Last updated on Mar 12, 2026

Get the free otezla prior authorization form
Show details
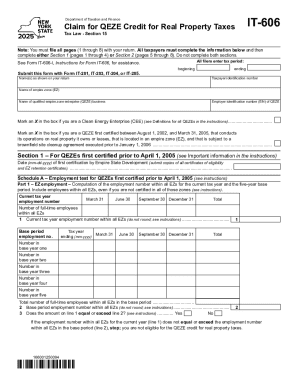
Blue Cross and Blue Shield of North Carolina (Blue Cross NC) | Healthy Blue | Healthy Blue Care Together | MedicaidImmunomodulators: Prior Authorization Form Fax this form to 8443762318. Healthy Blue
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is otezla prior authorization form
The Otezla Prior Authorization Form is a medical consent document used by Blue Cross and Blue Shield of North Carolina members to request prior authorization for the immunomodulator Otezla.
pdfFiller scores top ratings on review platforms




Who needs otezla prior authorization form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to otezla prior authorization form
What is the Otezla Prior Authorization Form?
The Otezla Prior Authorization Form is crucial for members seeking to obtain coverage for the immunomodulator Otezla through their Blue Cross and Blue Shield plans in North Carolina. This form is essential in requesting permission for medication prior to its prescription and helps ensure patients receive comprehensive care tailored to conditions like psoriasis and psoriatic arthritis.
Prior authorization helps manage treatment plans effectively by requiring healthcare providers to submit detailed patient information and clinical justifications. This step is vital to confirm that patients adhere to the necessary medical guidelines when utilizing the Otezla medication.
Purpose and Benefits of the Otezla Prior Authorization Form
The form offers several advantages, particularly for members of Blue Cross and Medicaid. Utilizing the Otezla Prior Authorization Form ensures access to necessary treatments while maintaining quality control over prescribed medications.
By requiring prior authorization, treatment plans for conditions such as psoriasis, psoriatic arthritis, and Behcet’s disease can be better managed, leading to improved patient outcomes and a more streamlined healthcare process.
Who Needs the Otezla Prior Authorization Form?
The Otezla Prior Authorization Form must be filled out by specific member groups including those diagnosed with conditions requiring this medication. Eligibility criteria typically include membership with Blue Cross and the necessity of using Otezla as part of their treatment plan.
Members can review their eligibility and confirm the need for prior authorization based on their prescribed treatments and insurance coverage. This form is particularly relevant for individuals suffering from psoriasis or psoriatic arthritis.
How to Fill Out the Otezla Prior Authorization Form Online (Step-by-Step)
To ensure successful completion of the Otezla Prior Authorization Form online, follow these steps:
-
Access the PDF version of the form on the pdfFiller platform.
-
Fill out the patient and prescriber information accurately.
-
Detail the medication and specified conditions that require treatment.
-
Provide any additional clinical documentation necessary to support the authorization request.
-
Review all filled fields before submission for accuracy.
Completing this form correctly is vital for a smooth authorization process, so pay close attention to each section.
Common Errors and How to Avoid Them When Completing the Otezla Prior Authorization Form
Several frequent mistakes can occur while filling out the Otezla Prior Authorization Form, and avoiding them can lead to quicker approval. Common errors include:
-
Incomplete or missing patient information.
-
Incorrect medication details or dosages listed.
-
Failure to include necessary clinical documentation.
By ensuring all information is accurate and complete, members can contribute to a faster review process, helping them receive essential treatments without unnecessary delays.
Submission Methods and What Happens After You Submit the Otezla Prior Authorization Form
Members can submit their completed Otezla Prior Authorization Form through various methods, such as faxing it to the designated number provided by their insurer. Upon submission, members should expect a confirmation of receipt and tracking updates regarding the status of their authorization request.
Timely submission is crucial as it affects the overall turnaround time for approval, and members should familiarize themselves with the potential outcomes of their requests to avoid any surprises in their treatment journey.
