Last updated on Mar 7, 2026

Get the free ssm health prior authorization
Show details
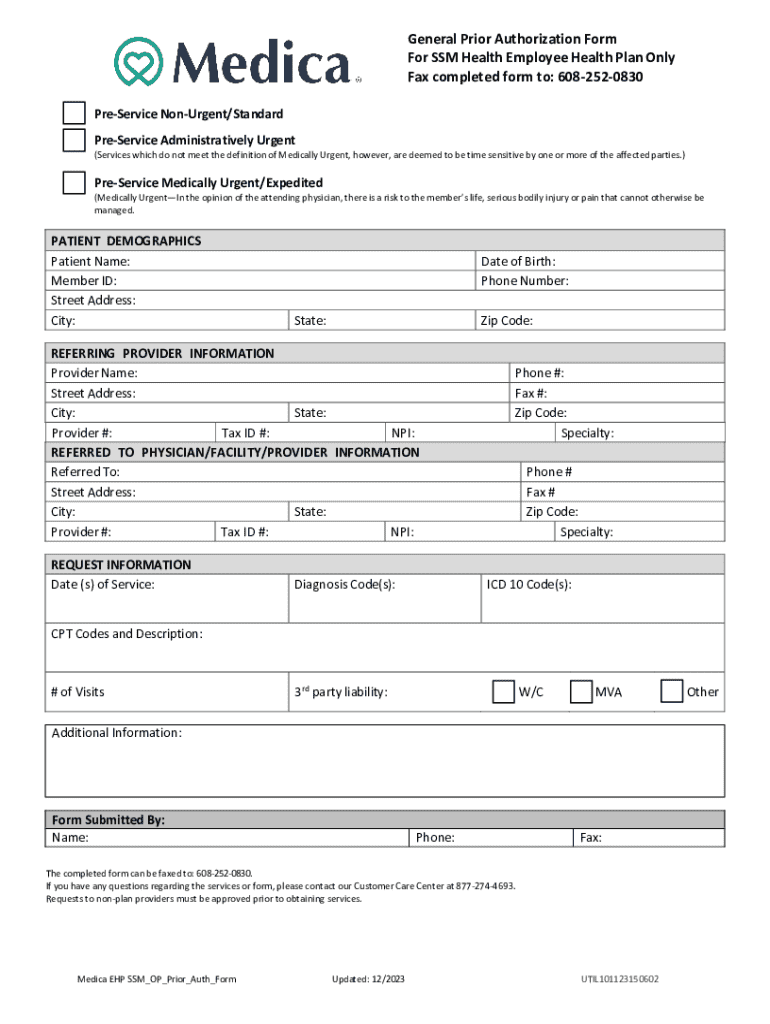
General Prior Authorization Form For SSM Health Employee Health Plan Only Fax completed form to: 6082520830 PreService NonUrgent/Standard PreService Administratively Urgent(Services which do not meet
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is ssm health prior authorization
The SSM Health Prior Authorization Form is a pre-authorization document used by SSM Health Employee Health Plan members to request authorization for medical services.
pdfFiller scores top ratings on review platforms




Who needs ssm health prior authorization?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to ssm health prior authorization
What is the SSM Health Prior Authorization Form?
The SSM Health Prior Authorization Form serves a crucial role in healthcare services by facilitating the authorization of medical procedures for SSM Health Employee Health Plan members. This form is essential for members seeking pre-service authorization.
To complete the SSM Health Prior Authorization Form, members must provide information such as patient demographics, service details, and medical codes. This ensures that necessary approvals are obtained before receiving medical services.
Purpose and Benefits of the SSM Health Prior Authorization Form
The primary purpose of the SSM Health Prior Authorization Form is to streamline the process for pre-service authorizations for medical services. By utilizing this form, healthcare providers can efficiently request authorizations, ensuring smoother patient care pathways.
The benefits extend beyond just patients; healthcare providers gain assurance of timely service approvals, which can enhance the overall quality of care. Moreover, submitting the form promptly is vital for securing necessary authorizations in a timely manner.
Who Needs the SSM Health Prior Authorization Form?
This form is specifically required for SSM Health Employee Health Plan members who are seeking medical services that necessitate prior authorization. It is crucial for patients who fit certain criteria, such as those undergoing specific procedures or treatments that are regulated.
There may be exceptions or specific cases where different requirements apply, particularly with regard to regulations in Wisconsin. Understanding these nuances can aid members in correctly navigating the authorization process.
How to Fill Out the SSM Health Prior Authorization Form Online
Filling out the SSM Health Prior Authorization Form online is a straightforward process. Members should start by entering critical information in the designated fields, including 'Patient Name', 'Provider Information', and relevant service dates.
