Last updated on Sep 10, 2015

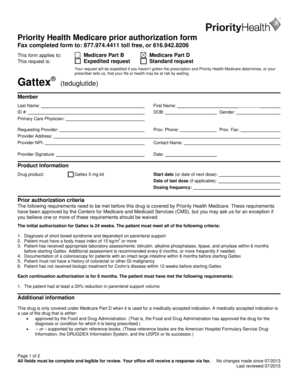
Get the free Pharmacy Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Form
The Pharmacy Prior Authorization Form is a healthcare document used by providers in the US to request authorization for specific medications like OxyContin.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
What is the Pharmacy Prior Authorization Form?
The Pharmacy Prior Authorization Form is a critical tool used by healthcare providers in the United States to request prior authorization for specific medications. This form plays a pivotal role in the medication approval process, ensuring that prescribed medications, especially those like OxyContin that may have higher risk factors, receive proper scrutiny based on medical necessity. The importance of this form cannot be understated, as it directly impacts patient access to essential treatments.
Purpose and Benefits of the Pharmacy Prior Authorization Form
Understanding the necessity of the Pharmacy Prior Authorization Form is imperative for both healthcare providers and patients. This form helps facilitate the approval of medications based on documented medical necessity and aids in reducing liability for medical professionals. Furthermore, it streamlines access to vital medications, improving the overall care experience for patients.
Among its various advantages, the form plays a central role in chronic pain medication authorization, ensuring that patients receive the treatments they need in a timely manner.
Who Needs to Use the Pharmacy Prior Authorization Form?
The Pharmacy Prior Authorization Form is primarily utilized by healthcare providers, who have the responsibility of submitting this form on behalf of patients. Patients prescribed medications requiring this form are also key players in the process, as their information and health history are essential for the approval. Understanding the roles and responsibilities of both providers and patients is crucial in navigating the prior authorization landscape effectively.
-
Healthcare providers are responsible for completing and submitting the form.
-
Patients must provide relevant health information and cooperate with their providers.
Key Features of the Pharmacy Prior Authorization Form
Key components of the Pharmacy Prior Authorization Form include detailed fields designed to gather essential information effectively. Providers must complete fields such as patient and provider details, medication specifics, and diagnosis descriptions to ensure a thorough submission. Additionally, it contains sections for supporting documents and explicit instructions for both completion and required signatures.
-
Comprehensive patient and provider information fields.
-
Sections for medication details and the patient’s diagnosis.
-
Clear instructions for form completion.
How to Complete the Pharmacy Prior Authorization Form Online (Step-by-Step)
Completing the Pharmacy Prior Authorization Form online requires attention to detail and accuracy. Follow these steps to ensure a successful submission:
-
Access the form and enter patient information, including ID and date of birth.
-
Detail the medication required, including dosage and frequency.
-
Provide information on the patient's diagnosis and past medication trials.
-
Attach any necessary supporting documents, such as the pain management contract.
-
Review all entries for legibility and completeness before submission.
Required Documents and Supporting Materials for the Pharmacy Prior Authorization Form
When submitting the Pharmacy Prior Authorization Form, including necessary supporting documentation is crucial for approval. Failure to include required materials can delay the process significantly. Key documents include medical chart notes from the last 90 days, ensuring that the treatment rationale is up-to-date and relevant.
-
Pain management contract.
-
Recent medical chart notes.
-
A checklist of all materials being submitted.
Submission Processes for the Pharmacy Prior Authorization Form
Understanding the submission process for the Pharmacy Prior Authorization Form can greatly affect its timely approval. The form can be submitted through various methods, including online platforms, fax, or traditional mail. It is essential to ensure all fields are filled out completely and legibly to avoid unnecessary delays.
-
Online submission via dedicated healthcare platforms.
-
Faxing the completed form to the appropriate healthcare provider.
-
Mailing the form if electronic options are not available.
Consequences of Not Filing or Late Filing the Pharmacy Prior Authorization Form
The risks associated with failing to file or submitting the Pharmacy Prior Authorization Form late can be significant. Delays in filing may lead to adverse patient outcomes, including challenges in obtaining necessary medications. Additionally, healthcare providers may face diminished patient satisfaction and potential impacts on their practice.
-
Delays in medication access can affect patient treatment outcomes.
-
Adherence to a 90-day resubmission timeline is crucial for ongoing medication needs.
How to Use pdfFiller for the Pharmacy Prior Authorization Form
pdfFiller offers an efficient solution for completing and managing the Pharmacy Prior Authorization Form online. The platform allows users to fill out and edit the form securely, eliminating concerns over document integrity. With features designed for eSigning and document management, pdfFiller enhances the submission process.
-
Use cloud-based tools for easy editing and filling of the form.
-
Leverage security features to protect sensitive patient information.
-
Access tools for eSigning and document sharing within the platform.
Next Steps After Completing the Pharmacy Prior Authorization Form
Once the Pharmacy Prior Authorization Form is completed and submitted, it is essential to follow up on the status of the authorization request to ensure timely processing. Additionally, understanding the renewal practices will help manage ongoing medication requirements effectively. Keeping a record of all submissions will serve as a useful reference for future authorizations.
-
Check the status of the authorization request consistently.
-
Be aware of timeframes for renewing medication needs.
How to fill out the Prior Authorization Form
-
1.To get started, access the Pharmacy Prior Authorization Form on pdfFiller by searching for its title. Once located, click on the form to open it in the editor.
-
2.Familiarize yourself with the pdfFiller interface. Use the navigation pane to move through the form sections effectively.
-
3.Before filling the form, gather necessary patient information such as the patient's last name, first name, date of birth, and medication details.
-
4.Begin filling out each field meticulously. Ensure you provide complete and legible information in fields like diagnosis, medication trials, and prescribing provider details.
-
5.Refer to the instructions provided within the form for specific requests such as inclusion of pain management contracts and recent medical chart notes.
-
6.After completing all fields, review the entire form to ensure accuracy and completeness. Double-check for any missing information.
-
7.When ready, use pdfFiller's tools to save your progress or download the completed form. You can also submit it directly through the platform if this option is available.

Who is eligible to use the Pharmacy Prior Authorization Form?
Healthcare providers who need to request prior authorization for medications from insurance companies, specifically for patients on treatments like OxyContin, are eligible to use this form.
What supporting documents are required with this form?
When submitting the Pharmacy Prior Authorization Form, you must include supporting documents such as a pain management contract and the most recent medical chart notes within the last 90 days.
How do I submit the Pharmacy Prior Authorization Form?
Once the form is completed, you can submit it directly to the insurance company via their preferred method, which may include online submission or mailing a hard copy.
What are the common mistakes to avoid when filling the form?
Common mistakes include leaving fields blank, not signing the form, and failing to attach required supporting documents like medical chart notes and pain management contracts.
What is the processing time for authorization requests?
Processing times for pharmacy prior authorization requests can vary, but typically, expect a response from insurance providers within 5-10 business days.
Are there any fees associated with using this form?
Generally, there are no fees for submitting the Pharmacy Prior Authorization Form itself, but providers may incur costs related to consultations or additional documentation needed.
What should I do if my request is denied?
If your request is denied, review the reasons for denial provided by the insurance company. You may need to gather additional information or appeal the decision with further documentation.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.