Last updated on Oct 24, 2015

Get the free Mercy Care Plan Prior Authorization Form
We are not affiliated with any brand or entity on this form
Why pdfFiller is the best tool for your documents and forms
End-to-end document management
From editing and signing to collaboration and tracking, pdfFiller has everything you need to get your documents done quickly and efficiently.
Accessible from anywhere
pdfFiller is fully cloud-based. This means you can edit, sign, and share documents from anywhere using your computer, smartphone, or tablet.
Secure and compliant
pdfFiller lets you securely manage documents following global laws like ESIGN, CCPA, and GDPR. It's also HIPAA and SOC 2 compliant.

What is Prior Authorization Form
The Mercy Care Plan Prior Authorization Form is a healthcare document used by prescribers to request authorization for brand name drugs under Medicaid.
pdfFiller scores top ratings on review platforms




Who needs Prior Authorization Form?
Explore how professionals across industries use pdfFiller.
Comprehensive Guide to Prior Authorization Form
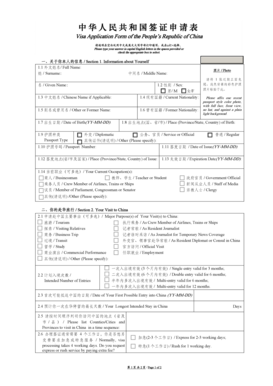
What is the Mercy Care Plan Prior Authorization Form?
The Mercy Care Plan Prior Authorization Form is a crucial document utilized within the Medicaid framework to facilitate the approval of brand name drugs. This form enables healthcare providers to formally request authorization to prescribe specific medications for their patients. Essential components of the form include patient information, detailed prescription details, and physician credentials. Properly completing these required fields ensures the request is processed efficiently, ultimately benefiting patient care.
Purpose and Benefits of the Mercy Care Plan Prior Authorization Form
Understanding the importance of the Mercy Care Plan Prior Authorization Form is vital for healthcare providers. This form streamlines the medication approval process by fostering clear communication between prescribers and payers. As a result, patients often experience improved health outcomes when the form is used correctly, leading to timely access to necessary medications. Enhanced efficiency in processing these requests is a key benefit, allowing providers to focus on patient care rather than paperwork.
Who Needs the Mercy Care Plan Prior Authorization Form?
This form is primarily used by prescribers who play a critical role in filling it out accurately. In addition to physicians, other healthcare professionals, such as nurse practitioners and physician assistants, may also require access to the form. In certain scenarios, patients might be directly involved in the submission process, particularly when clarifying details or ensuring they receive the medications their healthcare providers recommend. Ensuring that the correct individuals handle the form can lead to smoother approvals.
How to Fill Out the Mercy Care Plan Prior Authorization Form Online
Filling out the Mercy Care Plan Prior Authorization Form online is a straightforward process. Using a platform like pdfFiller, users can follow these steps:
-
Access the Mercy Care Plan Prior Authorization Form via pdfFiller.
-
Complete each section carefully, avoiding common pitfalls such as missing signatures or incomplete fields.
-
Ensure all required information, including patient and prescription details, is accurate before submission.
-
Submit the form electronically, following any specific methods outlined by Mercy Care Plan.
Common Errors and How to Avoid Them
When submitting the Mercy Care Plan Prior Authorization Form, several common errors may arise. To maintain accuracy and completeness, consider the following tips:
-
Double-check all filled fields for accuracy, particularly patient and prescription information.
-
Verify that required signatures are present and appropriately dated.
-
Review the completed form for clarity and ensure that all necessary documentation is included.
What Happens After You Submit the Mercy Care Plan Prior Authorization Form?
After submitting the Mercy Care Plan Prior Authorization Form, providers must understand the subsequent steps. The review process typically involves evaluating the submitted information and determining approval status. Providers should track application status regularly and be prepared for possible follow-up actions, especially if additional information is requested. Knowing how to handle potential rejections and resubmit the form is crucial for timely medication access.
Security and Compliance with the Mercy Care Plan Prior Authorization Form
Users should feel confident about the security of their sensitive data while using the Mercy Care Plan Prior Authorization Form. pdfFiller employs robust security measures, including 256-bit encryption, to safeguard healthcare documents. Additionally, the platform complies with HIPAA regulations and follows best practices for data protection. Understanding data retention policies related to submitted forms further enhances user confidence in the system.
How pdfFiller Enhances Your Experience with the Mercy Care Plan Prior Authorization Form
pdfFiller significantly improves the experience of filling out the Mercy Care Plan Prior Authorization Form. Key features of the platform include the ability to easily edit and fill out PDFs online, facilitating modifications without hassle. Users can also take advantage of secure eSigning, sharing options, and reliable storage for their completed documents, making the entire process more efficient and streamlined.
Sample or Example of a Completed Mercy Care Plan Prior Authorization Form
To assist users in accurately completing the Mercy Care Plan Prior Authorization Form, a sample completed form is provided. This example illustrates how each section should be filled out appropriately, emphasizing accuracy and attention to detail. Referencing this sample can serve as valuable guidance throughout the form-filling process.
Empower Your Form Submission with pdfFiller
Utilizing pdfFiller for the Mercy Care Plan Prior Authorization Form offers numerous benefits for users looking to streamline their submission process. The platform's user-friendly features are designed to enhance the overall experience, making it easier to fill out and submit the form with confidence. By starting the process on pdfFiller, users can ensure a hassle-free experience.
How to fill out the Prior Authorization Form
-
1.Access the Mercy Care Plan Prior Authorization Form on pdfFiller by searching in the template section or entering the form title in the search bar.
-
2.Once the form opens, familiarize yourself with the layout, noting the sections for drug details, patient information, and prescriber details.
-
3.Gather necessary information before starting, including the patient's full name, date of birth, Medicaid number, and any relevant medical history or diagnosis.
-
4.Complete the fields for drug information, including the generic name, prescription order, and dosage, ensuring accuracy to avoid processing delays.
-
5.Fill in the prescriber’s details carefully, including the name, contact information, and National Provider Identifier (NPI), as these will be essential for authorization.
-
6.Address any specific questions regarding patient experience with generic formulations in the designated areas of the form, providing thorough and precise responses.
-
7.Review the completed form for any missing information or errors to ensure all fields are filled out correctly.
-
8.Once confirmed, sign the form electronically using pdfFiller’s e-sign feature or by printing, signing, and scanning it back into pdfFiller.
-
9.To finalize, download the completed form in your preferred format or submit directly through pdfFiller if your healthcare plan allows electronic submissions.

