Last updated on Oct 23, 2015

Get the free Prolia Prior Authorization Request Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prolia Authorization Form
The Prolia Prior Authorization Request Form is a medical document used by healthcare providers to request coverage for the medication Prolia.
pdfFiller scores top ratings on review platforms




Who needs Prolia Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prolia Authorization Form
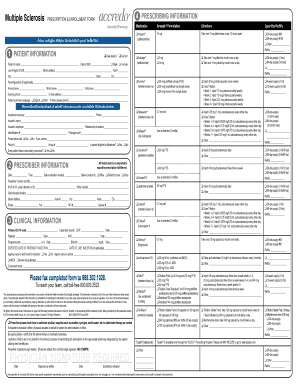
What is the Prolia Prior Authorization Request Form?
The Prolia Prior Authorization Request Form is essential for healthcare providers seeking medication coverage for Prolia. This form plays a pivotal role in securing insurance reimbursement for patients requiring this specific treatment. It must be completed with meticulous detail, as it requires the prescriber’s signature and several specific pieces of information to meet the criteria set by insurance companies.
Purpose and Benefits of the Prolia Prior Authorization Request Form
The primary purpose of the Prolia Prior Authorization Request Form is to streamline the process of obtaining medication coverage. By securing prior authorization, healthcare providers can facilitate patient access to necessary treatments efficiently. This process can lead to crucial cost savings for both patients and healthcare providers, decreasing the financial burden associated with medication costs.
Who Needs the Prolia Prior Authorization Request Form?
This form is primarily used by healthcare providers who prescribe Prolia. Eligible patients, typically those dealing with osteoporosis and other related conditions, are the primary beneficiaries of this authorization process. A strong relationship between the prescriber and the patient is vital for ensuring the form is filled out accurately and comprehensively.
How to Fill Out the Prolia Prior Authorization Request Form Online
Filling out the Prolia Prior Authorization Request Form online can be straightforward. Here is a step-by-step guide:
-
Access the form through your pdfFiller account.
-
Complete the key fields, paying special attention to medical history and diagnostic codes.
-
Review the details for accuracy to minimize the risk of rejection.
Field-by-Field Instructions for the Prolia Prior Authorization Request Form
When completing the Prolia Prior Authorization Request Form, focus on the following fields:
-
Patient demographics, which include name, date of birth, and insurance details.
-
Medical history, ensuring that all relevant conditions and past treatments are accurately listed.
-
Prescriber information, which requires precise identification of the prescribing physician.
Be aware of common errors in each field and ensure accurate diagnostic codes are provided to facilitate the approval process.
Submission Methods and Delivery
Upon completing the Prolia Prior Authorization Request Form, there are several options for submission to Scott & White Prescription Services:
-
Fax the completed form directly to the designated number.
-
Email the form if this method is supported by the service.
Ensure that you follow any specific submission instructions, as these may vary, and be aware of the timeline for receiving confirmations regarding your submission.
What Happens After You Submit the Prolia Prior Authorization Request Form?
After submitting the Prolia Prior Authorization Request Form, Scott & White Prescription Services will initiate a review process. Notifications regarding approval or denial are typically communicated within a specified timeline. If the request is denied, the prescriber and patient should be prepared to follow the appeals process to contest the decision and seek coverage.
Security and Compliance When Using the Prolia Prior Authorization Request Form
When submitting the Prolia Prior Authorization Request Form online, it is critical to understand the security measures in place. With pdfFiller, data is protected via 256-bit encryption, ensuring compliance with HIPAA regulations. Users can take additional steps to guarantee their sensitive information remains secure throughout the submission process.
Final Steps: Using pdfFiller to Complete Your Prolia Prior Authorization Request Form
Utilizing pdfFiller to complete your Prolia Prior Authorization Request Form can significantly enhance the efficiency of the process. The platform offers features such as eSigning and easy document editing, streamlining the completion of the form. Remember to ensure all necessary fields are accurately filled out for the best possible outcome.
How to fill out the Prolia Authorization Form
-
1.Access the Prolia Prior Authorization Request Form on pdfFiller by navigating to the provided link or searching for the form title.
-
2.Once the form is open, review the instructions and familiarize yourself with the layout, including text fields and checkboxes provided.
-
3.Gather the necessary information such as patient details, prescriber information, medical history, and diagnostic codes before starting to fill out the form.
-
4.Begin completing the text fields with accurate details, ensuring that all required patient information is provided.
-
5.Navigate through the form using the tab key or mouse to enter information smoothly, checking each section as you go based on the requirements listed.
-
6.Ensure you have the prescriber's signature at the designated area by initiating a signature field within pdfFiller's interface, if needed.
-
7.Review the entire form for any inaccuracies or missing information, and confirm that all sections are fully completed.
-
8.Finalize the form by clicking the save button located in the top right corner of the pdfFiller interface.
-
9.Download the completed form to your device or directly submit it to Scott & White Prescription Services through the upload feature on pdfFiller.

Who is eligible to use the Prolia Prior Authorization Request Form?
The Prolia Prior Authorization Request Form is intended for use by healthcare providers who prescribe Prolia for patients. This includes doctors, nurses, and authorized staff members involved in patient care.
What information is needed to complete the form?
To complete the Prolia Prior Authorization Request Form, you will need patient information, prescriber contact details, medical history, and specific diagnostic codes required for authorization.
How should the completed form be submitted?
Once completed and signed, the Prolia Prior Authorization Request Form should be faxed to Scott & White Prescription Services for review. Ensure you have the correct fax number before sending.
Are there any supporting documents required with the form?
Typically, no additional documents are required beyond the information filled in the Prolia Prior Authorization Request Form. However, if specific clinical information is needed, it may be attached to support the request.
What are common mistakes to avoid when filling out this form?
Common mistakes include missing required fields, entering incorrect patient or prescriber information, and neglecting to include a signature. Always review the form carefully before submission.
How long does processing take for a prior authorization request?
Processing times can vary; however, it generally takes several business days for the insurance company to review and respond to the Prolia Prior Authorization Request Form.
Is there a specific timeframe to submit the form?
It's advised to submit the Prolia Prior Authorization Request Form as soon as the medication is prescribed to avoid delays, particularly if there are treatment timelines that must be adhered to.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.