Utilizing tools available through pdfFiller can enhance the experience by simplifying the completion process. Members should pay particular attention to accuracy, ensuring that diagnosis codes and CPT codes are correctly entered to avoid delays.
Common Errors and How to Avoid Them
When completing the SSM Health Prior Authorization Form, it's important to be aware of potential pitfalls. Common mistakes include entering an incorrect member ID, leaving required fields blank, or failing to provide necessary signatures.
To avoid these issues, users should meticulously validate their information before submission. Implementing a review process to double-check all entries can significantly reduce the chances of complications arising due to inaccurate data.
Submission Methods for the SSM Health Prior Authorization Form
Completed SSM Health Prior Authorization Forms can be submitted through various methods. Members may choose to fax the form or utilize online submission via pdfFiller.
For those submitting via fax, detailed instructions, including the fax number, should be followed carefully. It's also critical to be aware of any deadlines associated with the submission to facilitate prompt processing.
What Happens After You Submit the SSM Health Prior Authorization Form?
After submitting the SSM Health Prior Authorization Form, members can anticipate a review period during which the authorization request is processed. Understanding potential timelines for approval can help set appropriate expectations.
Members should also be informed on how to check the status of their requests, and it’s beneficial to know the possible outcomes, such as approval or rejection, along with the necessary next steps for each scenario.
Security and Compliance with the SSM Health Prior Authorization Form
When submitting the SSM Health Prior Authorization Form, members can rest assured that their information is handled securely. Compliance with regulations such as HIPAA and GDPR underscores the importance of privacy and data protection.
pdfFiller employs encryption and other security measures to safeguard sensitive patient information, ensuring that users can fill out the form confidently, knowing their data is protected.
Get Started with pdfFiller to Complete the SSM Health Prior Authorization Form
Using pdfFiller to complete the SSM Health Prior Authorization Form offers numerous advantages. The platform’s features simplify the filling and signing processes, making it user-friendly for all members.
With a commitment to document security and an intuitive interface, pdfFiller qualifies as a reliable tool for handling sensitive healthcare forms, ensuring both accessibility and security throughout the entire process.
How to fill out the ssm health prior authorization
-
1.Access the SSM Health Prior Authorization Form on pdfFiller by visiting the provided link and logging in to your account.
-
2.Once the form is visible, review the layout and available fields. Familiarize yourself with the sections that will need completion.
-
3.Before you begin filling out the form, gather essential information such as patient demographics, provider details, service dates, diagnosis codes, and CPT codes.
-
4.Utilize the fillable fields for Patient Name, Date of Birth, and Member ID. Click on each section to input the required details accurately.
-
5.In the 'Provider Information' section, enter the referring and referred provider’s names, including contact information if required.
-
6.Fill in the 'Request Information' by specifying the service type and the expected dates for each requested service.
-
7.Review all entered information to ensure accuracy and that nothing is left uncompleted. Correct any mistakes or omitted data before proceeding.
-
8.Once satisfied with the details entered, utilize pdfFiller’s options to save the form. You can also download it to your device.
-
9.To submit, confirm the fax number is correct and then fax the completed form to 608-252-0830 for authorization. Check the submission confirmation process as needed.
Who is eligible to use the SSM Health Prior Authorization Form?
The SSM Health Prior Authorization Form is specifically for members of the SSM Health Employee Health Plan seeking pre-service authorizations for their healthcare needs.
What information is required to complete this form?
You will need patient demographics, referring and referred provider information, diagnosis codes, CPT codes, and service dates to fill out the SSM Health Prior Authorization Form accurately.
How do I submit the completed form?
After completing the SSM Health Prior Authorization Form, fax it to 608-252-0830. It's essential to verify all provided information is correct before submission to avoid delays.
Are there any common mistakes to avoid when filling out this form?
Common mistakes include missing vital fields such as Member ID or service dates, and inaccuracies in diagnosis or CPT codes. Always review the form thoroughly before submitting.
What is the processing time for an authorization request?
Processing times for the SSM Health Prior Authorization can vary. Typically, allow a few business days for approval, and ensure to account for this before scheduling services.
Are supporting documents required with the SSM Health Prior Authorization Form?
Yes, additional documentation like medical records or referral letters may be required. Confirm with your healthcare provider to ensure you have all necessary supporting documents ready.
What should I do if I encounter issues with pdfFiller while completing the form?
If you experience issues on pdfFiller, ensure your browser is up-to-date, clear your cache, or contact pdfFiller support for assistance with technical difficulties.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.