Who is eligible to use the Mercy Care Plan Prior Authorization Form?
Healthcare providers, including physicians and prescribers, who are requesting authorization for brand name medications under Medicaid are eligible to use this form.
What information is required to complete the form?
Essential information includes the patient's details, diagnosis, medication information, and prescriber's credentials, ensuring all sections are accurately filled to facilitate processing.
How should I submit the form after completion?
Once the form is completed and signed, it must be faxed to the Mercy Care Plan for review and approval, following their specific submission guidelines.
Are there deadlines for submitting the prior authorization request?
While specific deadlines can vary, it is crucial to submit the authorization request as soon as possible after the prescription is made to avoid treatment delays.
What are common mistakes to avoid when completing the form?
Avoid leaving any sections blank, failing to provide complete patient information, or neglecting to sign the form. Double-check for accuracy to prevent processing issues.
How long does it take to process the prior authorization request?
Processing times can vary, but it typically takes a few business days. It is advisable to follow up if a decision is not received within the expected timeframe.
What happens if the authorization is denied?
If the authorization is denied, you will receive a notification detailing the reasons. You may appeal the decision by providing additional information supporting the need for the requested medication.
If you believe that this page should be taken down, please follow our DMCA take down process
here
.
This form may include fields for payment information. Data entered in these fields is not covered by PCI DSS compliance.