Last updated on Oct 22, 2015

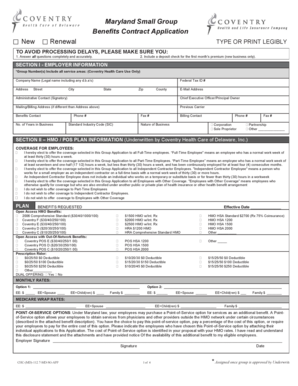
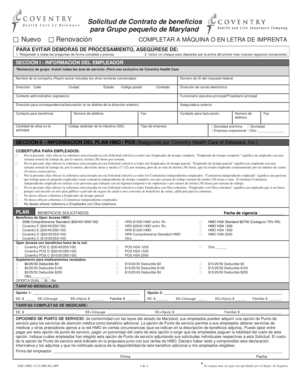
Get the free Samsca Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Samsca PA Form
The Samsca Prior Authorization Request Form is a healthcare document used by prescribers to request prior authorization for the medication Samsca®.
pdfFiller scores top ratings on review platforms




Who needs Samsca PA Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Samsca PA Form
What is the Samsca Prior Authorization Request Form?
The Samsca Prior Authorization Request Form serves a critical role in healthcare by enabling providers to request necessary medication approval. This form requires essential details such as the patient's diagnosis and the corresponding ICD code, ensuring that healthcare providers can secure the authorization needed for treatments.
This form is utilized when a medication like Samsca® needs prior approval from insurance companies before it can be dispensed. Understanding its purpose helps streamline the approval process and improve patient care.
-
Definition: A document for medication approval requests.
-
Usage: Necessary for securing treatment coverage.
Who Needs the Samsca Prior Authorization Request Form?
The Samsca Prior Authorization Request Form is essential for various roles in the healthcare ecosystem. Primarily, healthcare providers and prescribers are responsible for filling out this form to seek approval for the medication.
Patients who require Samsca® for their treatment may benefit significantly from this form, as it helps ensure they receive their medications in a timely manner. Understanding who needs this form fosters better communication between patients and their healthcare teams.
-
Primary users: Healthcare providers and prescribers.
-
Beneficiaries: Patients requiring Samsca® medication.
Key Features of the Samsca Prior Authorization Request Form
The Samsca Prior Authorization Request Form is designed with user-friendliness in mind, featuring multiple fillable fields. Important fields include 'Patient Name,' 'Patient’s ID,' and 'Physician’s Name,' which must be accurately completed for the form to be valid.
A critical aspect of this form is the prescriber’s signature, which acts as verification of the request. Recognizing the template nature of this document can facilitate more straightforward usage for healthcare professionals.
-
Key fields: 'Patient Name,' 'Patient’s ID,' 'Physician’s Name.'
-
Prescriber’s signature required: Essential for validation.
-
Template form: Streamlined design for ease of use.
How to Fill Out the Samsca Prior Authorization Request Form Online
Filling out the Samsca Prior Authorization Request Form online can be accomplished efficiently with the right approach. Begin by inputting patient information accurately, ensuring that all required fields are completed to prevent delays.
Choose the appropriate diagnosis from the provided options, and double-check each entry for possible errors. Utilizing tools like pdfFiller enhances this process, offering cloud-based editing features that simplify form completion.
-
Step 1: Fill out patient information.
-
Step 2: Select the correct diagnosis.
-
Avoid errors: Double-check entries before submission.
Submission Methods and Processing of the Samsca Prior Authorization Request Form
Once completed, the Samsca Prior Authorization Request Form must be submitted for processing. Faxing the filled form to CVS/Caremark is a standard submission method that healthcare providers should follow closely.
Post-submission, users can expect various processing times and potential fees based on their insurance provider. It's essential to stay informed about the status of the application and be aware of common rejection reasons to address issues promptly.
-
Submit by faxing the completed form.
-
Understand potential fees and processing times.
-
Track application status to monitor progress.
Required Documents and Supporting Information
Accompanying documents are vital when submitting the Samsca Prior Authorization Request Form. These may include medical records and insurance information, which provide necessary context for the approval process.
To streamline submissions, consider using a pre-filing checklist to ensure all required documents are gathered ahead of time, minimizing delays and enhancing the likelihood of approval.
-
Supporting documents: Medical records, insurance information.
-
Pre-filing checklist: Ensure all necessary documents are ready.
Security and Compliance with the Samsca Prior Authorization Request Form
Ensuring the security of sensitive information is paramount when handling the Samsca Prior Authorization Request Form. pdfFiller employs robust security features, including 256-bit encryption and adherence to regulations like HIPAA.
By prioritizing patient data protection and confidentiality during the prior authorization process, healthcare providers can maintain trust while navigating complex healthcare requirements.
-
Security features: 256-bit encryption.
-
Regulatory compliance: HIPAA compliance is essential.
-
Importance of confidentiality in patient data handling.
Streamlining Your Prior Authorization Requests with pdfFiller
Utilizing pdfFiller can significantly enhance the experience of filling out the Samsca Prior Authorization Request Form. Key functionalities such as eSigning, online form completion, and document sharing make the submission process more efficient.
With features that simplify editing and ensure accuracy, healthcare providers can confidently submit requests, minimizing turnaround times and enhancing overall service delivery to patients.
-
eSigning capability: Facilitate faster approvals.
-
Online form completion: Eliminates paper usage.
-
Document sharing: Easy collaboration among healthcare teams.
Examples and Resources for the Samsca Prior Authorization Request Form
Access to visual aids and additional information about the Samsca Prior Authorization Request Form is invaluable. Users can refer to sample forms or completed versions to understand submission requirements better.
Moreover, links to related resources and insightful readings about prior authorization processes can further assist users in navigating this healthcare necessity.
-
Sample forms: Access examples for reference.
-
Related resources: Explore further readings.
How to fill out the Samsca PA Form
-
1.To access the Samsca Prior Authorization Request Form on pdfFiller, visit the pdfFiller website and log in or create an account if you do not have one.
-
2.Use the search function to locate the 'Samsca Prior Authorization Request Form' and select it to open the document in the editing interface.
-
3.Carefully review the form fields, including 'Patient Name', 'Date', 'Patient’s ID', and 'Physician’s Name'. Gather relevant patient and physician information to fill in these fields accurately.
-
4.Click on each fillable field to input the necessary details. You can use pdfFiller's text tools to ensure clarity and legibility.
-
5.If you have the patient’s diagnosis and ICD code, locate the appropriate fields on the form and enter this information, ensuring accuracy for the approval process.
-
6.Before finalizing, review the entire form to ensure all fields are filled correctly and the prescriber’s signature is included.
-
7.Once completed, save your progress. You can download the filled form directly to your device or submit it electronically depending on the options provided by pdfFiller.
-
8.To submit the form, fax it to CVS/caremark as indicated in the instructions within the form. Ensure you keep a copy for your records.

