Last updated on Mar 10, 2026

Get the free prior authorization form
Show details
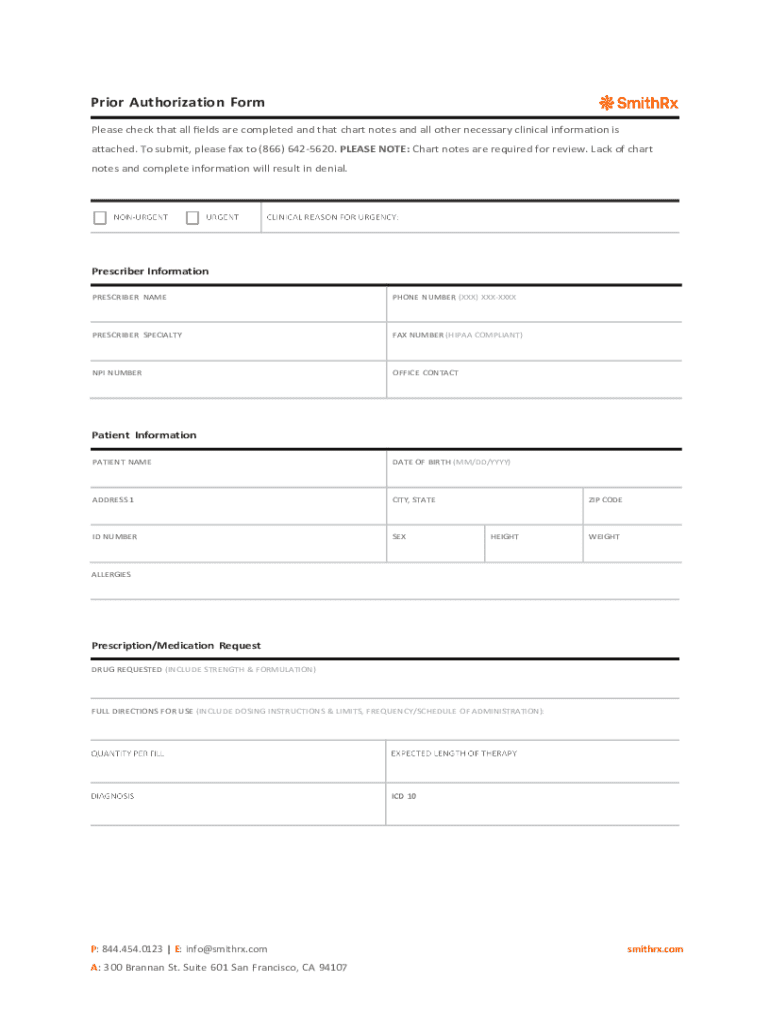
Prior Authorization Form Please check that all elds are completed and that chart notes and all other necessary clinical information is attached. To submit, please fax to (866) 6425620. PLEASE NOTE:
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is prior authorization form
The Prior Authorization Form is a medical consent document used by healthcare providers to request approval for prescription medications or treatments.
pdfFiller scores top ratings on review platforms




Who needs prior authorization form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to prior authorization form
What is the Prior Authorization Form?
The prior authorization form is a crucial document used by healthcare providers to request approval for necessary prescription medications and treatments. This healthcare authorization form plays a pivotal role in ensuring that patients receive appropriate care while complying with insurance requirements. By utilizing this medication request form, healthcare providers can effectively manage prescribed treatments and maintain adherence to regulatory standards.
Purpose and Benefits of the Prior Authorization Form
Healthcare providers use the prior authorization form to facilitate the approval process for certain medications. This streamline helps patients access required treatments promptly, which can lead to better health outcomes. The prescription approval form not only benefits patients but also assists prescribers by ensuring compliance with insurance policies and reducing the risk of denials.
Who Needs the Prior Authorization Form?
Key stakeholders involved in the prior authorization process include prescribers, healthcare providers, and patients. Typically, physicians, pharmacists, and specialists are responsible for submitting the prescriber information form. Situations that might necessitate the completion of a prior authorization form include specific drug therapies, repeat prescriptions, or treatments deemed non-standard.
How to Fill Out the Prior Authorization Form Online (Step-by-Step)
To complete the prior authorization form through a cloud-based PDF editor, follow these step-by-step instructions:
-
Access the form through your preferred platform.
