Last updated on Mar 10, 2026

Get the free coverage determination request form
Show details
COVERAGE DETERMINATION REQUEST FORM EOC ID: EOC IDCOMM_Nonformulary Exception Phone: 8333201824 Fax back to: 8663511617 SlateRx manages the pharmacy drug benefit for your patient. Certain requests
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is coverage determination request form
The Coverage Determination Request Form is a healthcare document used by prescribers to request approval for non-formulary medications for their patients.
pdfFiller scores top ratings on review platforms




Who needs coverage determination request form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to coverage determination request form
What is the Coverage Determination Request Form?
The Coverage Determination Request Form is a key document in healthcare, utilized mainly by healthcare providers to request coverage for non-formulary medications. It plays an essential role in ensuring that patients have access to necessary treatments that their insurance plans might not automatically cover.
This form defines "non-formulary medications" as those drugs not included on a specific insurance plan's preferred drug list. A coverage determination is critical in cases where a patient requires a medication not readily accessible through their plan, as it may facilitate improved patient care and medication adherence.
Purpose and Benefits of the Coverage Determination Request Form
The Coverage Determination Request Form provides significant advantages for both healthcare providers and patients. For healthcare providers, this form streamlines the process of obtaining necessary approvals, thereby reducing delays in patient treatment.
For patients, completing this medication request form ensures they gain access to vital medications that may be essential for managing their health conditions effectively. This access can significantly enhance patient outcomes and overall satisfaction with their healthcare experience.
Key Features of the Coverage Determination Request Form
This form includes several critical components that must be filled out accurately. Key features comprise the patient's and prescriber's names, member or subscriber numbers, and detailed medication information.
Additionally, it requires the prescriber’s signature, which validates the request, along with necessary patient diagnosis details, ensuring that the submission conforms to the criteria outlined by insurance policies.
Who Needs the Coverage Determination Request Form?
Moreover, pharmacy benefits managers play a vital role in processing these requests, evaluating each one to determine if the medication should be covered based on medical necessity. Certain scenarios, such as when a patient requires a drug that is not included in their insurance formulary, exemplify the need for this form.
How to Fill Out the Coverage Determination Request Form Online (Step-by-Step)
Filling out the Coverage Determination Request Form online can be straightforward if you follow these steps:
-
Access the form through your healthcare provider portal or pdfFiller.
-
Begin by entering patient information, such as their name and member number.
-
Complete fields regarding the prescriber, including their name and contact details.
-
Detail the medication being requested along with the dosage and reason for use.
-
Include patient diagnosis information and relevant ICD-10 codes.
-
Finally, add the prescriber’s signature to validate the request before submission.
Common Errors and How to Avoid Them
When completing the Coverage Determination Request Form, several errors often occur that can lead to delays. Common mistakes include incomplete fields, incorrect patient information, and failing to provide an appropriate diagnosis.
To avoid these issues, carefully review the form for accuracy and ensure all required signatures are included. Cross-checking the details before submission can help mitigate delays and ensure a smoother approval process.
How to Submit the Coverage Determination Request Form
Submitting the Coverage Determination Request Form can be done through various channels. Providers typically have the option to fax the completed form to the specified insurance provider’s fax number.
It's also crucial to be aware of any submission deadlines and processing times that pertain to the request. Adhering to these timelines can help ensure prompt review and approval of the medication request.
What Happens After You Submit the Coverage Determination Request Form?
Once the Coverage Determination Request Form is submitted, it undergoes a review process by the insurance company. During this time, prescribers and patients can anticipate different outcomes based on the necessity and justification provided for the medication.
Patients and providers may track the status of their submission, often communicated through calls or online portals, to provide updates on approval or request for additional information.
Security and Compliance When Using the Coverage Determination Request Form
Maintaining security and compliance is paramount when using the Coverage Determination Request Form. Platforms like pdfFiller ensure that sensitive patient data is protected through robust measures, including 256-bit encryption and adherence to HIPAA and GDPR compliance.