Who can complete the Samsca Prior Authorization Request Form?
The Samsca Prior Authorization Request Form should be completed by a prescriber, such as a physician or qualified healthcare professional. It is essential for requesting medication approval for patients diagnosed with conditions warranting the use of Samsca®.
What information is required on the form?
The form requires details such as the patient's name, identification number, physician's name, the patient’s diagnosis, and the corresponding ICD code. Ensure all fields are filled accurately to avoid processing delays.
How do I submit the completed form?
After completing the Samsca Prior Authorization Request Form, you must fax it to CVS/caremark for processing. Refer to the specific submission instructions included on the form itself or through your pharmacy.
Are there any deadlines for submitting this form?
There are no specific deadlines mentioned for the Samsca Prior Authorization Request Form submission; however, it is advisable to submit the form as soon as possible to ensure timely medication approval. Always check with insurance for any specific timelines.
What common mistakes should I avoid?
Common mistakes include leaving fields blank, providing incorrect or incomplete diagnosis codes, failing to include the prescriber’s signature, and not faxing to the correct number. Double-check all entries before submission.
How long does it take to process the request?
Processing times for prior authorization requests can vary. Typically, it may take a few business days, but you should check with CVS/caremark for specific timelines and to track the status of your submission.
Do I need supporting documents with the form?
Depending on individual circumstances, it may be necessary to include additional supporting documents such as clinical notes or test results. Verify with your insurance provider for specific requirements.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.