Last updated on Mar 7, 2026

Get the free prior authorization for adjunct
Show details
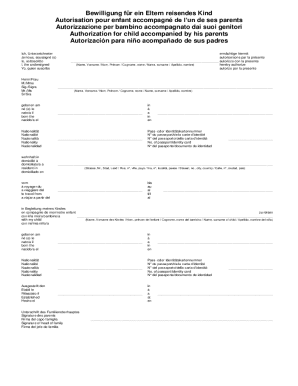
Prior Authorization for Adjunct Request Form Adjunct MH OP and other disallowed services require Prior Authorization to ensure that duplication of services does not occur with a currently approved
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is prior authorization for adjunct
The Prior Authorization for Adjunct Request Form is a healthcare document used by providers to obtain prior authorization for adjunct mental health outpatient services.
pdfFiller scores top ratings on review platforms




Who needs prior authorization for adjunct?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to prior authorization for adjunct
What is the Prior Authorization for Adjunct Request Form?
The Prior Authorization for Adjunct Request Form serves a critical role in mental health outpatient services. Healthcare providers utilize this form to request authorization for additional mental health services that are not typically covered. This ensures that patients receive comprehensive care tailored to their needs.
Providers use the prior authorization adjunct request form in various scenarios, especially when they seek to prevent service duplication that might already be approved under a member’s current Level of Care. Understanding the context and appropriate use of this form is essential for effective patient management.
Purpose and Benefits of the Prior Authorization for Adjunct Request Form
This form is designed to guarantee coverage for additional services that may not be routinely included in standard mental health outpatient services. By using the prior authorization adjunct request form, healthcare providers can enhance care delivery while also ensuring efficient use of available resources.
Additionally, the form aids in preventing the duplication of previously authorized services, thus fostering a streamlined approach to patient care and allowing providers to focus on what is essential for their patients' health.
Key Features of the Prior Authorization for Adjunct Request Form
-
Member Information section to capture patient details accurately.
-
Provider Information section that identifies the healthcare provider submitting the request.
-
Authorization Request section, which specifies the services being requested.
Specific data required on the form includes diagnosis codes and current approved services. Accurate completion of these fields is of utmost importance, as it directly influences the approval process and overall efficiency of care.
Who Needs the Prior Authorization for Adjunct Request Form?
The adjunct request form template must be completed by licensed healthcare providers who are seeking additional services for their patients. This form is necessary in several scenarios, particularly when standard coverage does not apply to specific services needed by the member.
Providers must ensure they meet the requirements for submission to facilitate the authorization process effectively, reinforcing their role in patient advocacy and care continuity.
How to Fill Out the Prior Authorization for Adjunct Request Form Online (Step-by-Step)
-
Begin with the Member Information section; provide all necessary patient details.
-
Complete the Provider Information section accurately to identify yourself.
-
Fill out the Authorization Request section, including all diagnosis codes and requested services.
-
Review all entries for accuracy before submitting the form online.
-
Submit the completed form through the designated submission methods.
Ensuring accuracy in diagnoses and service requests is critical to avoid delays or potential denials during the approval process.
Common Errors and How to Avoid Them
When filling out the prior authorization adjunct request form, providers frequently encounter several common errors. These may include incomplete information, incorrect diagnosis codes, or misunderstanding the documentation requirements.
-
Double-check entries in all fillable fields.
-
Ensure diagnosis codes match the requested services accurately.
-
Review previously approved services to avoid duplication.
Implementing a checklist for submission can help streamline the process and reduce the likelihood of mistakes.
Where and How to Submit the Prior Authorization for Adjunct Request Form
The submission of the prior authorization adjunct request form can be accomplished through several methods including online, via mail, or other specified methods based on the provider's preference. It is important to verify if there are any associated fees and be aware of deadlines for submission.
Understanding the processing times for submissions is also crucial for effective planning in patient care, as it affects when additional services can be accessed.
What Happens After You Submit the Prior Authorization for Adjunct Request Form?
After submission, providers can typically expect confirmation of receipt and specific processing timelines related to the request. Understanding the review process helps in managing patient expectations and planning follow-up actions if necessary.
Providers should also be prepared to check the application status regularly and know how to respond to potential rejections or requests for additional information.
Security and Compliance for the Prior Authorization for Adjunct Request Form
The security of sensitive information submitted through the prior authorization adjunct request form is paramount. pdfFiller employs advanced security measures to protect such data, ensuring compliance with HIPAA and GDPR regulations.
These measures provide peace of mind for healthcare providers as they navigate the complexities of patient authorization seamlessly and securely.
Seamlessly Fill Out the Prior Authorization for Adjunct Request Form with pdfFiller
Utilizing pdfFiller's tools allows healthcare providers to edit, sign, and manage the Prior Authorization for Adjunct Request Form seamlessly. The platform offers a convenient and secure method to access and submit forms online, enhancing efficiency in patient administration.
By leveraging these user-friendly capabilities, providers can streamline their workflows while ensuring thorough completion of essential documentation.
How to fill out the prior authorization for adjunct
-
1.Access pdfFiller and search for the 'Prior Authorization for Adjunct Request Form' to locate the document you need.
-
2.Open the form by clicking on it to launch the editing interface.
-
3.Before filling the form, gather essential information, including patient diagnosis codes, current approved services, and the provider's details.
-
4.Navigate through the document by clicking on fillable fields to input the required information for Member Information and Provider Information sections.
-
5.Use pdfFiller's tools to select options or checkboxes where applicable for the Authorization Request section.
-
6.Review all entries diligently to ensure accuracy and completeness of the details provided in each section.
-
7.Once complete, save your work frequently to avoid losing any information during the process.
-
8.After finalizing the form, use pdfFiller’s options to download, print, or submit the form electronically through the platform.
Who is eligible to use the Prior Authorization for Adjunct Request Form?
Healthcare providers who wish to request authorization for mental health outpatient services can use this form. It's designed for professionals involved in patient care, including social workers and therapists.
Are there specific deadlines for submitting this form?
Submission deadlines may vary based on the insurance provider. It's best to check with the relevant insurance company for any specific time-sensitive requirements associated with prior authorizations.
How can I submit the completed form?
You can submit the completed Prior Authorization for Adjunct Request Form via pdfFiller by downloading it for mailing or using electronic submission methods provided by your insurance company.
What supporting documents are required with this form?
When submitting the Prior Authorization for Adjunct Request Form, include any relevant medical records, previous treatment notes, and a copy of the current approved services to strengthen the request.
What common mistakes should I avoid when filling out this form?
Ensure all required fields are filled out accurately, including diagnosis codes and provider information. Omitting critical information or errors in coding can lead to delays or denials in authorization.
How long does it take to process the authorization request after submission?
Processing times for prior authorization requests can vary by insurance company. Generally, it may take anywhere from a few days to a couple of weeks. Check with the insurance provider for their specific timelines.
What should I do if my request for authorization is denied?
If your authorization request is denied, review the denial letter for reasons and gather additional supporting documentation. You can then appeal the decision by following your insurance provider's appeal process.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.