Last updated on Oct 22, 2015

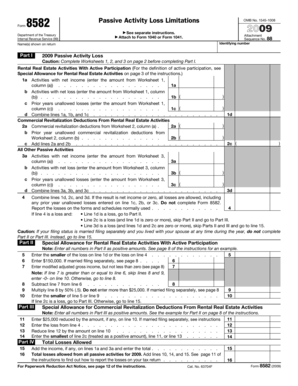
Get the free Simplified Billing or ECLIPSE Adjustment Claim
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Adjustment Claim Form
The Simplified Billing or ECLIPSE Adjustment Claim form is a medical document used by Australian health insurers and medical providers to amend previously processed claims with new information.
pdfFiller scores top ratings on review platforms




Who needs Adjustment Claim Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Adjustment Claim Form
What is the Simplified Billing or ECLIPSE Adjustment Claim?
The Simplified Billing or ECLIPSE Adjustment Claim form serves a crucial role in the Australian healthcare system. This form is primarily utilized by private health insurers, medical providers, and billing agents seeking to amend previously processed claims. It encompasses vital information such as patient details and reasons for adjustments.
This form is instrumental in ensuring the accuracy and integrity of the billing process. It includes fields for key data, ensuring that all necessary information is captured to facilitate smooth claim adjustments.
Purpose and Benefits of the Simplified Billing or ECLIPSE Adjustment Claim
The primary purpose of the Simplified Billing or ECLIPSE Adjustment Claim form is to provide a straightforward mechanism for correcting billing information. This enhances the overall accuracy of claims processed by health insurers. Among its benefits, the form aids in reducing the incidence of billing errors, which can adversely affect revenue cycles.
This claim adjustment process proves beneficial for private health insurers, billing agents, and healthcare providers. Timely amendments ensure that claims are settled appropriately, thus maintaining cash flow and operational efficiency.
Key Features of the Simplified Billing or ECLIPSE Adjustment Claim
-
Includes fields for the patient's full name, Medicare provider number, and reason for the adjustment.
-
Required fields must be completed to ensure the form’s validity.
-
Supports necessary documentation, including the sender's signature and date.
The form is designed to facilitate quick and efficient adjustments to claims, making it easier for all stakeholders involved in the billing process.
Who Needs to Use the Simplified Billing or ECLIPSE Adjustment Claim?
The primary users of the Simplified Billing or ECLIPSE Adjustment Claim include medical providers, billing agents, and private health insurers. This form becomes essential in various scenarios, particularly when there's a need for correcting previously submitted claims.
Understanding who requires this form is crucial for its effective utilization, ensuring that all necessary claims adjustments are processed without delay.
When to File the Simplified Billing or ECLIPSE Adjustment Claim
Timeliness in submission is critical when filing the Simplified Billing or ECLIPSE Adjustment Claim. Submissions should be made promptly after the discovery of inaccuracies to avoid complications that may affect claims processing.
-
Ensure submission before applicable deadlines to prevent delays in payment.
-
Recognize the consequences of late submissions, as they can lead to claim denials.
How to Fill Out the Simplified Billing or ECLIPSE Adjustment Claim Online
Filling out the Simplified Billing or ECLIPSE Adjustment Claim online involves a detailed, field-by-field approach. Start by gathering all necessary information, including patient details and the reasons for adjustment, before initiating the form.
-
Ensure all required fields are filled accurately to prevent submission errors.
-
Be mindful of common mistakes, such as leaving fields blank or mislabeling information.
Submission Methods for the Simplified Billing or ECLIPSE Adjustment Claim
Once completed, the Simplified Billing or ECLIPSE Adjustment Claim can be submitted via fax. Familiarity with state-specific rules regarding submission is essential for compliance. Additionally, adhering to security measures when transmitting sensitive information ensures the protection of patient data.
What Happens After You Submit the Simplified Billing or ECLIPSE Adjustment Claim?
Upon submission, the claim undergoes a thorough review process by health insurers. Tracking the status of the claim is possible, allowing users to remain informed throughout the process.
-
Common rejection reasons can include incomplete fields or insufficient documentation.
-
Understanding how to address and remedy these issues is vital for successful claim adjustments.
Security and Compliance Considerations for the Simplified Billing or ECLIPSE Adjustment Claim
Data security and compliance are paramount when handling the Simplified Billing or ECLIPSE Adjustment Claim. Various safety measures are in place to protect sensitive information, ensuring that submissions adhere to stringent standards.
This includes compliance with regulations such as HIPAA and GDPR, affirming the commitment to privacy and data protection in the management of patient information.
Get Started with pdfFiller for Your Simplified Billing or ECLIPSE Adjustment Claim
pdfFiller significantly simplifies the process of filling out the Simplified Billing or ECLIPSE Adjustment Claim. The platform provides users with secure, efficient online tools for document management, making the form-completion process straightforward and reliable.
Exploring the features of pdfFiller allows users to enhance their experience, ensuring that all required adjustments are made seamlessly.
How to fill out the Adjustment Claim Form
-
1.Access the Simplified Billing or ECLIPSE Adjustment Claim form on pdfFiller by searching its name in the template library or by navigating to the link provided.
-
2.Once the form is open, use the pdfFiller interface to navigate each section using the intuitive toolbar.
-
3.Before completing the form, gather necessary information including the patient’s full name, their Medicare provider number, and any previous claim identification numbers.
-
4.Fill in each field accurately, ensuring to provide detailed reasons for adjustment in the designated area.
-
5.Review all entries for accuracy and completeness. Utilize pdfFiller’s review tools to check for any missing information.
-
6.Once satisfied, finalize the form by saving it within pdfFiller. You can also download it in various formats for your records.
-
7.To submit, follow the instructions provided on the form for faxing it to the Simplified Billing Coordinator in your relevant state or territory.

Who is eligible to use the Simplified Billing or ECLIPSE Adjustment Claim form?
Private health insurers, billing agents, and healthcare providers in Australia are eligible to use this form to adjust previously submitted claims.
What documents are required when submitting this form?
While the form itself is the primary document required, gather any related claim information, such as previous claims and patient details, to help substantiate your request.
What are the deadlines for submitting the adjustment claim?
To ensure timely processing, submit your adjustment claim as soon as you identify discrepancies, ideally before any claim-related deadlines set by your health insurer.
How can I submit the Simplified Billing or ECLIPSE Adjustment Claim form?
Submit the completed form by fax to the Simplified Billing Coordinator in your relevant state or territory, as indicated in the instructions provided with the form.
What common mistakes should I avoid when filling out this form?
Ensure that all required fields are completed, especially patient details and reasons for adjustment. Double-check for accuracy to avoid processing delays.
How long does it take to process my adjustment claim?
Processing times can vary based on the insurer; however, expect a typical turnaround of 2-4 weeks after submission for review and adjustments.
What should I do if my claim adjustment is denied?
If your adjustment claim is denied, review the denial reasons provided by your insurer and consider submitting additional documentation or a follow-up claim for reconsideration.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.