Last updated on Sep 10, 2015

Get the free Pharmacy Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Form
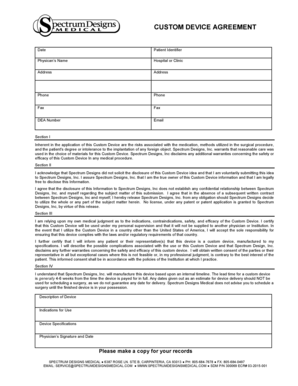
The Pharmacy Prior Authorization Form is a medical document used by healthcare providers to request approval for the drug Neulasta for patients undergoing specific chemotherapy treatments.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Pharmacy Prior Authorization Form?
The Pharmacy Prior Authorization Form is a crucial document utilized by healthcare providers to request authorization for specific medications, such as Neulasta (pegfilgrastim). This form is necessary in scenarios where prior clearance from insurance providers is essential for drug prescription and coverage.
This form is typically used by healthcare providers who treat patients undergoing chemotherapy. It ensures that medications, which may involve significant costs or regulatory scrutiny, can be prescribed appropriately. Without prior authorization, patients may face treatment delays or denials, impacting their healthcare journey.
Purpose and Benefits of the Pharmacy Prior Authorization Form
The primary function of the Pharmacy Prior Authorization Form is to secure authorization for particular treatments, greatly impacting patient care. By obtaining prior authorization, healthcare providers can facilitate cost coverage and treatment approval for patients.
Benefits include enhancing the appropriateness of medication use in chemotherapy and contributing to positive patient outcomes. This streamlined process not only improves healthcare efficiency but also minimizes the chances of unnecessary treatment interruptions.
Key Features of the Pharmacy Prior Authorization Form
This form incorporates several important sections that healthcare providers must complete accurately. Key information required includes patient diagnosis, dosing frequency, and provider details that are essential for the authorization process.
Moreover, the form mandates signature verification, emphasizing the need for meticulous completion. Specific sections and checkboxes must be selected, ensuring the form adheres to submission standards.
Eligibility Criteria for the Pharmacy Prior Authorization Form
To effectively use the Pharmacy Prior Authorization Form, specific eligibility criteria must be met. Generally, patients receiving chemotherapy for non-myeloid malignancies require this authorization to access particular medications.
Several factors may influence approval, including insurance policies and medical necessity. Age or specific health conditions may also play a role in a patient’s eligibility to utilize this form for authorization requests.
How to Fill Out the Pharmacy Prior Authorization Form Online (Step-by-Step)
Filling out the Pharmacy Prior Authorization Form online involves several clear steps to ensure accuracy. First, gather necessary patient and provider information, verifying that all data is complete before starting.
Follow these steps when completing the form:
-
Enter patient diagnosis and relevant medical history.
-
Provide dosing frequency and other medication specifics.
-
Ensure all fields are filled out, paying attention to signature requirements.
-
Double-check for any missing or incorrect details before submission.
By avoiding common pitfalls, you can enhance the likelihood of authorization approval.
Submission Methods and Delivery of the Pharmacy Prior Authorization Form
After completing the Pharmacy Prior Authorization Form, it’s essential to follow proper submission procedures. Different submission methods may include faxing, emailing, or using an online portal.
Adhering to specific delivery instructions is critical for avoiding delays in processing. Following up post-submission can help confirm that the request has been received and is being processed appropriately.
What Happens After You Submit the Pharmacy Prior Authorization Form?
Once the Pharmacy Prior Authorization Form is submitted, the request enters a review phase by insurance or healthcare providers. Understanding the potential outcomes is vital for users:
-
Approval of the authorization request.
-
Denial of the request for specified reasons.
-
Requests for additional information to support the authorization.
Tracking the status of the authorization can provide crucial updates and clarity during this process.
Common Errors and How to Avoid Them When Using the Pharmacy Prior Authorization Form
Users often encounter common mistakes that can lead to delays or denials of authorization. Typical errors include missing signatures or incomplete fields.
To ensure successful submission:
-
Review the form thoroughly for accuracy before submitting.
-
Use resources available for guidance if uncertain about any section.
Your diligence in these areas can help facilitate a smoother authorization process.
Security and Privacy when Handling the Pharmacy Prior Authorization Form
Handling sensitive information on the Pharmacy Prior Authorization Form raises significant security concerns. It is essential to prioritize data protection, given the confidential nature of patient information.
pdfFiller’s platform implements stringent security measures, including HIPAA compliance and encryption, to safeguard user data during submission. Additionally, users should reinforce their own security practices to protect sensitive information effectively.
Experience the Ease of Using pdfFiller for Your Pharmacy Prior Authorization Form
Utilizing pdfFiller streamlines the process of completing, signing, and submitting the Pharmacy Prior Authorization Form. The platform’s user-friendly features include e-signature capabilities and secure cloud storage.
Moreover, pdfFiller emphasizes security and efficiency, making it a trusted choice for healthcare forms. Users can experience the benefits of fast, secure document handling with the assurance of protected patient information.
How to fill out the Prior Authorization Form
-
1.Start by navigating to pdfFiller and searching for the Pharmacy Prior Authorization Form.
-
2.Open the form in pdfFiller's editor once you find it.
-
3.Gather all necessary patient information, including diagnosis and drug details before beginning.
-
4.Begin filling in the patient’s demographics in the indicated fields, ensuring accuracy.
-
5.Provide the requesting provider's information as well, including contact details.
-
6.In the medical history section, detail the relevant diagnoses and previous treatments.
-
7.Complete the medication section with the drug name, frequency, and dosage as per the requirements.
-
8.Review all entries for completeness and accuracy, ensuring there are no blank fields.
-
9.Once the form is filled out, locate the signature area and use pdfFiller's tool to insert the provider's signature.
-
10.Date the form appropriately before finalizing it for submission.
-
11.Save your completed form as a PDF using the 'Save' option.
-
12.Download it for personal records and submit it via fax to the specified numbers, following the submission guidelines.

What are the eligibility requirements for submitting this form?
Eligibility typically requires a medical necessity for Neulasta, with clear documentation of the patient's diagnosis and treatment plan aligning with drug guidelines.
Are there deadlines for submitting the Pharmacy Prior Authorization Form?
It is essential to submit the form as soon as possible before the patient's chemotherapy begins to avoid treatment delays. Check individual insurance policy requirements for specific timelines.
What method do I use to submit the completed form?
The completed Pharmacy Prior Authorization Form should be faxed to the designated numbers provided within your payer's authorization guidelines.
What supporting documents are required along with the form?
Typically, you will need to attach medical records or notes that justify the use of Neulasta for the patient’s chemotherapy treatment, along with any previous prescription history.
What are some common mistakes to avoid when submitting this form?
Avoid leaving any fields blank, double-check the accuracy of all information provided, and ensure that the form is signed and dated before submission.
How long does it take to process the Pharmacy Prior Authorization Form?
Processing times can vary depending on the insurance provider, but it generally takes between 24 to 72 hours for a decision to be made once submitted.
What if my request for prior authorization is denied?
If denied, you can appeal the decision by reviewing the denial letter, ensuring all justifications are clear, and resubmitting the form with additional information as needed.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.