilizing the Wisconsin Dental Prior Authorization Form, data security and privacy are of utmost importance. pdfFiller employs robust security features, such as 256-bit encryption, to protect sensitive patient information during the completion and submission process.
Additionally, it's essential for users to understand the compliance measures in place, including adherence to HIPAA standards and SOC 2 Type II certifications, to ensure that their data remains confidential and secure throughout its lifecycle.
How to fill out the Wisconsin Dental PA
-
1.To access the Wisconsin Dental Prior Authorization Form on pdfFiller, visit the pdfFiller website and use the search bar to type in the form's name.
-
2.Once you locate the form, click on it to open in the pdfFiller interface. You will see the form displayed, which you can easily fill out.
-
3.Before starting, gather all necessary member and provider information, including dental procedure details and treatment plans that may be required.
-
4.Begin by filling in the member's information in the designated fields. Make sure to enter accurate names, dates of birth, and insurance details.
-
5.Next, move on to the provider information section. This will require the name of the requesting provider, along with their credentials and contact information.
-
6.Proceed to specify the dental procedures requested in the appropriate section. Each procedure may have specific codes or descriptions; ensure these are accurately detailed.
-
7.If appropriate, outline the treatment plan and justification for the requested services, providing as much detail as necessary to support the authorization request.
-
8.Utilize pdfFiller’s tools to check any boxes as needed. You can also add comments or additional information in the blank fields provided.
-
9.Once all required fields have been filled, take time to review the entire form for accuracy. Make sure all sections are complete and clear.
-
10.After verifying all information is correct, save your changes. You can do this by clicking the save button on the interface.
-
11.Finally, to download or submit the form, select the appropriate option in pdfFiller. You can email it directly from the platform or download a copy for personal records.

Who is eligible to use the Wisconsin Dental Prior Authorization Form?
This form is primarily intended for dental healthcare providers in Wisconsin seeking authorization from insurance companies for dental services. It is also relevant for patients requesting coverage.
Are there any specific deadlines for submitting this form?
While the metadata does not specify deadlines, it is generally advisable to submit prior authorization requests as early as possible. Check with your dental insurance provider for specific processing times.
How should I submit the completed Wisconsin Dental Prior Authorization Form?
You can submit the completed form either through the pdfFiller platform, using the email feature to send it directly to your insurance provider, or by downloading it and sending it through traditional mail or fax.
What supporting documents are typically required with this form?
Usually, you may need to attach supporting documents like treatment plans, x-rays, or clinical notes to provide additional justification for requested dental services.
What common mistakes should I avoid when filling out this form?
Common mistakes include omitting required fields, providing inaccurate information, and failing to gather necessary supporting documents. Review the form carefully before submission to avoid these errors.
What is the usual processing time for a prior authorization request?
Processing times can vary by insurance provider, but generally, expect a response within a few business days to a couple of weeks. Always verify this with your specific insurer.
Are there fees associated with the prior authorization process?
Typically, there are no direct fees for submitting a prior authorization request, but patients should confirm with their insurance to check for any potential costs related to the services requested.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.






