Safeguarding sensitive information remains a top priority, as proper handling of such data is essential for preserving patient confidentiality and trust in healthcare providers.
Effortlessly Manage Your Coverage Determination Request Form with pdfFiller
Utilizing pdfFiller enhances the experience of managing your Coverage Determination Request Form. With its user-friendly interface, pdfFiller streamlines the process of filling out, editing, and submitting forms.
Key functionalities, such as eSigning, creating fillable forms, and secure document sharing, support healthcare providers in navigating the complexities of form submissions while ensuring compliance and security.
How to fill out the coverage determination request form
-
1.To access the Coverage Determination Request Form on pdfFiller, visit the site and search for the form using its name.
-
2.Once located, click on the form to open it in the pdfFiller interface, where you can begin editing.
-
3.Before starting, gather necessary information such as the patient's name, diagnosis, and ICD-10 codes, as well as medication details and previous treatments.
-
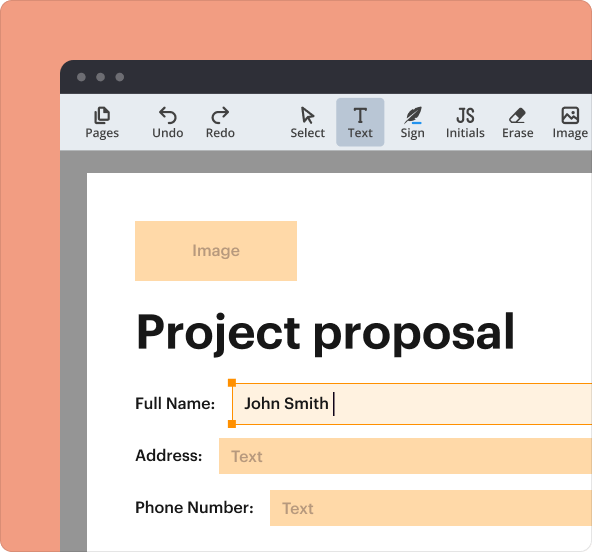
4.Begin filling in the form by clicking on each field and inputting the required information. Use the provided guidelines to ensure accuracy.
-
5.Make use of the toolbar to navigate between fillable fields and utilize any templates or instructions provided on the side.
-
6.Once you have completed all fields, take a moment to review the information entered for any inconsistencies or omissions.
-
7.Finalize the form by ensuring the prescriber signature is included, as it is required for submission.
-
8.After finalizing, save your progress by clicking the save option in pdfFiller. You can also download a copy for your records.
-
9.To submit the completed form, follow the submission instructions provided within pdfFiller, which may include faxing to a specified number.
Who is eligible to use the Coverage Determination Request Form?
Eligibility to use the Coverage Determination Request Form generally includes healthcare providers such as physicians and prescribers responsible for submitting requests for non-formulary medications on behalf of their patients.
What is the typical submission method for this form?
The Coverage Determination Request Form is typically completed and signed by the healthcare provider and then submitted via fax to the specified number for review by the insurance company.
What information do I need to gather before filling out the form?
Before filling out the Coverage Determination Request Form, you will need detailed information like the patient's diagnosis, ICD-10 codes, prescribed medication details, and any previous treatment attempts that support the request.
Are there any common mistakes to avoid when completing the form?
Common mistakes to avoid include failing to provide a prescriber signature, overlooking required fields, and not attaching necessary supporting documents that validate the request for medication approval.
How long does it take to process a Coverage Determination Request?
Processing times for a Coverage Determination Request can vary but typically range from a few days to a couple of weeks, depending on the insurance provider's review procedures.
What if my Coverage Determination Request is denied?
If your Coverage Determination Request is denied, you can appeal the decision by following the insurance company's appeal process, which often requires resubmission with additional documentation.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.