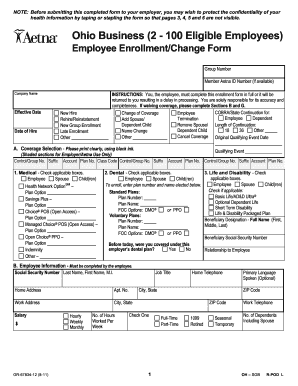
Last updated on Oct 18, 2015

Get the free Cigna Behavioral Health Out-of-Network Claim Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Cigna Claim Form
The Cigna Behavioral Health Out-of-Network Claim Form is a health insurance claim document used by employees to submit claims for behavioral health services not covered by their insurance provider.
pdfFiller scores top ratings on review platforms




Who needs Cigna Claim Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Cigna Claim Form
Understanding the Cigna Behavioral Health Out-of-Network Claim Form
The Cigna Behavioral Health Out-of-Network Claim Form is an essential tool for employees to submit claims for behavioral health services outside their insurance network. This form’s primary function is to facilitate the reimbursement process by documenting necessary details about the services rendered. Employees often need this form when they receive care from non-network providers, ensuring they can still seek necessary treatment without financial burdens.
Its significance lies in bridging the gap between out-of-network care and eligible reimbursements, allowing employees to maintain access to quality mental health support.
Why Use the Cigna Behavioral Health Out-of-Network Claim Form?
Utilizing the Cigna claim form for out-of-network services offers several key advantages. Firstly, it enables employees to claim for services that may not be directly covered under their current plan. Secondly, completing this form helps ensure that all critical information is documented correctly, leading to a more efficient claims process.
Submitting detailed claims through this form can significantly enhance the likelihood of receiving accurate reimbursements, making it a critical step for those managing healthcare costs.
Who Needs to Complete the Cigna Behavioral Health Out-of-Network Claim Form?
This form is primarily designed for employees who have opted for behavioral health services that are not included in their insurance network. To qualify for submitting a claim through this form, employees must meet specific eligibility criteria that often include ensuring the services were medically necessary and documented appropriately.
Additionally, patients receiving care for behavioral health issues should be aware of the need for this form to address their claims effectively, as it is pivotal for securing their reimbursement.
How to Fill Out the Cigna Behavioral Health Out-of-Network Claim Form
To complete the Cigna claim form, follow these detailed steps:
-
Start by providing your personal information in the designated sections.
-
Input patient details, ensuring accuracy in names and dates.
-
Describe the services rendered, including dates, diagnoses, and costs associated with each service.
-
Double-check for common errors, such as incorrect spelling or missing signatures.
Careful attention to these elements will help prevent delays or rejections of the claims.
Submission Process for the Cigna Behavioral Health Out-of-Network Claim Form
After completing the form, follow these steps for submission:
-
Submit the form via email, postal mail, or through your Cigna account online.
-
Ensure you keep a copy of the claim for your records.
-
Pay attention to any submission deadlines to avoid potential issues.
Timely submission is crucial for ensuring a smooth reimbursement process.
Supporting Documentation for the Cigna Behavioral Health Out-of-Network Claim Form
When submitting the claim form, it is essential to include the following supporting materials:
-
Itemized bills from the healthcare provider detailing services rendered.
-
Any recommended treatment plans or notes that substantiate the need for services.
Gathering and submitting these documents is vital for expediting the claims processing and ensuring that your submission is complete and accurate.
Tracking Your Cigna Behavioral Health Out-of-Network Claim Submission
Once you have submitted your claim, here's what to anticipate:
-
Most claims will be acknowledged within a few business days.
-
You can check the status of your claims through your online Cigna account or by contacting support.
-
Be aware that common reasons for delays or rejections can often relate to incomplete documentation or missing signatures.
Keeping track of your claim status is essential for peace of mind and financial planning.
How pdfFiller Can Help with the Cigna Behavioral Health Out-of-Network Claim Form
pdfFiller offers several features to streamline the process of filling out the Cigna insurance form. With its cloud-based platform, users can complete forms quickly and securely from any browser without installations. Enhanced security measures ensure that sensitive information remains protected throughout the process.
Using pdfFiller enhances user experience, allowing for efficient form filling and submission, making the process less cumbersome.
Secure Your Documents with pdfFiller
When using pdfFiller, you can feel confident about the security of your information. The platform employs 256-bit encryption and adheres to HIPAA compliance standards, ensuring that both personal and sensitive data are safeguarded. By using pdfFiller, you can also enjoy organized document management, keeping your files easily accessible while maintaining privacy.
Final Steps to Ensure Successful Claims Submission
Before submitting the Cigna Behavioral Health Out-of-Network Claim Form, recap the essential steps:
-
Verify that all fields on the form are completed accurately.
-
Ensure that all supporting documents are included and organized.
By following these final steps, you can greatly reduce the risk of errors and enhance the efficiency of your claims process.
How to fill out the Cigna Claim Form
-
1.Access the Cigna Behavioral Health Out-of-Network Claim Form by navigating to pdfFiller and using the search bar or the provided link.
-
2.Open the form, and familiarize yourself with its layout and sections designed for detailed information input.
-
3.Before completing the form, gather necessary information, including employee details, patient information, dates of services, diagnoses, and associated costs.
-
4.Use the text fields to input details accurately. Click on each field to type in information or select from dropdown menus where applicable.
-
5.Make sure to fill in checkboxes where necessary to provide additional information regarding the claim.
-
6.After you’ve filled out all required fields, double-check the entered information for accuracy and completeness.
-
7.Once finalized, look for options on the interface to save your progress, download it, or prepare for submission through pdfFiller.
-
8.Review all details one more time and use the 'Submit' function to send the completed claim form along with any itemized billing documents.

Who is eligible to use the Cigna Behavioral Health Out-of-Network Claim Form?
Any employee covered by a Cigna health insurance plan who has received behavioral health services that are not covered by their plan can utilize this form to submit claims for reimbursement.
What documents do I need to submit with the claim form?
You need to include an itemized bill detailing the services rendered along with your completed Cigna Behavioral Health Out-of-Network Claim Form to ensure proper processing of your claim.
How do I submit the Cigna claim form after completion?
After completing the Cigna Behavioral Health Out-of-Network Claim Form on pdfFiller, you can submit it electronically through the platform or print it out to mail it to the appropriate Cigna claims department.
What are common mistakes to avoid when completing the claim form?
Common pitfalls include incomplete fields, errors in patient or employee information, and failing to attach required supporting documents like itemized billing. Make sure to triple-check your entries.
What is the expected processing time for claims submitted?
Typically, processing times for health claims like the Cigna Behavioral Health Out-of-Network Claim Form can vary, but you can usually expect a response within 30 days of submission, provided all required documents are included.
Can I make changes to the claim form after it has been submitted?
Once submitted, changes to a claim form typically cannot be made. If necessary, you would need to follow up directly with Cigna’s claims department to address any issues.
Related Catalogs
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.