Last updated on Sep 10, 2015

Get the free Priority Health Medicare Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Medicare Prior Authorization
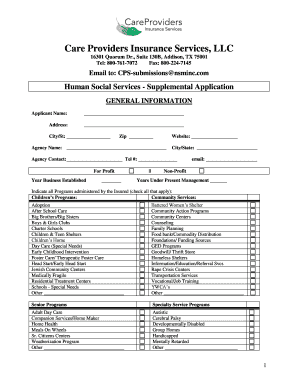
The Priority Health Medicare Prior Authorization Form is a medical document used by healthcare providers to request prior authorization for Relistor (methylnaltrexone) under Medicare Part B and Part D.
pdfFiller scores top ratings on review platforms




Who needs Medicare Prior Authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Medicare Prior Authorization
What is the Priority Health Medicare Prior Authorization Form?
The Priority Health Medicare Prior Authorization Form serves a crucial role in requesting prior authorization for medications under Medicare, specifically for Relistor. This document is essential for healthcare providers to obtain approvals necessary before prescribing certain treatments. By utilizing this form under Medicare Part B and D, providers ensure that the patient's treatment adheres to regulatory requirements, making it a vital component of the healthcare process.
It includes key information about the patient and the prescribed drug, which aids in expediting the treatment initiation.
Purpose and Benefits of the Priority Health Medicare Prior Authorization Form
Prior authorization is imperative for specific medications like Relistor due to insurance regulatory standards. This process verifies that the prescribed treatment is medically necessary and meets Medicare guidelines. Providers can greatly benefit from timely submissions, ensuring that patients receive their medications without unnecessary delays.
For patients, submitting this form accurately can lead to faster access to therapies and improved health outcomes. Utilizing it promotes a streamlined process to receive approvals efficiently.
Key Features of the Priority Health Medicare Prior Authorization Form
The form contains several critical fillable fields necessary for a successful request. Healthcare providers must provide detailed information, including but not limited to:
-
Patient personal data such as last name and date of birth
-
Drug product details and dosing frequency
-
Diagnosis for opioid-induced constipation
-
Prior treatments and the place of administration
Moreover, the form allows for exception requests if standard criteria do not apply. These features enable healthcare professionals to submit comprehensive and compliant requests for prior authorization.
Who Needs the Priority Health Medicare Prior Authorization Form?
Healthcare providers prescribing Relistor under Medicare must complete and submit this prior authorization form. Additionally, patients requiring this medication under Medicare are the ultimate beneficiaries of the authorization process.
Thus, both providers and patients play integral roles in utilizing this form effectively, ensuring the medication is accessible when needed.
How to Fill Out the Priority Health Medicare Prior Authorization Form Online
Filling out the Priority Health Medicare Prior Authorization Form online is a straightforward process. Follow these steps to ensure the form is completed accurately:
-
Access the form through the official platform.
-
Input the patient's details, including full name and Medicare ID.
-
Provide the prescribing provider's information.
-
Include the required drug information and patient diagnosis.
-
Review all fields for completeness and accuracy.
-
Submit the completed form electronically for processing.
Common Errors and How to Avoid Them
Several common mistakes occur during the completion of the Priority Health Medicare Prior Authorization Form. Identifying these pitfalls can help ensure a smoother submission process. Here are mistakes to watch out for:
-
Omitting required fields, leading to delays
-
Providing illegible handwriting in written submissions
-
Failing to include supporting documentation
To enhance accuracy, double-check all entries before submission to confirm that each field is filled out completely and clearly.
Submission Methods for the Priority Health Medicare Prior Authorization Form
Once the Priority Health Medicare Prior Authorization Form is completed, it can be submitted through various methods. The options include:
-
Emailing the form directly to the designated review team
-
Faxing the completed document
-
Online submission via the healthcare platform
Additionally, be mindful of submission deadlines and any associated fees that may apply, as these details are crucial in ensuring a timely review process.
What Happens After You Submit the Priority Health Medicare Prior Authorization Form?
Upon submission of the Priority Health Medicare Prior Authorization Form, it enters a review process. The Priority Health team will evaluate the request based on the information provided.
Healthcare providers can track the status of their submission through the designated online system, facilitating clear communication and updates regarding the authorization's outcome.
Maintaining Privacy and Security While Using the Priority Health Medicare Prior Authorization Form
It is critical to maintain privacy and security when handling sensitive documents, including the Priority Health Medicare Prior Authorization Form. pdfFiller implements robust security measures, such as:
-
256-bit encryption to protect data integrity
-
HIPAA compliance ensuring confidentiality of health information
These measures are necessary to safeguard patient information throughout the submission process and foster trust in handling sensitive healthcare documents.
Get Started with pdfFiller for the Priority Health Medicare Prior Authorization Form
Using pdfFiller for the Priority Health Medicare Prior Authorization Form offers numerous advantages. The platform provides an easy way to access, edit, and submit healthcare forms securely.
Employing pdfFiller streamlines the workflow, enabling users to focus on completing the form accurately without the hassle of physical paperwork.
How to fill out the Medicare Prior Authorization
-
1.Start by accessing the Priority Health Medicare Prior Authorization Form on pdfFiller's website. Use the search bar or browse through the healthcare forms section to locate it.
-
2.Once the form is opened, familiarize yourself with the layout and the fillable fields. You will need to enter patient information and details regarding the medication.
-
3.Gather all necessary information before you begin filling out the form. This includes the patient’s demographic details, provider's contact information, and specifics regarding the drug product.
-
4.Begin entering data in the required fields such as 'Last Name,' 'First Name,' 'ID #,' and relevant medication details. Ensure all entries are clear and legible.
-
5.Utilize the navigation tools to move seamlessly from one field to another. Use the tab key or your cursor for efficient entry. Select checkboxes for any applicable options.
-
6.After completing all sections, review the information entered to confirm accuracy and completeness. Pay special attention to conditional fields and required signatures.
-
7.Finalize the form by saving it as a draft or download it for submission. If you're ready to submit, use pdfFiller’s submission options which might include email or integration with other services.

Who is eligible to use the Priority Health Medicare Prior Authorization Form?
The form is primarily for healthcare providers submitting requests on behalf of patients needing prior authorization for Relistor under Medicare guidelines.
What is the deadline for submitting the form?
While specific deadlines may vary, it’s generally recommended to submit the prior authorization request as soon as possible to avoid treatment delays.
How do I submit the completed form?
You can submit the completed Priority Health Medicare Prior Authorization Form through your provider's office via fax or electronic submission as instructed by Priority Health.
What supporting documents are required with the form?
Typically, you may need to provide diagnosis codes, previous treatment records, and any required clinical notes that justify the request for prior authorization.
What are common mistakes to avoid when filling out the form?
Common mistakes include missing required fields, entering incorrect patient information, and failing to provide complete diagnosis details that may result in processing delays.
How long does it take to process the form?
Processing times can vary, but approvals typically take several days. It's advisable to check with Priority Health for specific timelines regarding your submission.
What should I do if my prior authorization request is denied?
If denied, consult the denial letter for reasons and consider reaching out to Priority Health to discuss further steps or appeal options available for your request.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.