-
Fill in the patient information fields thoroughly.
-
Provide the prescriber details, ensuring accuracy.
-
Attach any necessary clinical information documentation.
-
Review your entries for completeness and accuracy.
Be sure to include any relevant notes that may support the approval of the medication authorization form.
Common Errors and How to Avoid Them When Submitting the Prior Authorization Form
Many errors can occur during the submission of the prior authorization form, including incomplete information or incorrect patient details. To avoid these mistakes and their potential consequences, consider implementing the following measures:
-
Double-check all entries before submission.
-
Ensure that required supporting documents are attached.
-
Validate all clinical information for accuracy.
Additionally, reviewing the form with a second party can help catch errors that may have been overlooked.
Required Documents and Supporting Materials for Submission
When submitting the prior authorization form, it is crucial to include certain required documents to facilitate the approval process. These may consist of:
-
Patient medical records or history.
-
Previous treatment outcomes or notes.
-
Clarification of medical necessity.
Providing comprehensive clinical information will enhance the chances of a successful approval for the authorization process.
Submission Methods for the Prior Authorization Form
The prior authorization form can be submitted both electronically and via fax. For California residents, specific submission points may be designated. Ensure that you are aware of any potential fees or deadlines associated with the various submission methods to avoid delays in the approval process.
What Happens After You Submit the Prior Authorization Form?
Once the prior authorization form is submitted, the review process begins. It is essential to track the status of your submission, which typically includes waiting for feedback from the insurance provider regarding approval or denial. Common reasons for rejection might include lacking clinical justification or missing documentation, and addressing these issues promptly can improve future submissions.
How pdfFiller Can Simplify the Prior Authorization Process
pdfFiller offers a user-friendly solution for filling out and submitting the prior authorization form. With key capabilities such as editing, eSigning, and sharing completed forms, pdfFiller makes the process efficient and secure. The platform ensures the safety of sensitive patient information through 256-bit encryption and compliance with HIPAA and GDPR regulations.
Final Thoughts on Streamlining Your Prior Authorization Process
Utilizing pdfFiller can significantly enhance your experience with the prior authorization process, making documentation simpler and more efficient. Remain committed to ensuring compliance and proper use of the prior authorization form to secure the best possible care for patients.
How to fill out the prior authorization form
-
1.Access pdfFiller and search for the Prior Authorization Form to open it in the interface.
-
2.Review the form layout to familiarize yourself with the various fields and sections.
-
3.Gather necessary patient and prescriber information, including details such as patient history and clinician credentials before you start.
-
4.Click on each fillable field within the form to enter required details such as medication specifics and justification for the request.
-
5.Use the checkboxes to indicate any necessary options that apply to the patient's situation as per the requirements.
-
6.Ensure that supporting documentation, like chart notes, is ready to be uploaded as they are mandatory for approval.
-
7.Once all information is entered, review the form thoroughly for accuracy and completeness.
-
8.After finalizing the data, save the completed form as a PDF on pdfFiller for your records.
-
9.You can submit the form through fax directly from pdfFiller or download it for offline submission.
Who is eligible to use the Prior Authorization Form?
The Prior Authorization Form is primarily for licensed healthcare providers who prescribe medications. Patients can also be involved as they will provide input on their medical history and needs.
What supporting documents are required with the form?
Required supporting documents include detailed patient medical history, prescriber credentials, clinical justification, and any relevant chart notes to ensure proper review and approval.
How do I submit the Prior Authorization Form?
You can submit the Prior Authorization Form by faxing it directly after completion. You also have the option to download it and fax it manually or submit it through your healthcare institution's administrative methods.
What are common mistakes when filling out this form?
Common mistakes include omitting required information, forgetting to attach supporting documents, and failing to review the form for accuracy before submission. Make sure all fields are correctly filled out.
What is the processing time for the Prior Authorization Form?
Processing time varies depending on the insurance provider and their review policies, but it typically takes a few business days. Check with your insurance company for more specific timelines.
Is notarizing required for the Prior Authorization Form?
No, notarizing the Prior Authorization Form is not required, but ensure all information is accurate and complete prior to submission.
Can I save the form on pdfFiller for later use?
Yes, you can save the filled-out Prior Authorization Form as a PDF on pdfFiller, allowing you to edit or submit it later as needed.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.