Security and Compliance When Using the Otezla Prior Authorization Form
Handling sensitive health information requires strict security measures to protect patient privacy and compliance with regulations. The pdfFiller platform employs advanced security protocols, including 256-bit encryption, to ensure data protection during the completion and submission of the Otezla Prior Authorization Form.
Additionally, pdfFiller adheres to HIPAA and GDPR standards, assuring users that their sensitive information remains secure throughout the document management process.
How pdfFiller Can Help You With the Otezla Prior Authorization Form
Utilizing pdfFiller offers numerous benefits when managing the Otezla Prior Authorization Form. The platform allows users to edit, fill, and sign the form effortlessly while providing features such as eSignatures, cloud storage, and functionality for easy document sharing.
These helpful tools streamline the submission process, making it easier for members to navigate through their healthcare documentation without unnecessary stress.
Sample or Example of a Completed Otezla Prior Authorization Form
Here is an example of a filled-out Otezla Prior Authorization Form to guide users through the submission process. The sample highlights the necessary details needed in each part of the form, ensuring clarity and understanding for those completing it.
Each section of this form includes fields capturing patient demographics, medication specifics, and clinical justification, all of which are necessary for full authorization consideration.
Next Steps: Getting Your Otezla Prior Authorization Approved
Once the Otezla Prior Authorization Form has been completed and submitted, users are encouraged to follow up as needed to ensure approval. pdfFiller’s services can aid in managing this process smoothly and efficiently.
Timely prior authorization not only facilitates access to medication but also plays a crucial role in the effective management of treatment plans, supporting overall patient health.
How to fill out the otezla prior authorization form
-
1.To start, access the Otezla Prior Authorization Form on pdfFiller by searching the form name in their search bar or browsing through healthcare forms.
-
2.Once open, review the form layout. Familiarize yourself with the sections, including patient, prescriber, and drug details.
-
3.Before you fill in the form, gather all necessary information, such as patient identification details, prescriber contact information, and specific medical conditions related to Otezla.
-
4.Begin filling in the fields systematically, entering the patient's information in the designated areas. Use the dropdowns where applicable to enhance accuracy.
-
5.Next, provide the prescriber’s information in the required fields. Ensure all contact details are accurate to facilitate communication.
-
6.Continue to input drug-related information, ensuring you specify the dosage and frequency. Double-check for consistency with the treatment plan.
-
7.As you complete each section, utilize the checkbox options and fill in clinical information to support the request for authorization. Review the instructions provided on the form for accurate completion.
-
8.After you have filled out all necessary fields, review your entries for accuracy. Make sure all required sections are complete to avoid processing delays.
-
9.Once you are confident that the form is filled out correctly, save your progress. Use the save function on pdfFiller to create a digital copy of your completed form.
-
10.Finally, download the completed form for your records. If required, submit it according to the specified submission method, typically by fax, to the designated number provided.
Who is eligible to use the Otezla Prior Authorization Form?
Members of Blue Cross and Blue Shield of North Carolina’s Medicaid plans who require Otezla for conditions like psoriasis or psoriatic arthritis are eligible to use this form.
What is the processing time for the Otezla Prior Authorization request?
Processing times can vary, but typically authorization requests are reviewed within 3-5 business days. It's advisable to submit the form well in advance of treatment needs.
How should I submit the completed Otezla Prior Authorization Form?
The completed form should be faxed to the designated number specified on the form. Ensure all required fields are filled to prevent submission delays.
What supporting documents do I need to include with the form?
While supporting documents are not always required, it's beneficial to include relevant medical records or treatment histories that support the prior authorization request.
Are there common mistakes to avoid when filling out this form?
Common mistakes include leaving fields blank, providing inaccurate patient or prescriber information, and not checking if all required sections are completed before submission.
Can I modify the Otezla Prior Authorization Form after I have filled it out?
Yes, you can modify the form if you haven't submitted it yet. Simply access it again on pdfFiller, make the necessary changes, and save your updated version.
What happens if my authorization request is denied?
If the request is denied, the insurance provider typically sends a denial letter outlining the reasons. You may appeal the decision by addressing the stated reasons and resubmitting the necessary information.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.